Autonomic Nervous System Drugs — MCQs

On this page
Drug S is most like which of the following drugs?
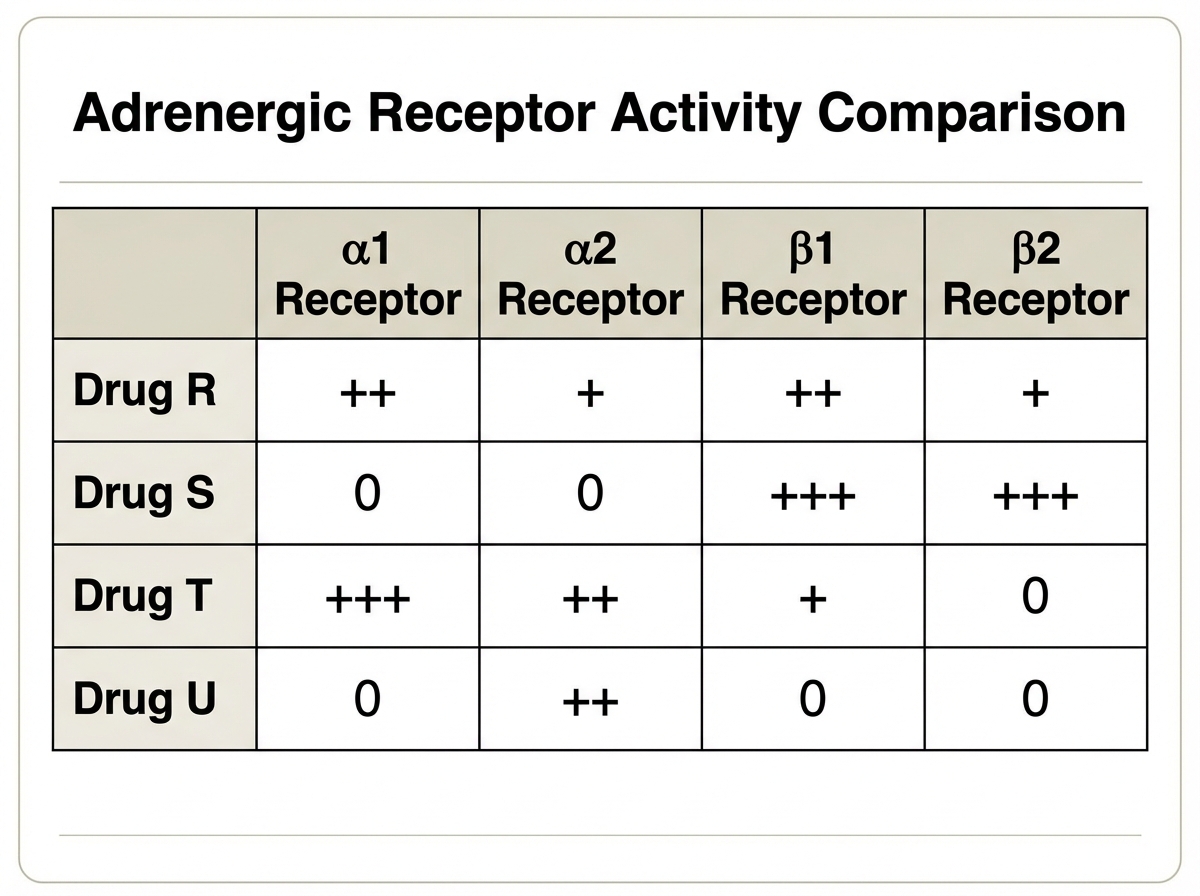
The action of non-competitive muscle blockers is affected by which of the following?
The difference between hyoscine and atropine is that hyoscine:
Which mydriatic agent is typically used for fundoscopic examination?
What is the probable diagnosis in a patient with a dilated pupil not responsive to 1% pilocarpine?
Which of the following drugs produces an action on the dilator pupillae that is analogous to the action of pilocarpine on the sphincter pupillae?
Retroperitoneal fibrosis is seen with which 5HT1 and 5HT2 receptor antagonist?
Which toxin increases the exocytosis of acetylcholine-containing vesicles?
Which of the following is the drug of choice for treating anaphylactic shock?
A patient requires mild cholinomimetic stimulation following surgery. Physostigmine and bethanechol in small doses have significantly different effects on which of the following?
Practice by Chapter
Cholinergic Agonists
Practice Questions
Cholinergic Antagonists
Practice Questions
Adrenergic Agonists
Practice Questions
Adrenergic Antagonists
Practice Questions
Ganglionic Agents
Practice Questions
Neuromuscular Blocking Agents
Practice Questions
Autonomic Drugs in Ophthalmology
Practice Questions
Autonomic Drugs in Cardiovascular Disease
Practice Questions
Autonomic Drugs in Respiratory Disease
Practice Questions
Autonomic Drugs in Urological Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
