Abdominal and Pelvic Radiology — MCQs

On this page
Air in the biliary tract is seen in all of the following conditions except:
The "chain of lakes" appearance on imaging is characteristic of which of the following conditions?
Which radiological method is best for staging cervical carcinoma?
Carman's meniscus sign is diagnostic of –
Which of the following conditions is characterized by the presence of a central dot sign on CT scan?
A 69-year-old man with dysphagia is found to have a benign lesion on barium swallow. What should he be told regarding benign tumors and cysts of the esophagus?
The 'diamond sign' is radiographically observed in which of the following conditions?
A patient with a history of choledocholithiasis presents with elevated conjugated bilirubin. Ultrasound reveals a dilated biliary system up to the terminal pancreas. In case of suspicion of an ampullary obstructive calculus, which of the following investigations would be most sensitive?
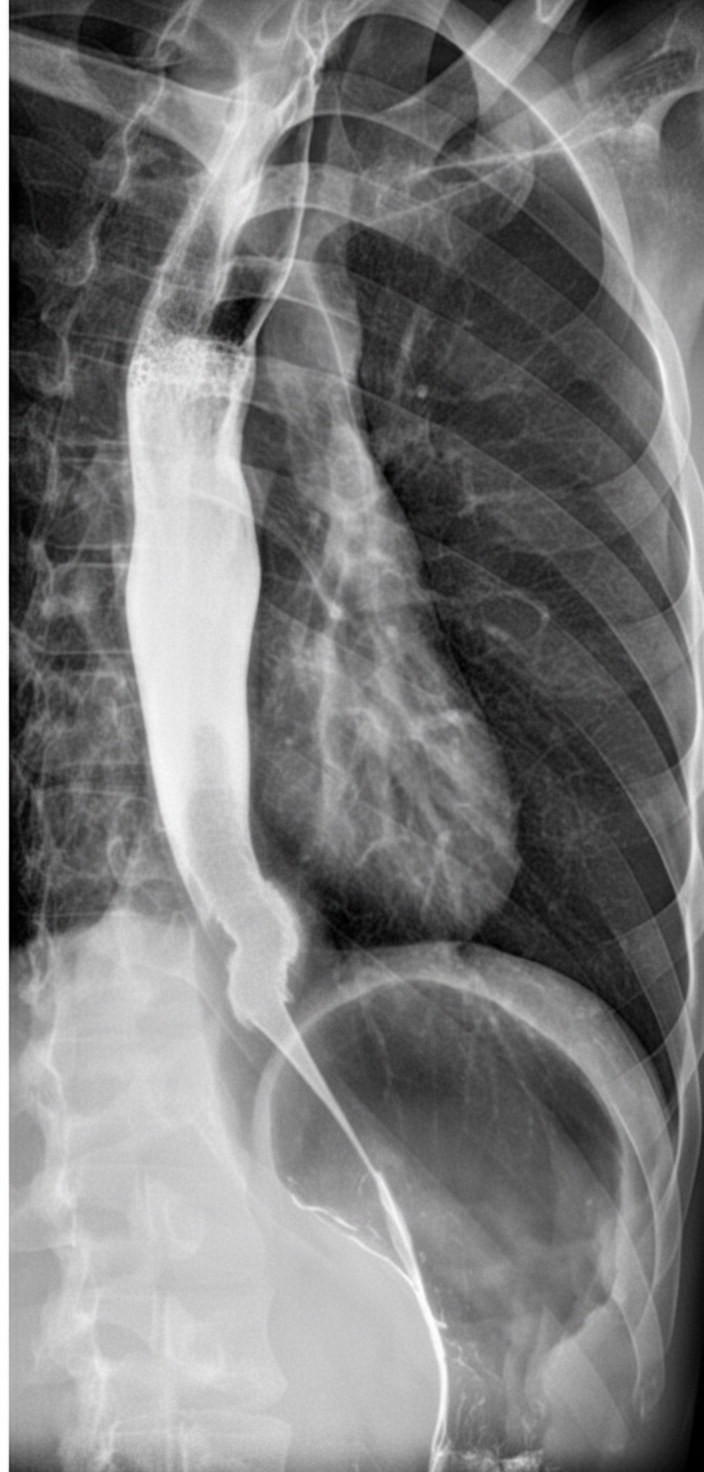
A barium swallow shows which of the following findings?
Endometriomas on ultrasound typically appear as?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
