Abdominal and Pelvic Radiology — MCQs

On this page
What is the term for the appearance of diverticulosis on a barium enema as depicted in the image?
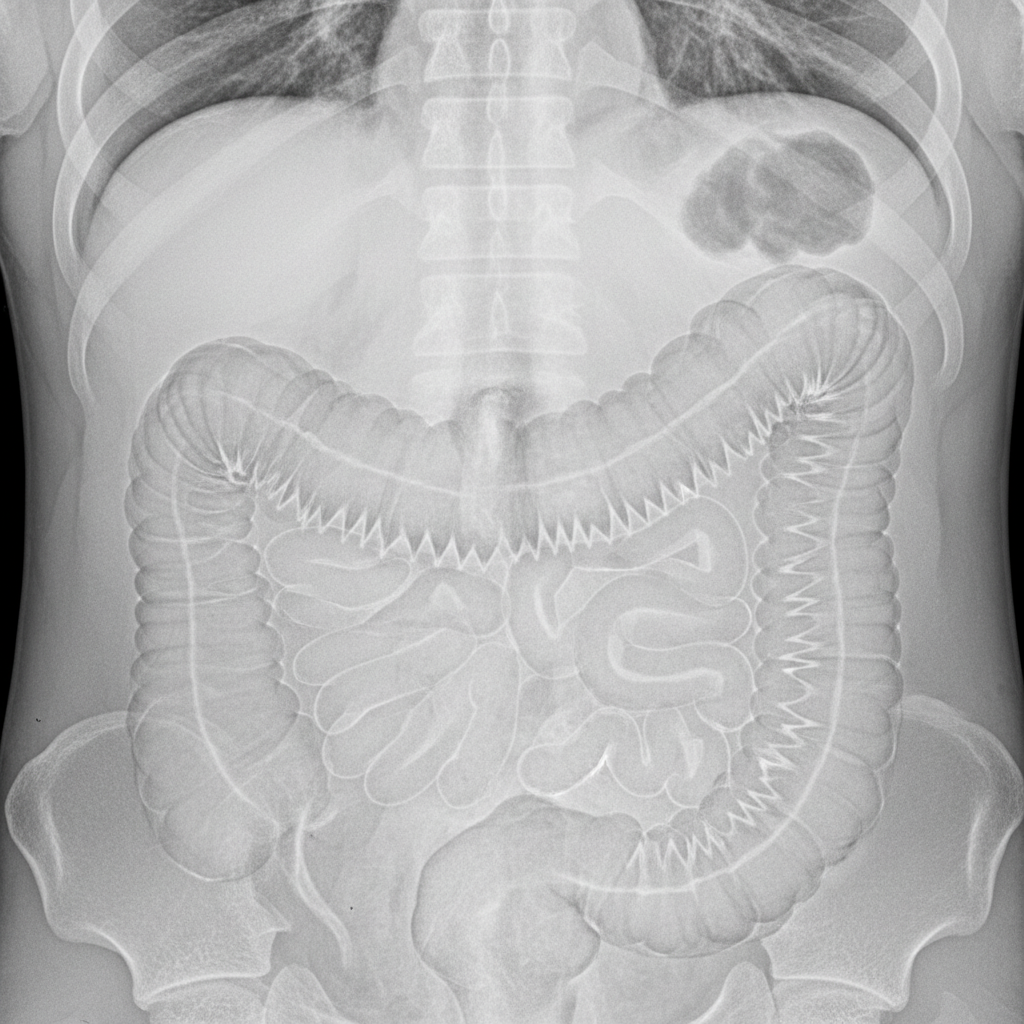
Tear drop bladder is seen in which of the following conditions?
An incidental finding on ultrasound abdomen is suggestive of which of the following?
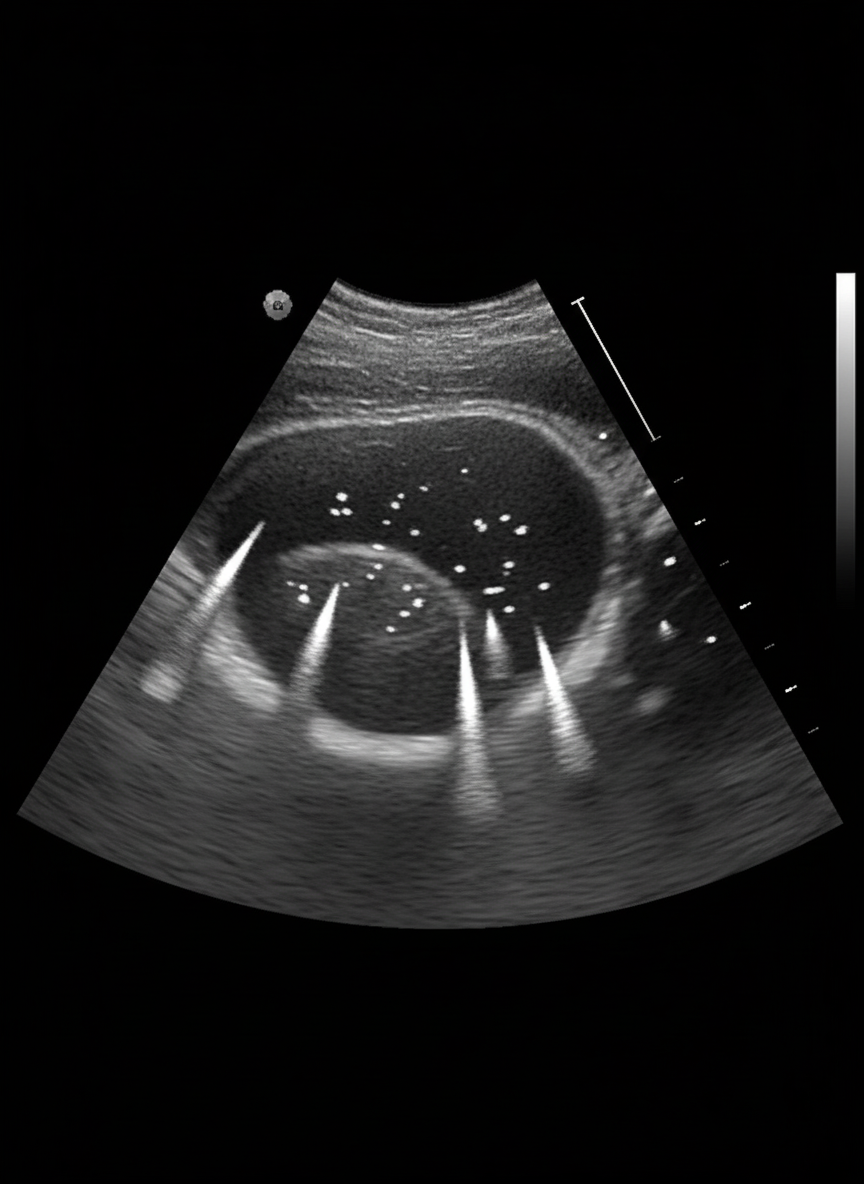
Which of the following parameters are used to estimate gestational age in the last trimester?
A 45-year-old male shows calcification on the right side of his abdomen in an AP view. In the lateral view, the calcification is seen to overlie the spine. What is the most likely diagnosis?
A 60-year-old male reports for denture adjustment. His OPG shows a 1 cm lytic area in the lower bicuspid region. What is the most probable diagnosis?
A 49-year-old computer technician receives irradiation to the pelvis for cervical cancer. Three months after irradiation, severe rectal proctitis may be shown by the presence of which of the following?
What condition is suggested by the below X-ray?
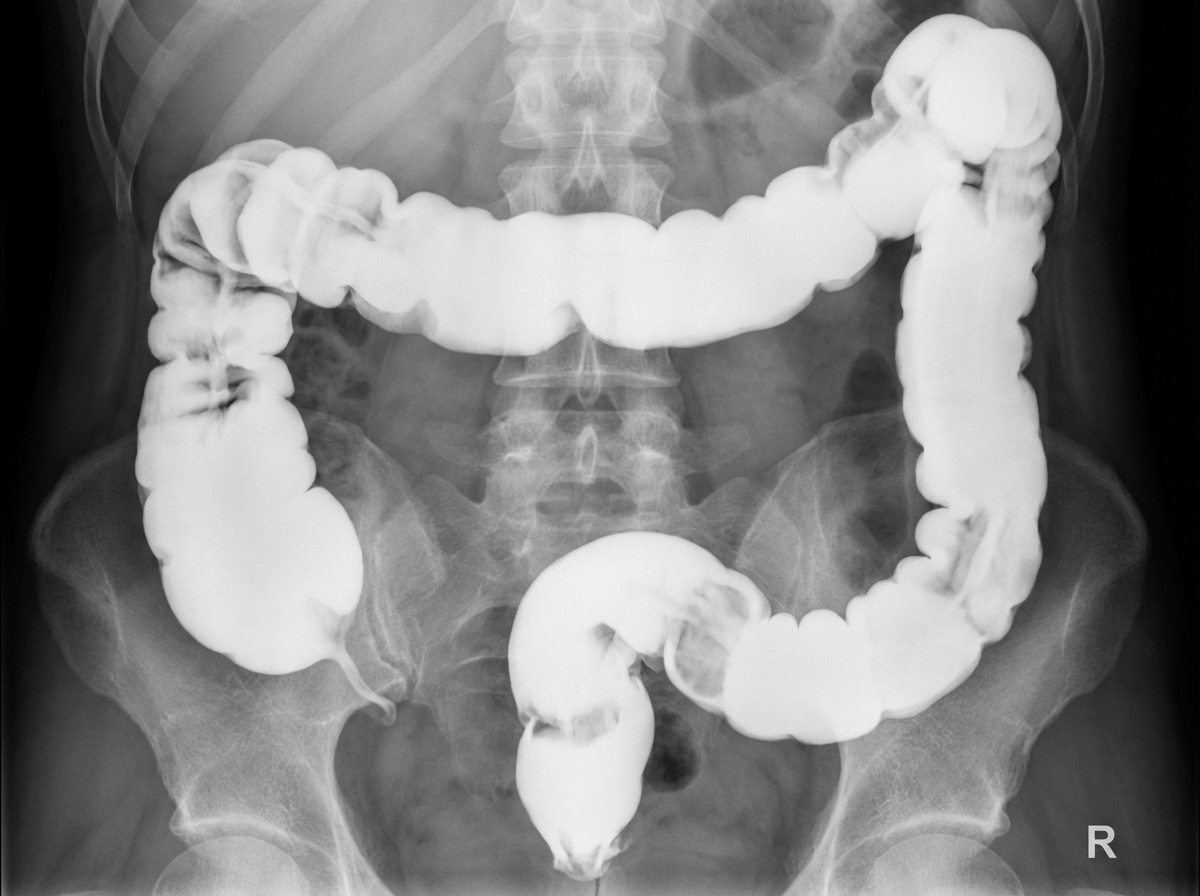
The 'bear paw' sign on imaging is characteristic of which condition?
Which of the following is hypointense (dark) on T2-weighted MRI?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
