Cardiovascular System — MCQs

On this page
What causes the third heart sound (S3)?
During inhibition of the SA node by vagal stimulation, which of the following occurs?
What is the normal cerebral blood flow per 100 grams of brain tissue per minute?
When does the pre-ejection ventricular phase begin?
All of the following statements regarding arteries are true EXCEPT?
Cardiac output is measured by all methods EXCEPT?
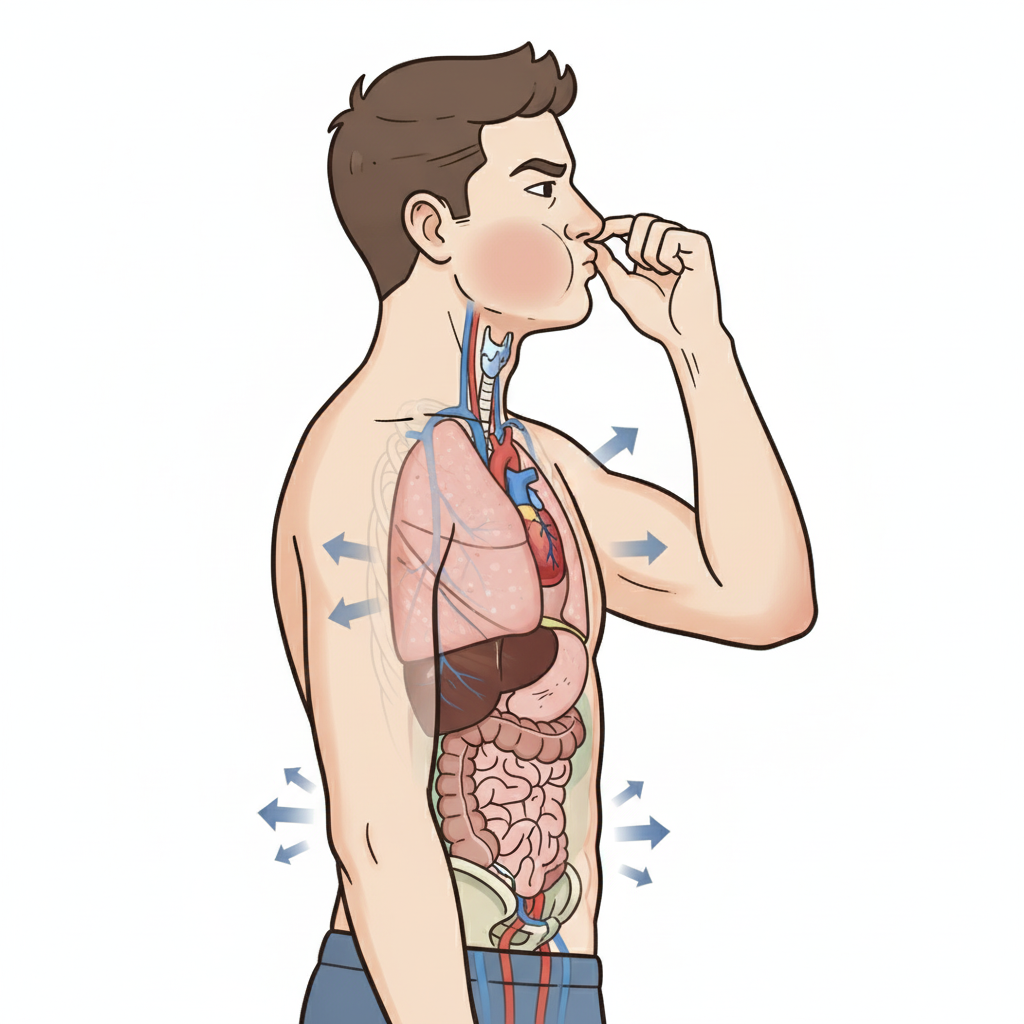
All of the following are physiological effects of the manoeuvre shown below except?
What is the normal cardiac index in an adult?
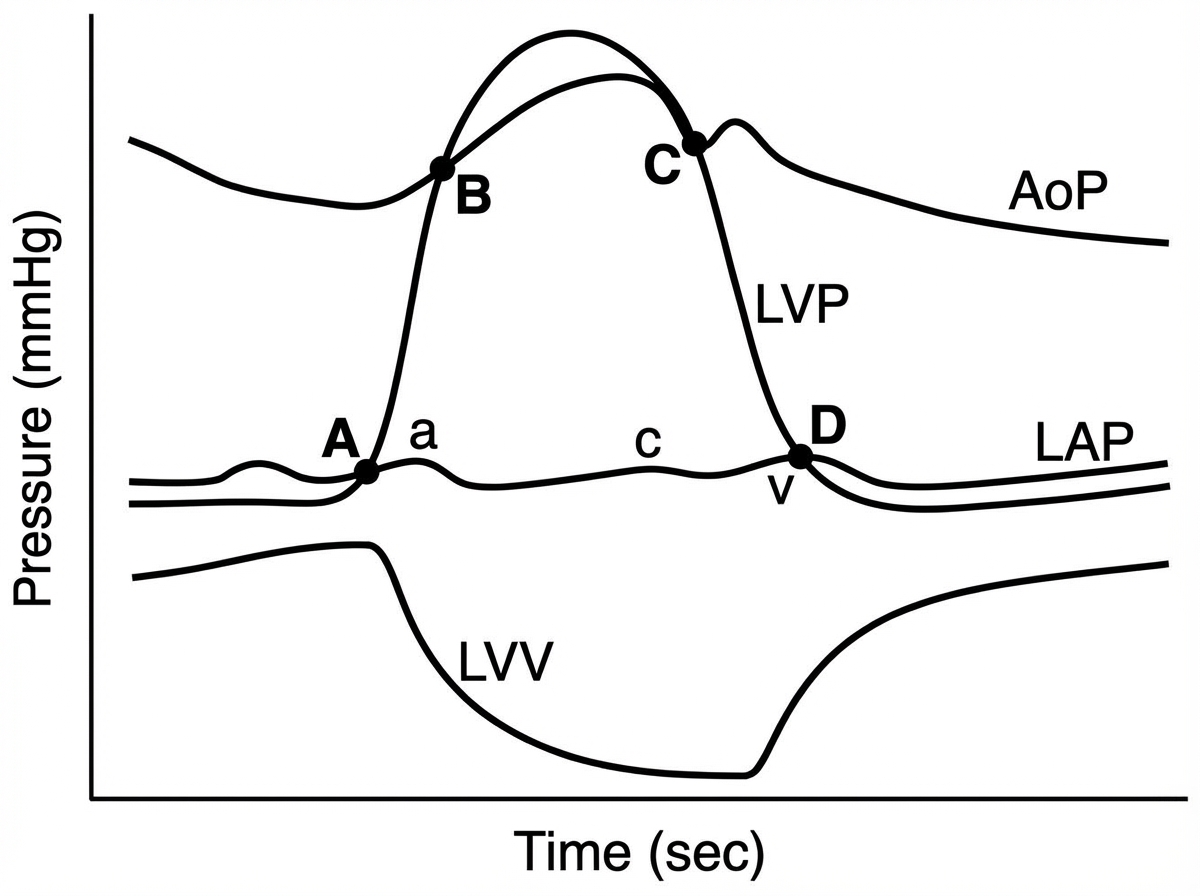
Closing of the mitral valve begins at which point?
What is true about troponin?
Practice by Chapter
Cardiac Electrophysiology
Practice Questions
Cardiac Cycle
Practice Questions
Cardiac Output and Its Regulation
Practice Questions
Hemodynamics and Blood Flow
Practice Questions
Arterial System Physiology
Practice Questions
Microcirculation and Lymphatics
Practice Questions
Venous Return and Central Venous Pressure
Practice Questions
Cardiovascular Reflexes
Practice Questions
Regional Circulations
Practice Questions
Cardiovascular Responses to Exercise and Stress
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
