Cardiovascular System — MCQs

On this page
Which of the following best describes the effect of calcium ions on the myocardium?
Which of the following is not true of the 'a' wave of venous pulsations in the neck?
What is the primary function of hemoglobin regarding oxygen transport?
Conversion of prothrombin to thrombin requires which of the following?
What is the maximum pressure observed in the left ventricle?
The absolute refractory period of the heart is the period of time in which:
If the heart rate is 70 beats/min, then the cardiac output of this ventricle is closest to?
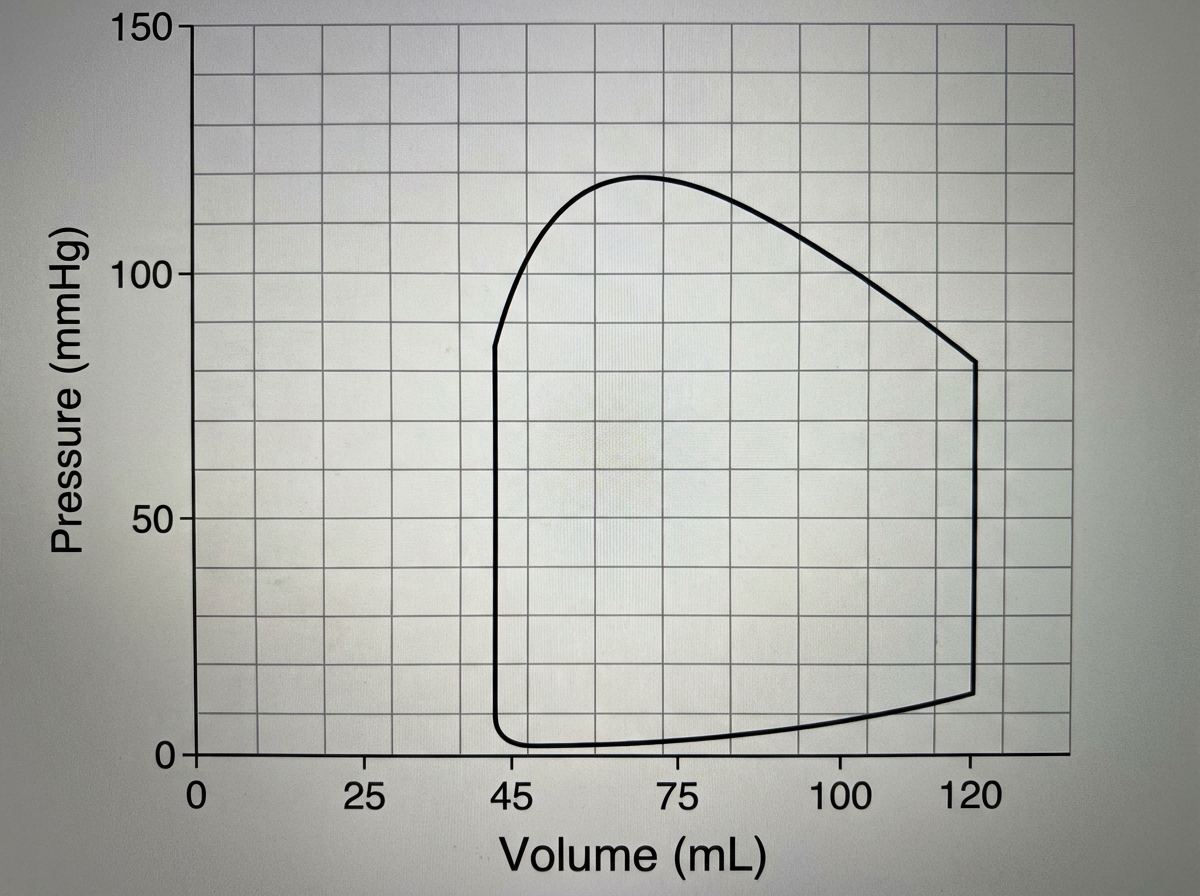
Which of the following statements regarding blood flow in various organs is true?
If a person has a heart rate of 70 beats/min, a left ventricular end-diastolic volume of 100 ml, and an ejection fraction of 0.50, what is the cardiac output?
Sympathetic stimulation causes all of the following, except?
Practice by Chapter
Cardiac Electrophysiology
Practice Questions
Cardiac Cycle
Practice Questions
Cardiac Output and Its Regulation
Practice Questions
Hemodynamics and Blood Flow
Practice Questions
Arterial System Physiology
Practice Questions
Microcirculation and Lymphatics
Practice Questions
Venous Return and Central Venous Pressure
Practice Questions
Cardiovascular Reflexes
Practice Questions
Regional Circulations
Practice Questions
Cardiovascular Responses to Exercise and Stress
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
