Cardiovascular System — MCQs

On this page
What is the blood flow of resting skeletal muscle?
Which component of systemic arterial blood pressure undergoes the least fluctuation?
Which of the following causes a decrease in blood pressure?
What percentage of the total blood volume is typically found in the capillaries?
Synthesis of clotting factors requires which vitamin?
In which electrolyte abnormality, the following ECG finding is seen?
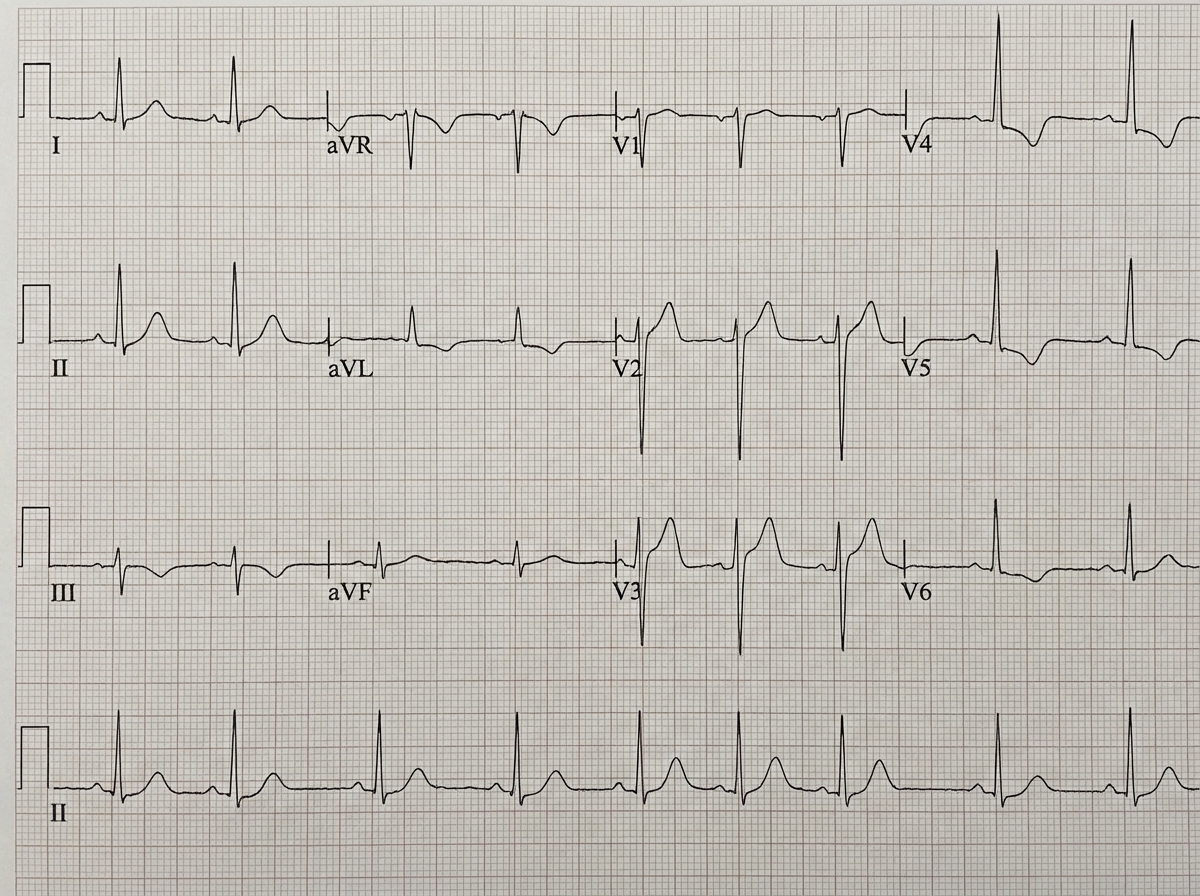
In the coagulation pathway, which factor is known as the Fibrin Stabilizing Factor?
What is the duration of the second heart sound?
Lymph flow from the foot is:
Which of the following is not increased during isometric exercise?
Practice by Chapter
Cardiac Electrophysiology
Practice Questions
Cardiac Cycle
Practice Questions
Cardiac Output and Its Regulation
Practice Questions
Hemodynamics and Blood Flow
Practice Questions
Arterial System Physiology
Practice Questions
Microcirculation and Lymphatics
Practice Questions
Venous Return and Central Venous Pressure
Practice Questions
Cardiovascular Reflexes
Practice Questions
Regional Circulations
Practice Questions
Cardiovascular Responses to Exercise and Stress
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
