Cardiovascular System — MCQs

On this page
CSF pressure is mainly regulated by?
Pre-capillary sphincter relaxation is caused by what?
Triggered automaticity leads to the development of which of the following rhythm disorders?
An ECG obtained from a 57-year-old male during a routine physical examination reveals atrial fibrillation. Which is most likely to accompany this condition?
Oxygen consumption by the heart is determined primarily by which of the following?
Which one of the following is not a transport or binding protein?
Coronary vasodilation is caused by:
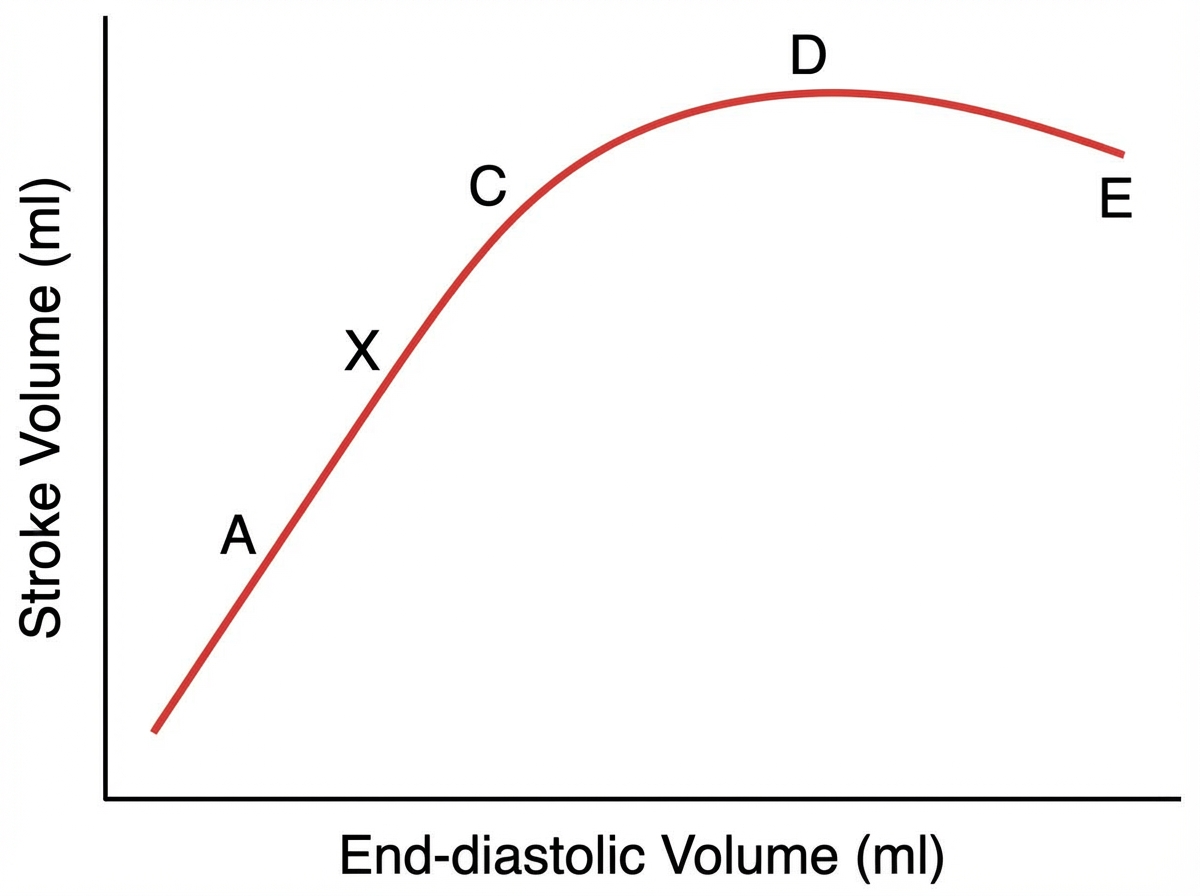
A mild hemorrhage will cause stroke volume to shift from point X to which of the following points?
Which of the following phases correlates with isovolumic contraction?
What is the second messenger involved in vagal bradycardia?
Practice by Chapter
Cardiac Electrophysiology
Practice Questions
Cardiac Cycle
Practice Questions
Cardiac Output and Its Regulation
Practice Questions
Hemodynamics and Blood Flow
Practice Questions
Arterial System Physiology
Practice Questions
Microcirculation and Lymphatics
Practice Questions
Venous Return and Central Venous Pressure
Practice Questions
Cardiovascular Reflexes
Practice Questions
Regional Circulations
Practice Questions
Cardiovascular Responses to Exercise and Stress
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
