Cardiovascular System — MCQs

On this page
In which stage of red blood cell development does hemoglobin first appear?
Which of the following is seen in second-degree AV block?
Which of the following phases is absent in the action potential of pacemaker cells?
Triggered effect in myocardium is due to what?
Which peptide causes increased capillary permeability and edema?
A patient's ECG shows Lead III with no S wave, but normal P, R, and T waves. What conclusions can be drawn about the patient's cardiac status?
What period does ventricular contraction correspond to on an ECG?
Cardiac output in L/min divided by heart rate equals:
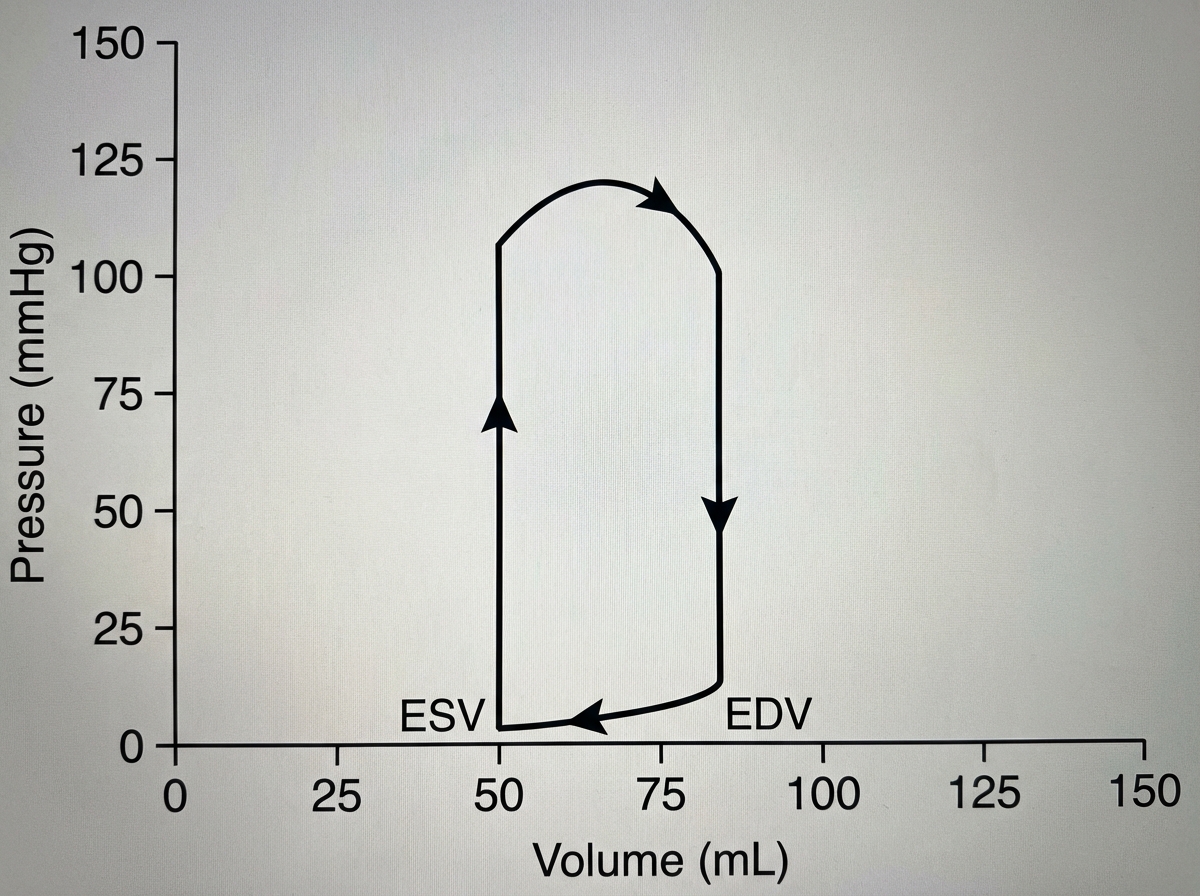
A 40-year-old man presents with a resting heart rate of 180 beats/min. A pressure-volume diagram of the left ventricle is shown below. What is the cardiac output?
Phase 1 of the myocardial action potential is primarily due to which ion movement?
Practice by Chapter
Cardiac Electrophysiology
Practice Questions
Cardiac Cycle
Practice Questions
Cardiac Output and Its Regulation
Practice Questions
Hemodynamics and Blood Flow
Practice Questions
Arterial System Physiology
Practice Questions
Microcirculation and Lymphatics
Practice Questions
Venous Return and Central Venous Pressure
Practice Questions
Cardiovascular Reflexes
Practice Questions
Regional Circulations
Practice Questions
Cardiovascular Responses to Exercise and Stress
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
