Cardiovascular System — MCQs

On this page
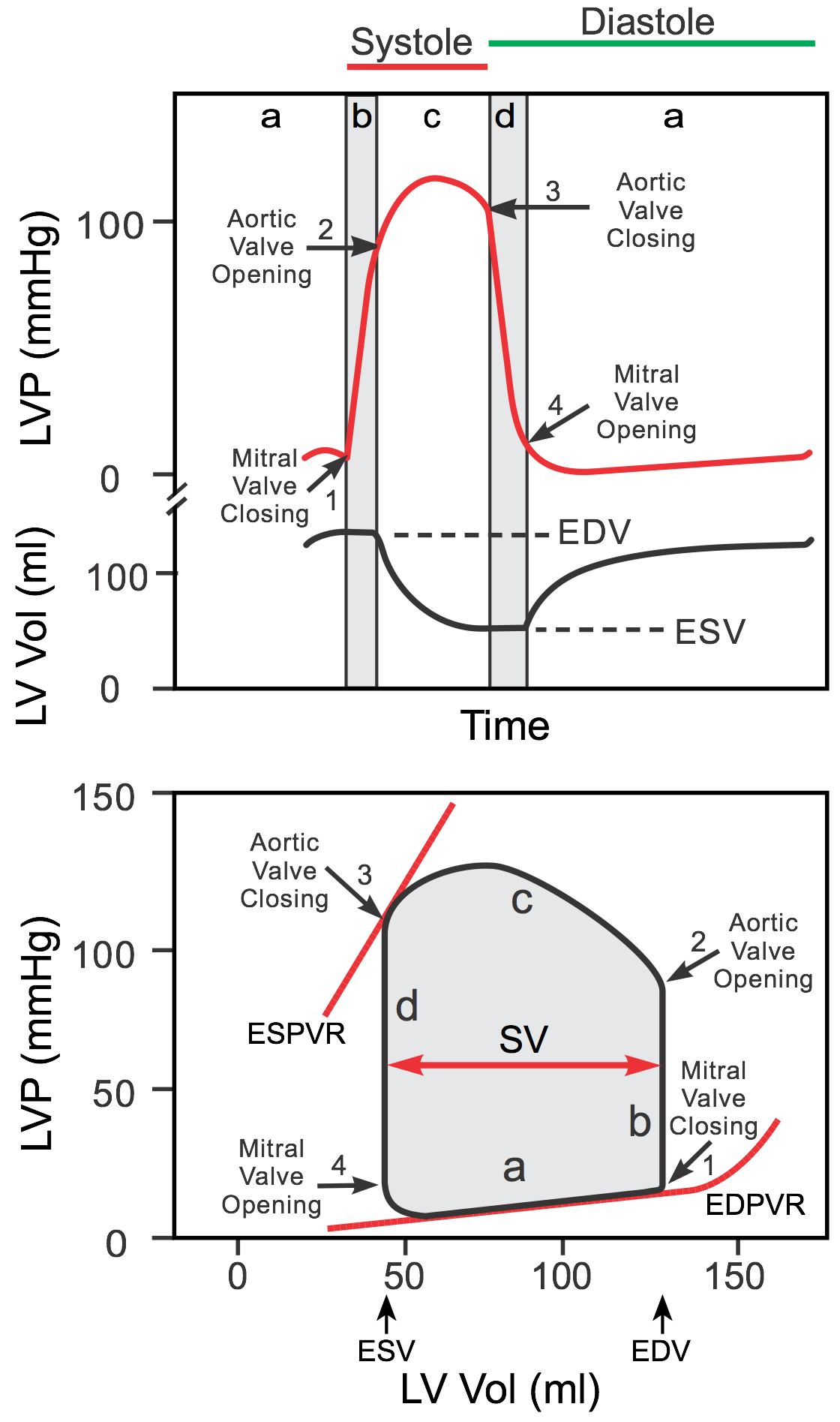
Pressure-Volume loop of cardiac cycle is shown below. What does point C represent?
The primary effect of vagal stimulation on the heart is
A shift of posture from supine to upright posture is associated with cardiovascular adjustments. Which of the following is NOT true in this context?
What is the mean arterial pressure (MAP) for a person with an arterial blood pressure of 125/75 mm Hg?
Which of the following equations correctly represents Poiseuille's Hagen law for fluid flow?
Coronary blood flow is maximum during which phase of the cardiac cycle?
Which heart sound is associated with decreased ventricular compliance?
Which is referred to as peripheral heart?
Which of the following is required for the Direct Fick method of measuring cardiac output?
The 'a' wave in jugular venous pressure is due to?
Practice by Chapter
Cardiac Electrophysiology
Practice Questions
Cardiac Cycle
Practice Questions
Cardiac Output and Its Regulation
Practice Questions
Hemodynamics and Blood Flow
Practice Questions
Arterial System Physiology
Practice Questions
Microcirculation and Lymphatics
Practice Questions
Venous Return and Central Venous Pressure
Practice Questions
Cardiovascular Reflexes
Practice Questions
Regional Circulations
Practice Questions
Cardiovascular Responses to Exercise and Stress
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
