Cardiovascular System — MCQs

On this page
The recording of cardiac cycle is drawn below. Which of the following is correct about $X$ and $Y$ shown in the image?
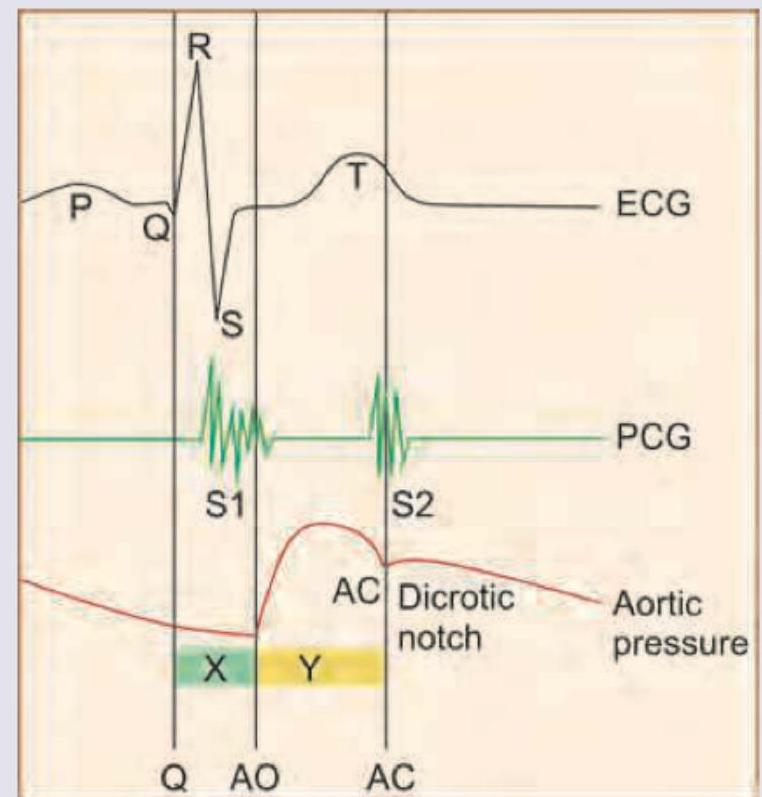
The following diagram represents flow in compliant versus non-compliant aorta. This shows operation of:
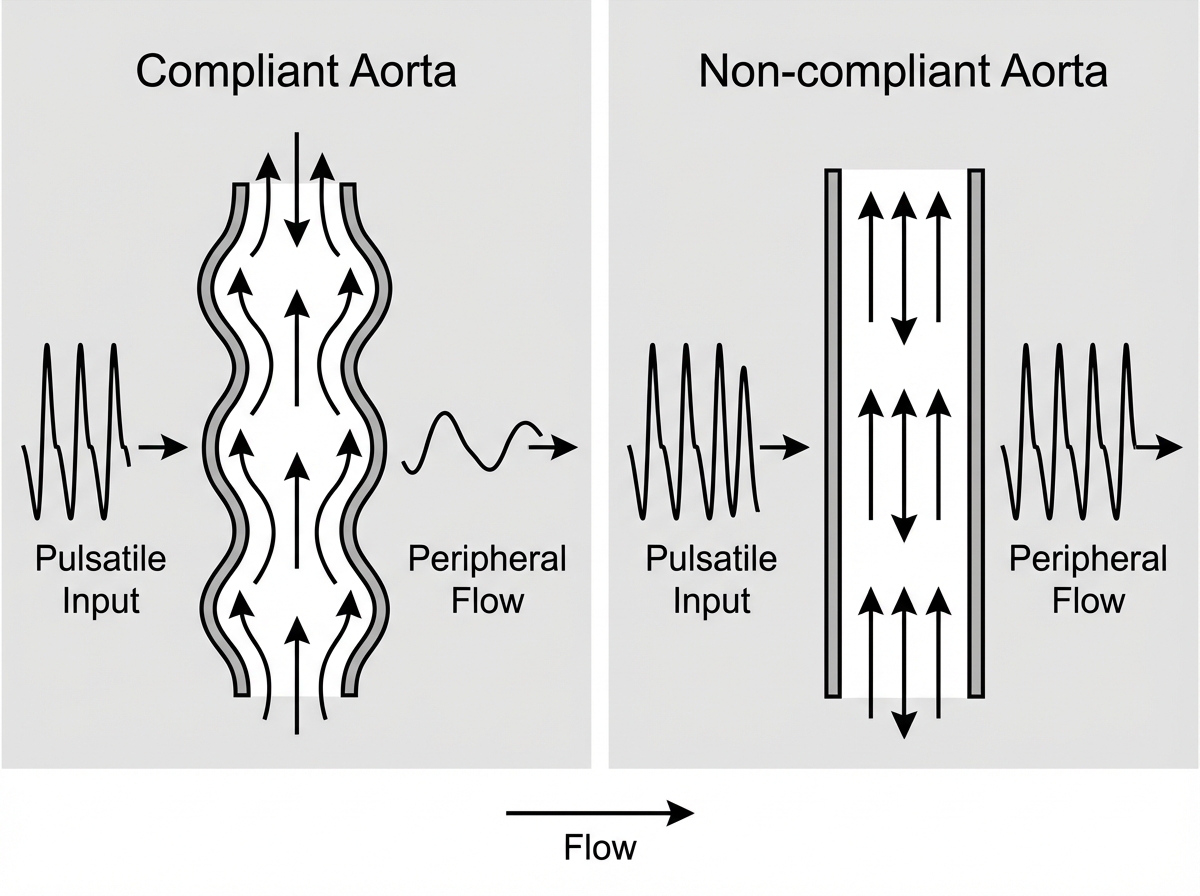
Which of the following dissociation curve mentioned is for myoglobin?
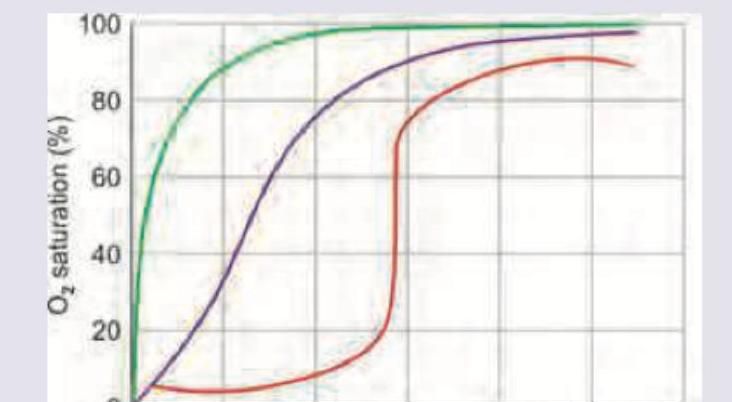
The pressure-volume loop of left ventricle tracing of the patient indicates:
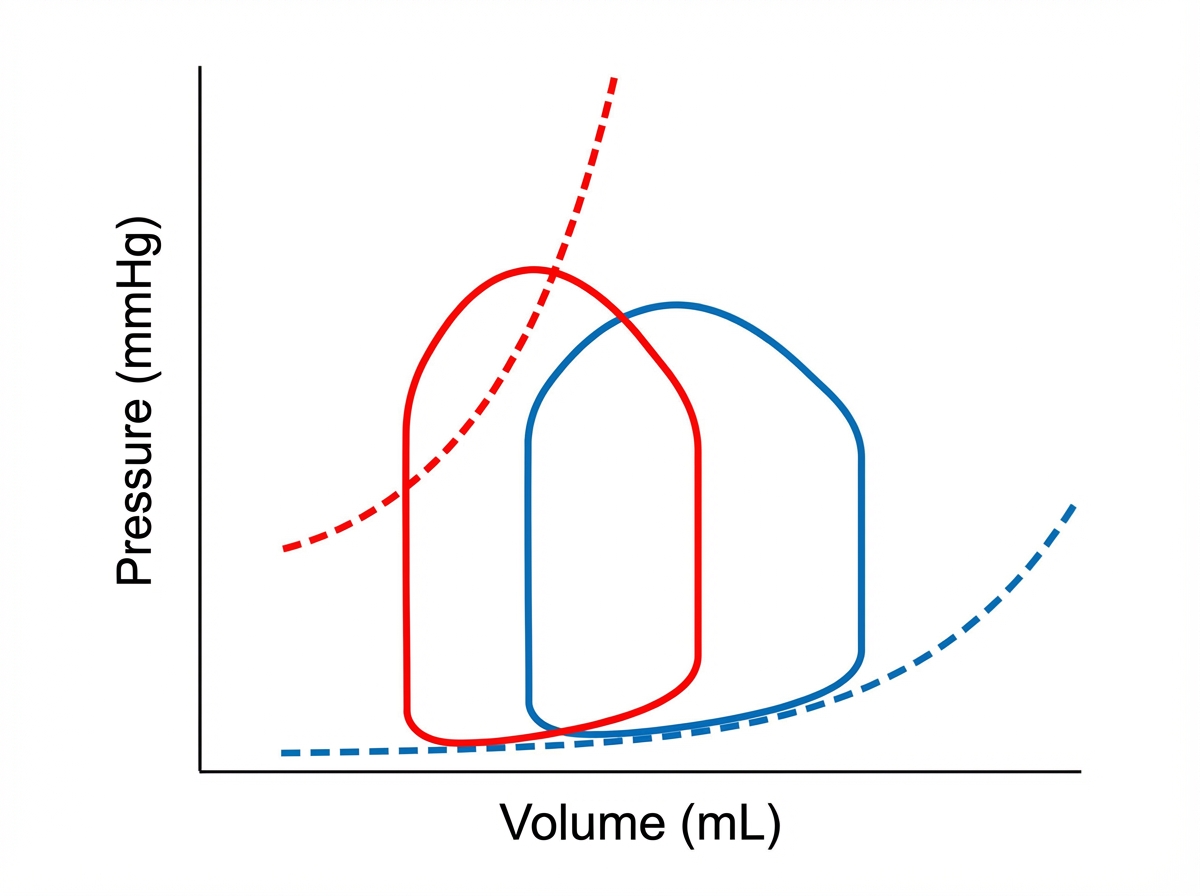
Which of the following is correct about the point marked $Z$ on the cardiac cycle?
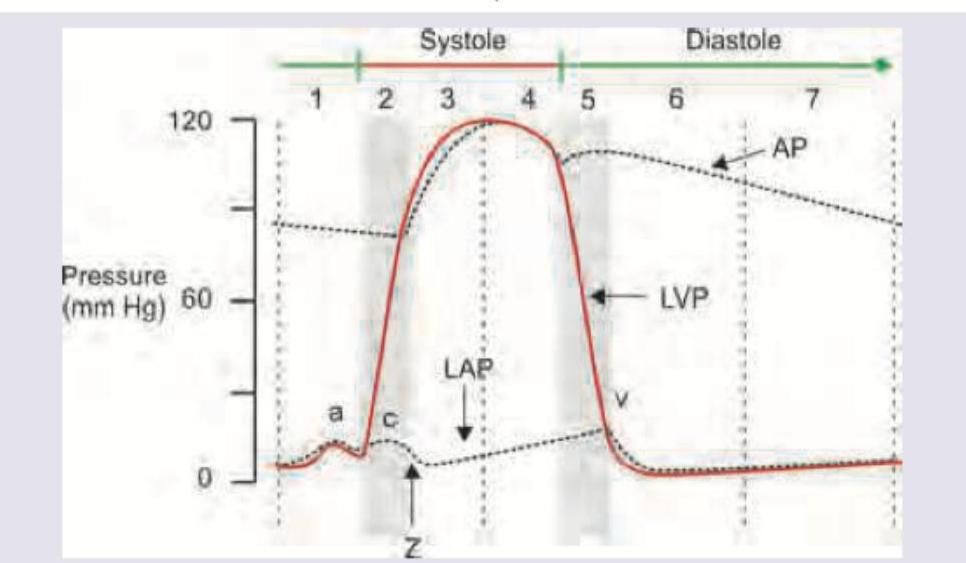
Which of the following is correct about the 'X' marking in Arterial Waveform?
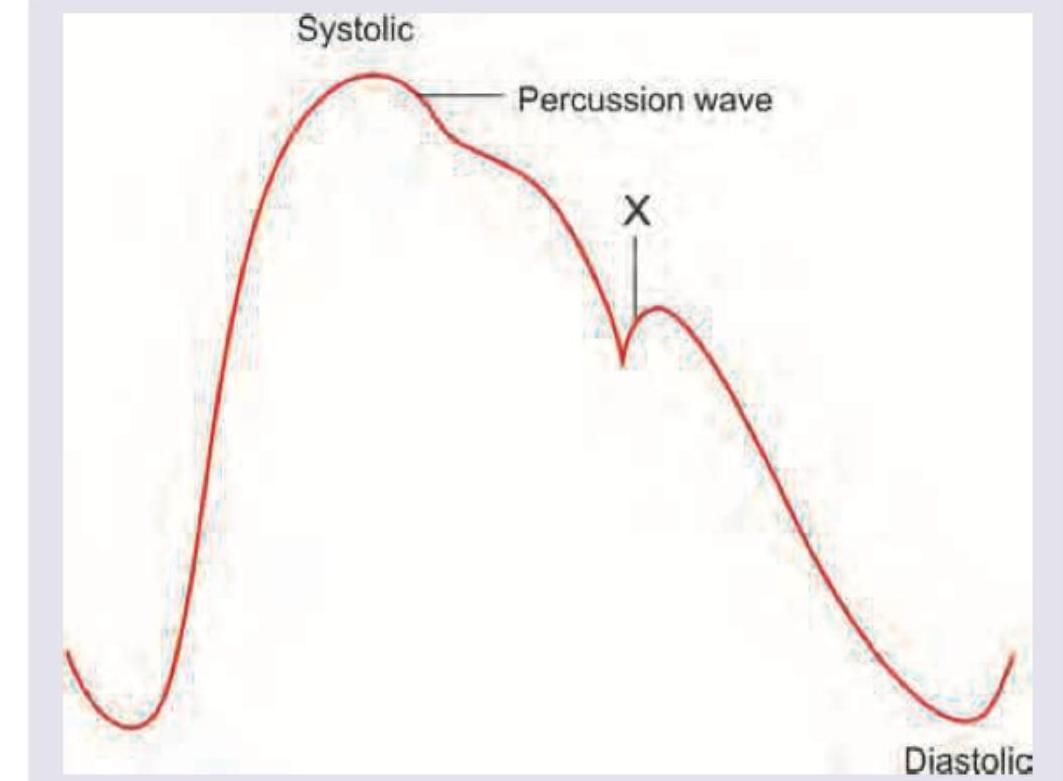
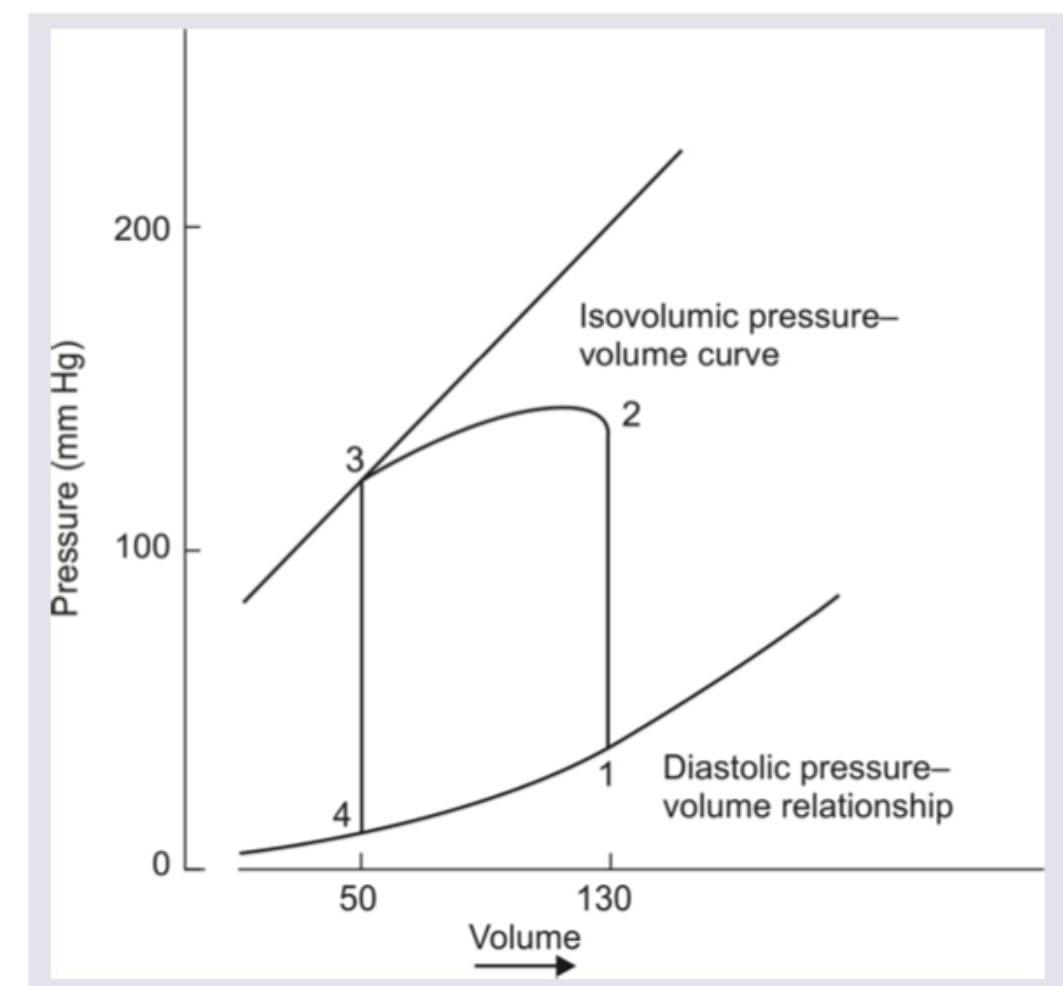
Which of the following is correct about the pressure volume loop of left ventricle?
The A wave in His bundle electrogram shows presence of:
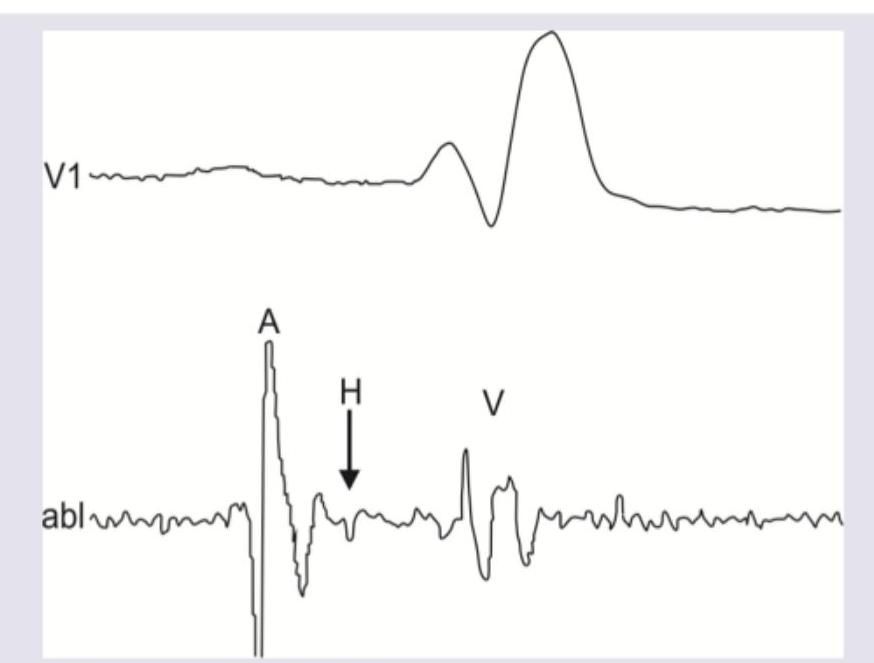
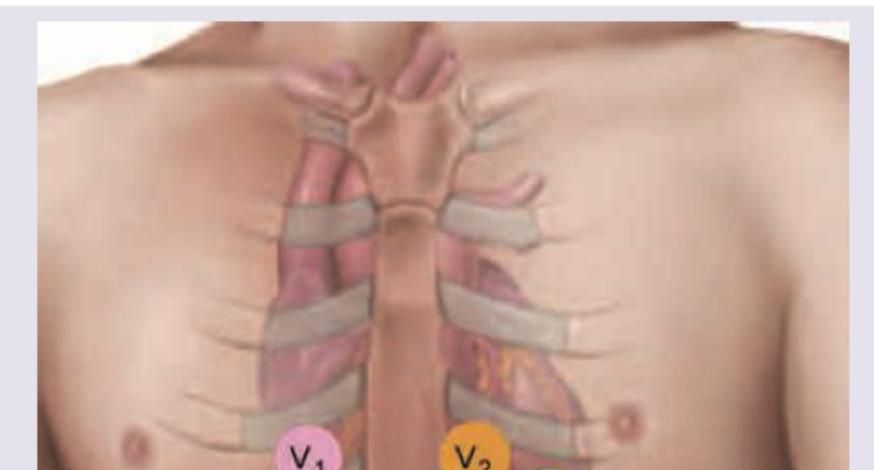
The lead of ECG marked as $X$ is called:
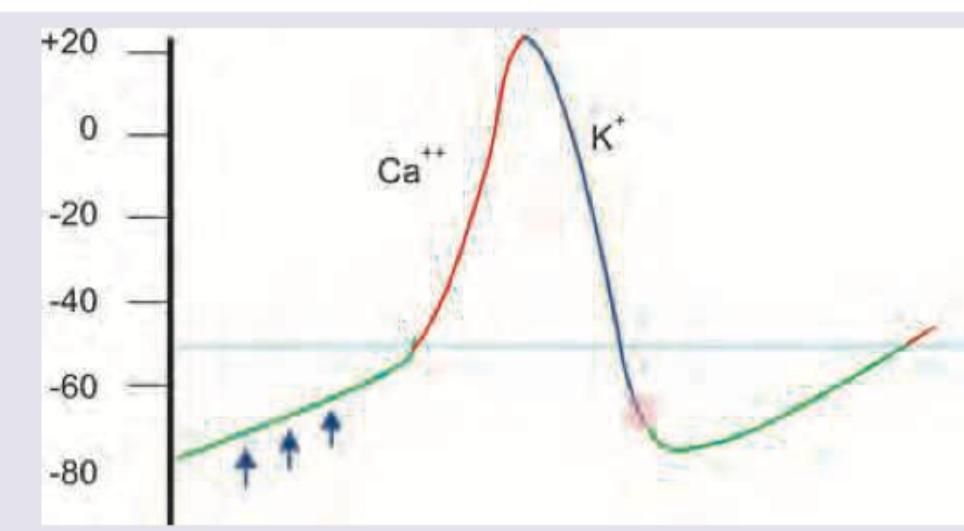
The phase of cardiac action potential marked Green is related to which of the following?
Practice by Chapter
Cardiac Electrophysiology
Practice Questions
Cardiac Cycle
Practice Questions
Cardiac Output and Its Regulation
Practice Questions
Hemodynamics and Blood Flow
Practice Questions
Arterial System Physiology
Practice Questions
Microcirculation and Lymphatics
Practice Questions
Venous Return and Central Venous Pressure
Practice Questions
Cardiovascular Reflexes
Practice Questions
Regional Circulations
Practice Questions
Cardiovascular Responses to Exercise and Stress
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
