Autonomic Nervous System Drugs — MCQs

On this page
Which of the following properties makes pyridostigmine different from neostigmine?
Which of the following H1 blockers has high anticholinergic activity?
Which of the following drugs should be given in a patient with acute angle closure glaucoma, except?
In oral poisoning with carbamate insecticide, which of the following may be hazardous?
Which of the following can be blocked by atropine, a muscarinic receptor blocker?
Which of the following is an example of asymmetric mixed-onium chlorofumarate?
Beta 2 selective agonists are often effective in which of the following conditions?
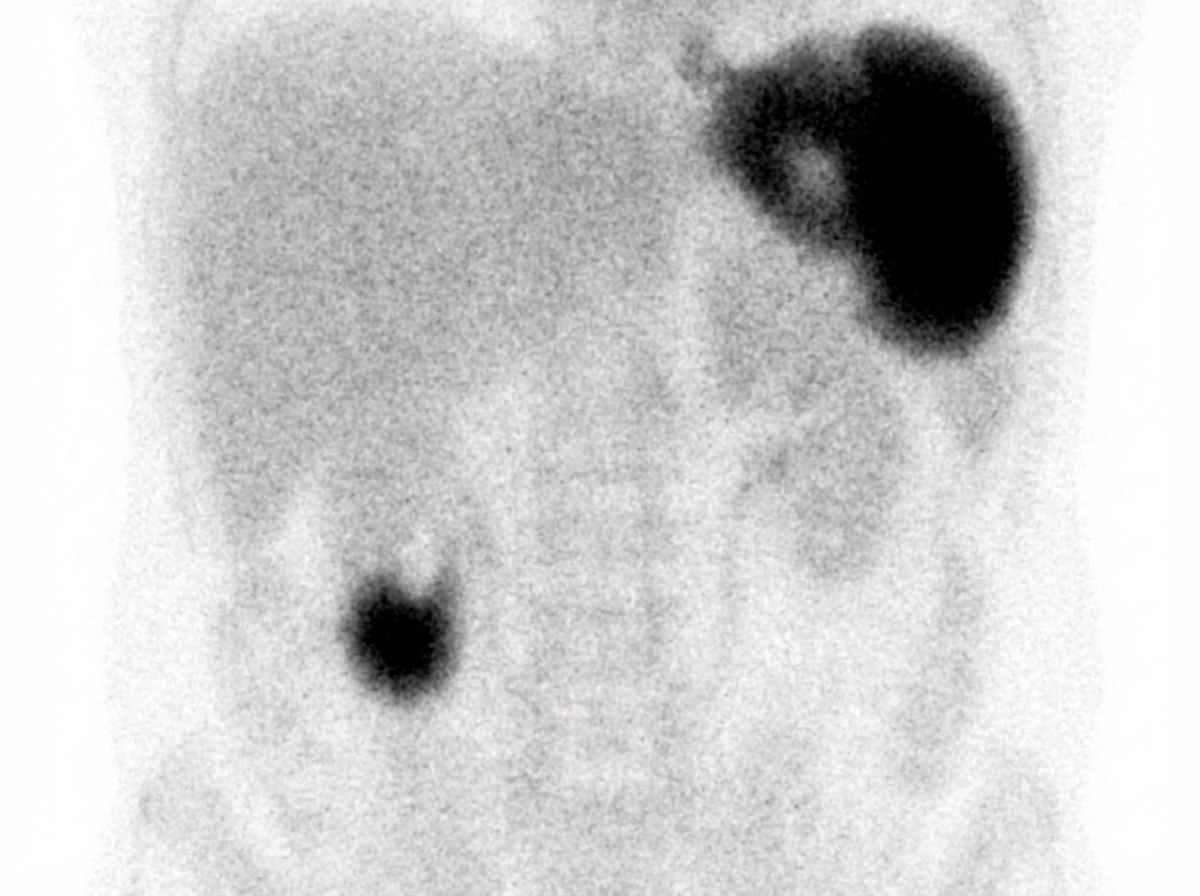
Which of the following drugs is used in this test?
What is the most important action of beta-blockers in glaucoma?
Which of the following inhibits the rate-limiting step of norepinephrine synthesis?
Practice by Chapter
Cholinergic Agonists
Practice Questions
Cholinergic Antagonists
Practice Questions
Adrenergic Agonists
Practice Questions
Adrenergic Antagonists
Practice Questions
Ganglionic Agents
Practice Questions
Neuromuscular Blocking Agents
Practice Questions
Autonomic Drugs in Ophthalmology
Practice Questions
Autonomic Drugs in Cardiovascular Disease
Practice Questions
Autonomic Drugs in Respiratory Disease
Practice Questions
Autonomic Drugs in Urological Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
