Cardiovascular System — MCQs

On this page
Which of the following factors increases stroke volume?
Which of the following components are included in microcirculation?
Which of the following statements about volume receptors is NOT true?
What is the definition of preload in the context of cardiac physiology?
What does Einthoven's law state regarding the relationship between the electrical potentials of the limb leads?
Mechanism by which Ach decreases heart rate is by:
Mean arterial pressure is calculated as:
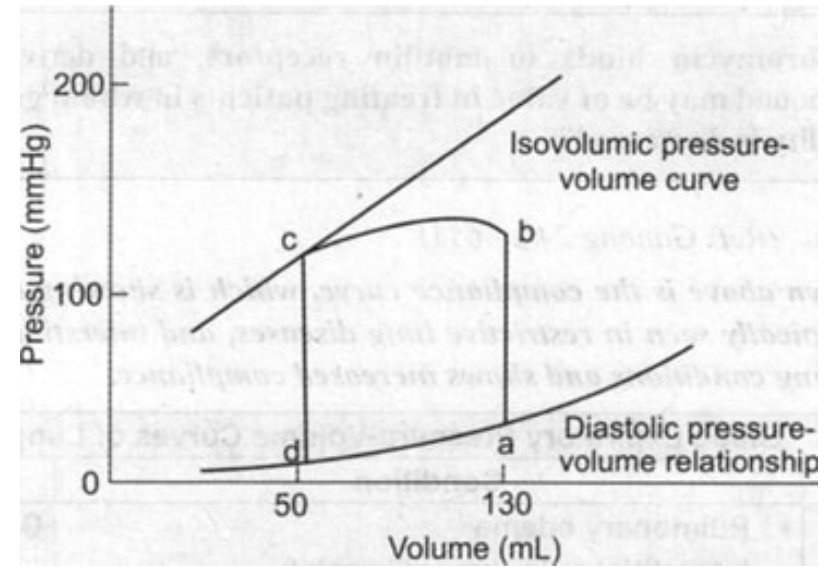
From the given pressure-volume curve, identify the end-diastolic volume (EDV) and end-systolic volume (ESV), then calculate the ejection fraction using the formula EF = (EDV - ESV)/EDV × 100%.
Volume receptors are primarily located in which of the following?
In which lead is the normal P wave inverted?
Practice by Chapter
Cardiac Electrophysiology
Practice Questions
Cardiac Cycle
Practice Questions
Cardiac Output and Its Regulation
Practice Questions
Hemodynamics and Blood Flow
Practice Questions
Arterial System Physiology
Practice Questions
Microcirculation and Lymphatics
Practice Questions
Venous Return and Central Venous Pressure
Practice Questions
Cardiovascular Reflexes
Practice Questions
Regional Circulations
Practice Questions
Cardiovascular Responses to Exercise and Stress
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
