Autonomic Nervous System Drugs — MCQs

On this page
Which of the following is contraindicated in a patient with Myasthenia Gravis?
The Edrophonium test is helpful in diagnosing which of the following conditions?
Hyoscine is which of the following?
Which was the first neuromuscular blocker to be used clinically?
Which of the following is a peripherally acting muscle relaxant?
A specific compound is derived from a plant. What condition is this compound used to treat?
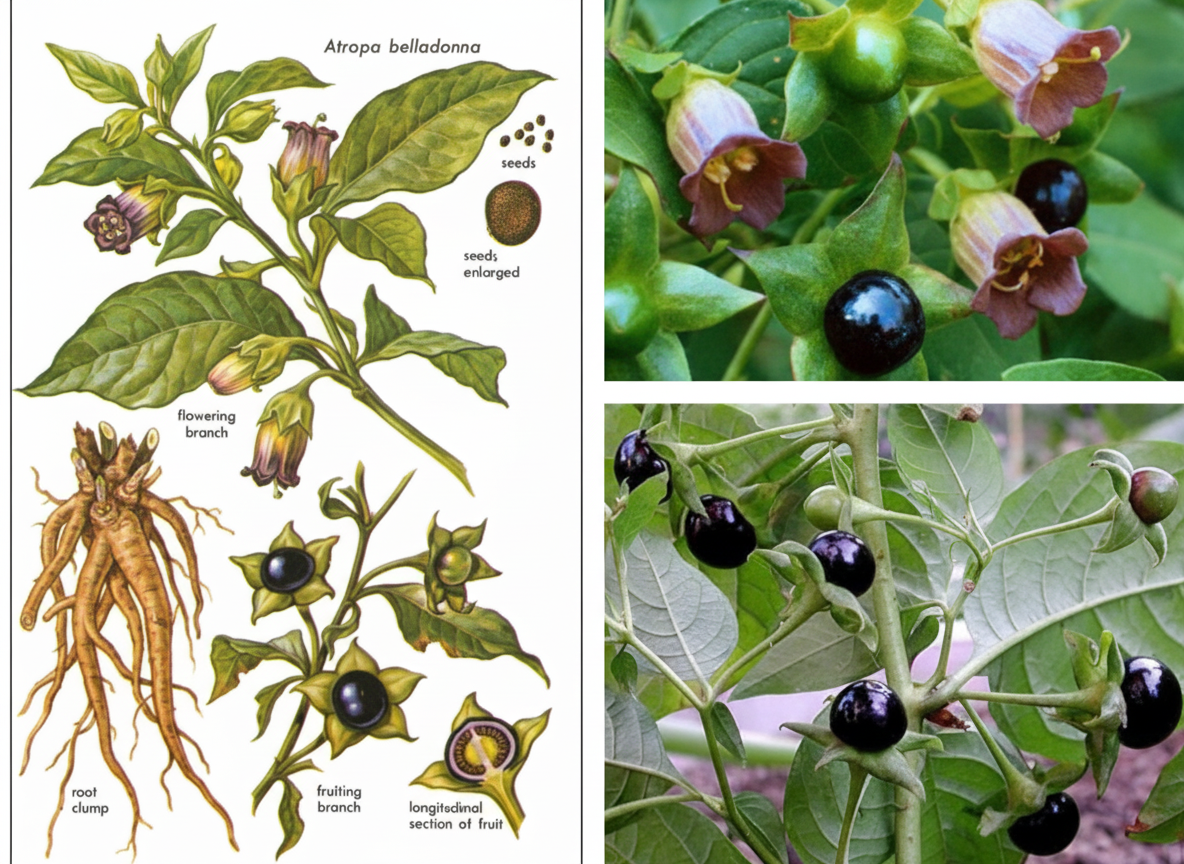
Which of the following functions is NOT associated with anticholinergic drugs?
In which of the following conditions, anti-muscarinic drugs are to be avoided?
A 60-year-old male requires an eye examination. Which drug can be used to dilate his pupils without causing paralysis of the ciliary muscles?
Which of the following conditions is NOT treated with a cholinomimetic agent?
Practice by Chapter
Cholinergic Agonists
Practice Questions
Cholinergic Antagonists
Practice Questions
Adrenergic Agonists
Practice Questions
Adrenergic Antagonists
Practice Questions
Ganglionic Agents
Practice Questions
Neuromuscular Blocking Agents
Practice Questions
Autonomic Drugs in Ophthalmology
Practice Questions
Autonomic Drugs in Cardiovascular Disease
Practice Questions
Autonomic Drugs in Respiratory Disease
Practice Questions
Autonomic Drugs in Urological Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
