Autonomic Nervous System Drugs — MCQs

On this page
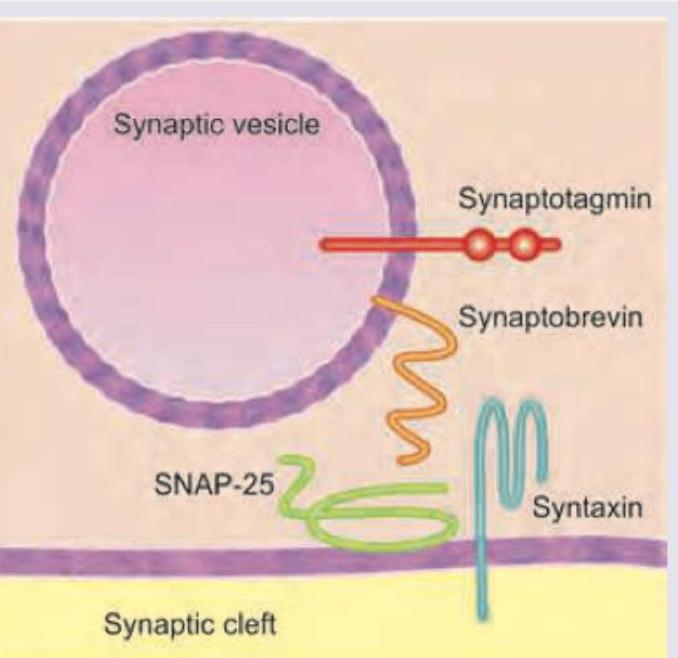
Which of the following is the site of action of botulinum toxin? (Recent NEET Pattern 2016-17)
A 20-year-old woman is admitted with the following presentation. 1% pilocarpine is not showing any response on the side of mydriasis. What is the diagnosis? (Recent NEET Pattern 2016-17)
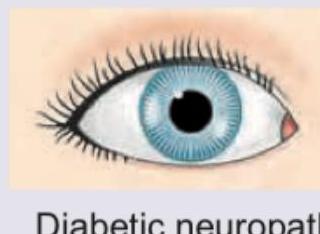
A 35-year-old farmer consumed a pesticide due to inability to repay loans. On examination he is having increased sweating, salivation and muscle fasciculations. The family members have also brought the empty canister of insecticide. All are correct about the condition except: (Recent NEET Pattem 2016-17)
Which of the following statement is correct regarding the graph shown? (AllMS Nov 2016)
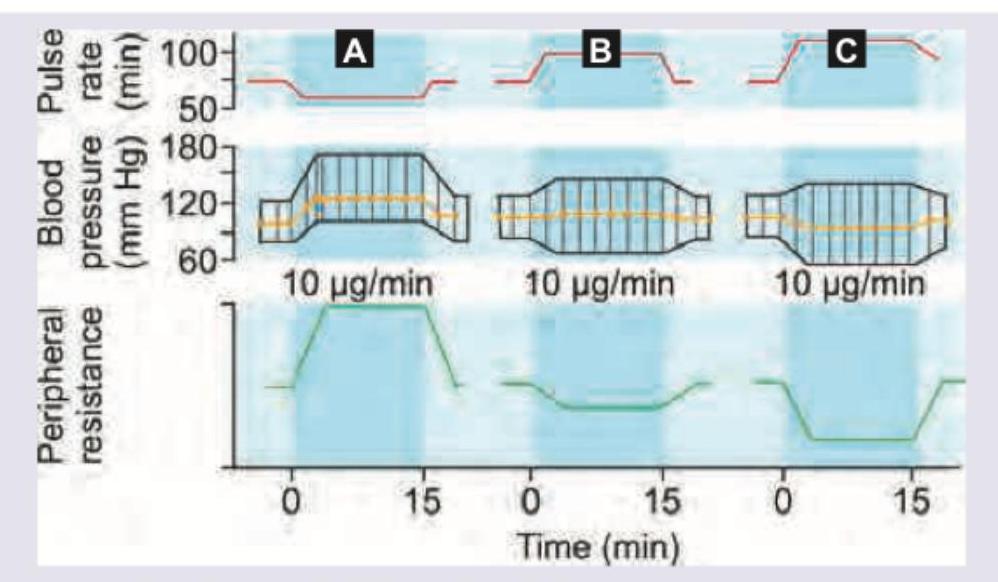
A man was brought to the emergency room after poisoning with an unknown substance. Muscarinic poisoning was suspected and he was treated for the same. What is the possible presenting feature which led to the diagnosis?
Match the following: Column A: a. Beta 1 b. Beta 2 c. Beta 3 Column B: 1. Mirabegron 2. Betaxolol 3. Salbutamol
A kid went to a temple with his grandmother and was constantly crying. On examination he had excruciating pain, hypertension, increased heart rate, sweating profusely, priapism and cold clammy skin. What should be the treatment given to the patient?
An investigator is developing a new intravenous medication that acts as a selective agonist at β-2 receptors. In addition to causing bronchodilation, this drug is most likely to have which of the following effects?
A 61-year-old woman comes to the emergency department because of a 2-hour history of headache, nausea, blurred vision, and pain in the left eye. She has had similar symptoms in the past. Her vital signs are within normal limits. The left eye is red and is hard on palpation. The left pupil is mid-dilated and nonreactive to light. Administration of which of the following drugs should be avoided in this patient?
Ritodrine is a:-
Practice by Chapter
Cholinergic Agonists
Practice Questions
Cholinergic Antagonists
Practice Questions
Adrenergic Agonists
Practice Questions
Adrenergic Antagonists
Practice Questions
Ganglionic Agents
Practice Questions
Neuromuscular Blocking Agents
Practice Questions
Autonomic Drugs in Ophthalmology
Practice Questions
Autonomic Drugs in Cardiovascular Disease
Practice Questions
Autonomic Drugs in Respiratory Disease
Practice Questions
Autonomic Drugs in Urological Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
