Autonomic Nervous System Drugs — MCQs

On this page
The schematic diagram is depicting some features of the autonomic and somatic nervous systems. What is the neurotransmitter at site 'F'?
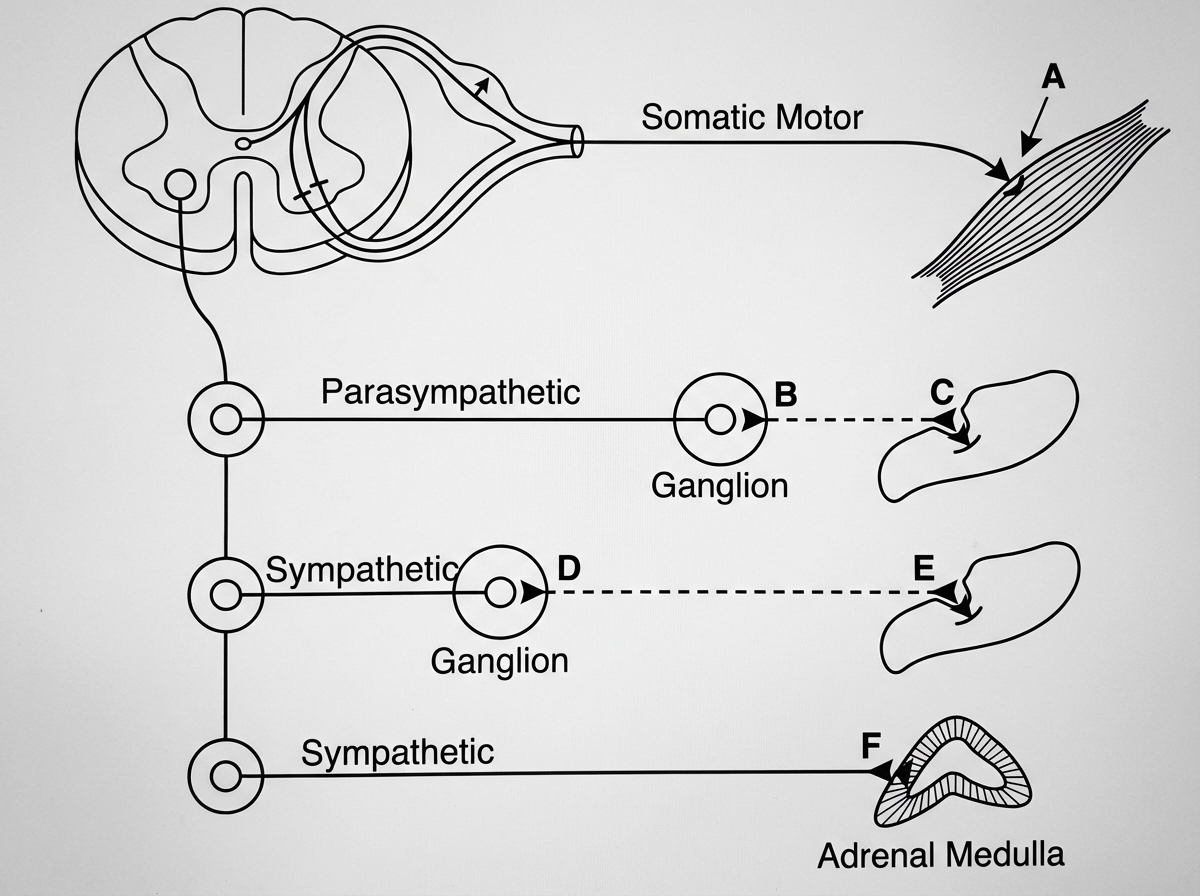
Prolonged muscle paralysis in a healthy individual may be caused by:
Curare poisoning is characterised by:
Which is the most dangerous effect of belladonna in very young children?
Which of the following is NOT a use of anticholinergics?
What is the primary reason dopamine is preferred in the treatment of shock?
Which muscle is injected with botulinum toxin?
Propranolol is useful in all the following conditions EXCEPT:
Which alpha-2 agonist is used in the management of glaucoma?
Nicotinic receptors are seen in all except?
Practice by Chapter
Cholinergic Agonists
Practice Questions
Cholinergic Antagonists
Practice Questions
Adrenergic Agonists
Practice Questions
Adrenergic Antagonists
Practice Questions
Ganglionic Agents
Practice Questions
Neuromuscular Blocking Agents
Practice Questions
Autonomic Drugs in Ophthalmology
Practice Questions
Autonomic Drugs in Cardiovascular Disease
Practice Questions
Autonomic Drugs in Respiratory Disease
Practice Questions
Autonomic Drugs in Urological Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
