Cardiovascular System — MCQs

On this page
The central venous pressure (CVP) is low in
In pregnancy, there is a physiological increase of the
Consider the following hemodynamic changes occurring during pregnancy: 1. Increase in cardiac output 2. Increase in stroke volume 3. Increase in colloid oncotic pressure 4. Increase in pulse rate Which of the statements given above are correct?
Regarding haemorrhagic shock, which one of the following statements is correct?
What is the function of the umbilical artery in fetal circulation?
Which among the following organs has the least arteriovenous oxygen difference?
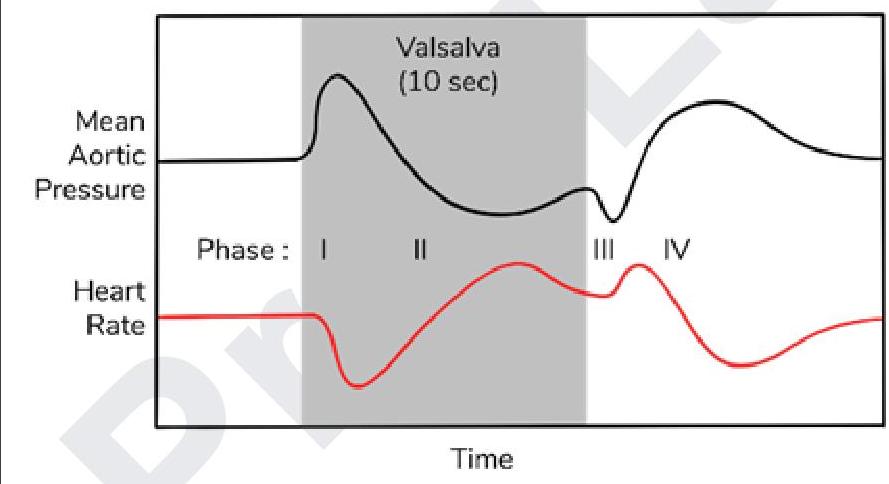
Blood pressure changes in radial artery were measured. Which of the following is the reason for initial rise in BP while performing Valsalva maneuver?
Windkessel effect is not shown by which of the following vessel?
If the contractility of the heart is decreased, which of the following is seen ?
Which factor most strongly influences coronary blood flow during exercise?
Practice by Chapter
Cardiac Electrophysiology
Practice Questions
Cardiac Cycle
Practice Questions
Cardiac Output and Its Regulation
Practice Questions
Hemodynamics and Blood Flow
Practice Questions
Arterial System Physiology
Practice Questions
Microcirculation and Lymphatics
Practice Questions
Venous Return and Central Venous Pressure
Practice Questions
Cardiovascular Reflexes
Practice Questions
Regional Circulations
Practice Questions
Cardiovascular Responses to Exercise and Stress
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
