Cardiovascular System — MCQs

On this page
Which substance contracts mesangial cells?
Which cells secrete IL-1?
What physiological event occurs during isovolumetric contraction?
Heme is converted to bilirubin mainly in which location?
The 'a' wave is absent in which of the following conditions?
Orthopnea in heart failure develops due to which of the following?
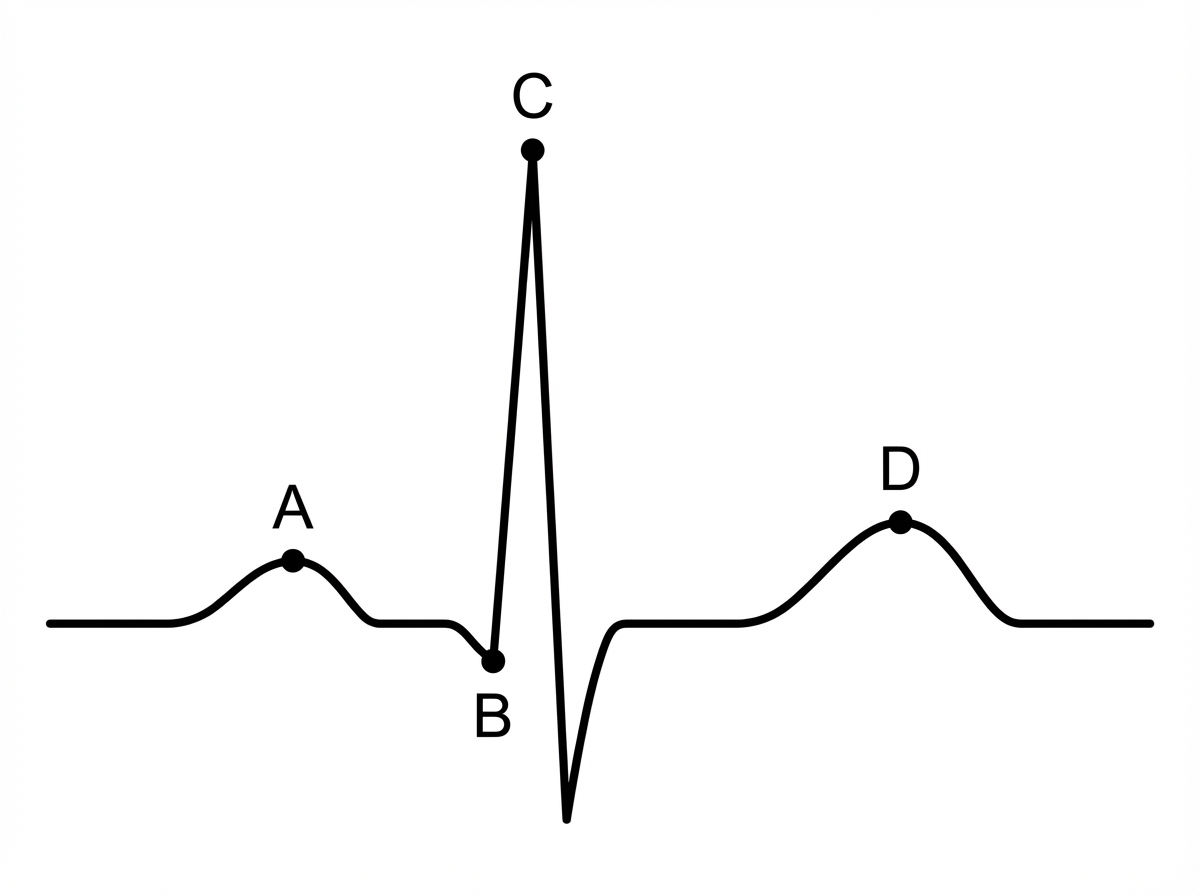
In the diagram below, which labeled point represents the "R" wave of ventricular depolarization?
Regarding S3 heart sound, all are true except?
What is the characteristic ECG change observed in hyperkalemia?
Which of the following statements regarding the flow of lymph from the lower limb is true?
Practice by Chapter
Cardiac Electrophysiology
Practice Questions
Cardiac Cycle
Practice Questions
Cardiac Output and Its Regulation
Practice Questions
Hemodynamics and Blood Flow
Practice Questions
Arterial System Physiology
Practice Questions
Microcirculation and Lymphatics
Practice Questions
Venous Return and Central Venous Pressure
Practice Questions
Cardiovascular Reflexes
Practice Questions
Regional Circulations
Practice Questions
Cardiovascular Responses to Exercise and Stress
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
