Neurology — MCQs

On this page
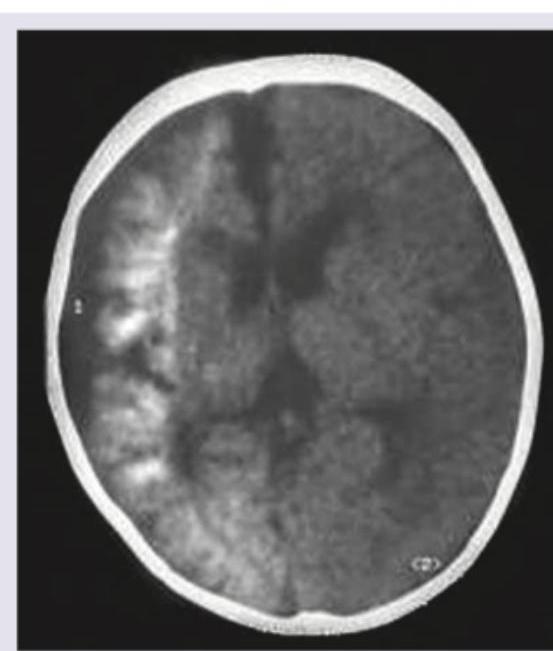
CT scan of a child with intellectual disability, recurrent seizures and hemangioma. Diagnosis is:
Which of the following diseases can lead to the position shown in the image?
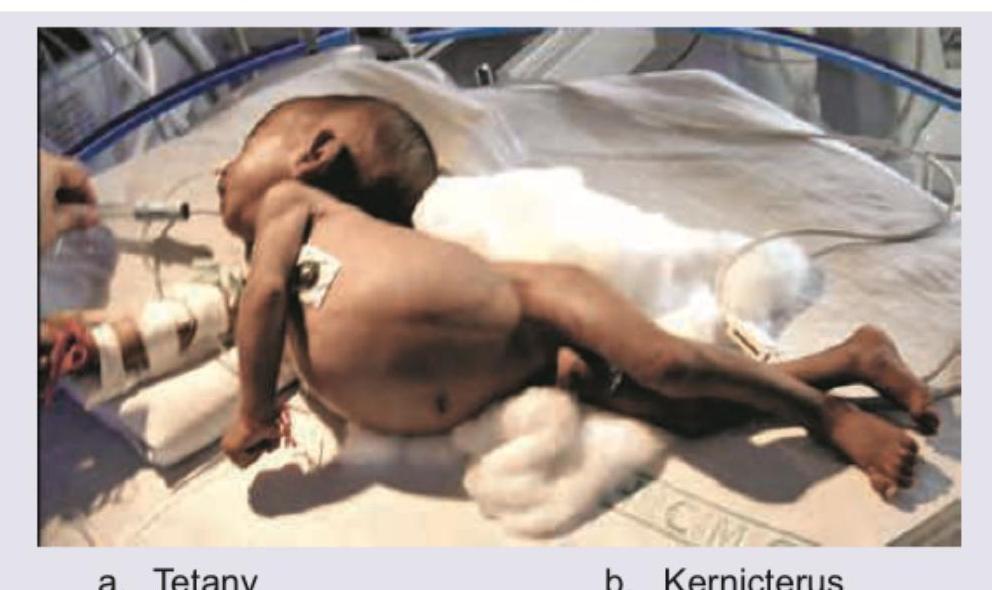
Comment on the diagnosis in this 1-year-old child:
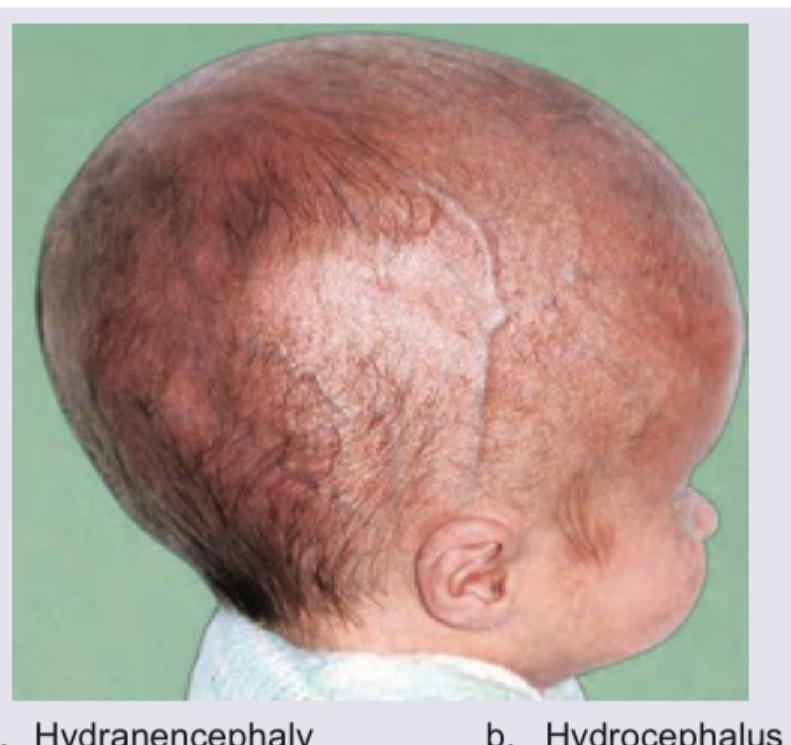
The MRI image shows a smooth brain surface with absence of normal gyri and sulci. What is the diagnosis?
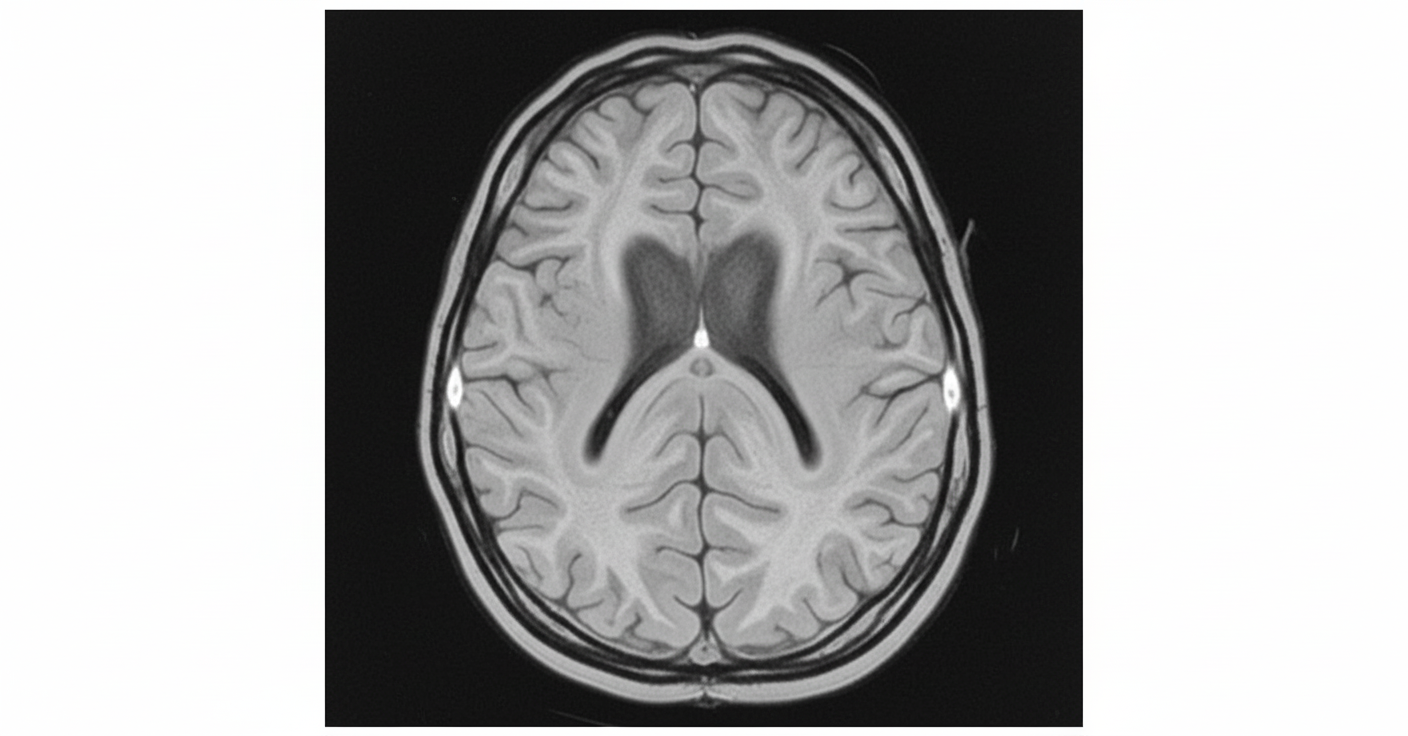
A 7-year-old girl is easily distracted in class and exhibits poor scholastic performance. EEG shows? (AIIMS May 2014)
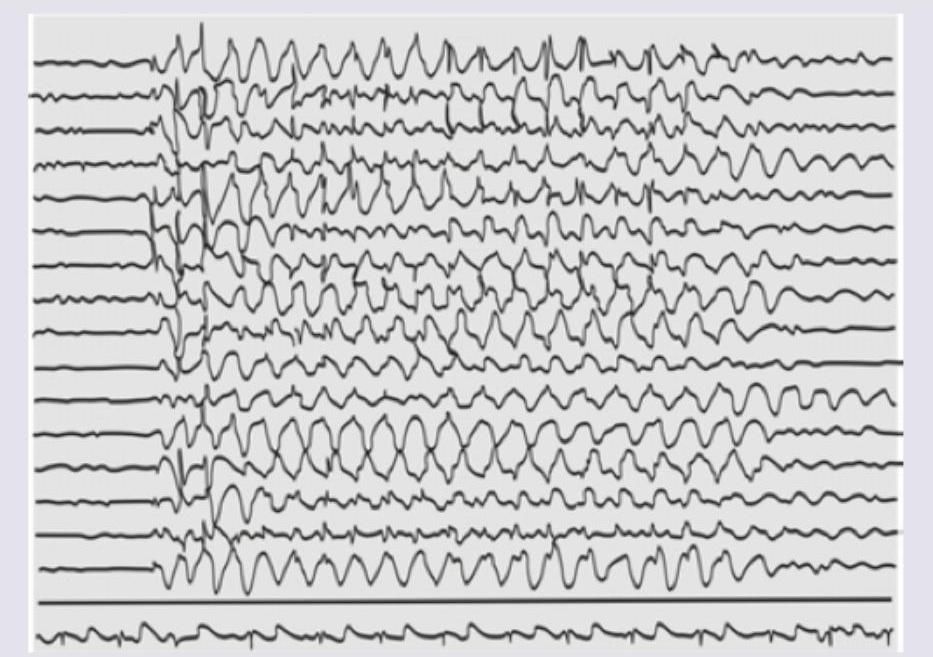
The EEG of an infant with early morning jerks shows?
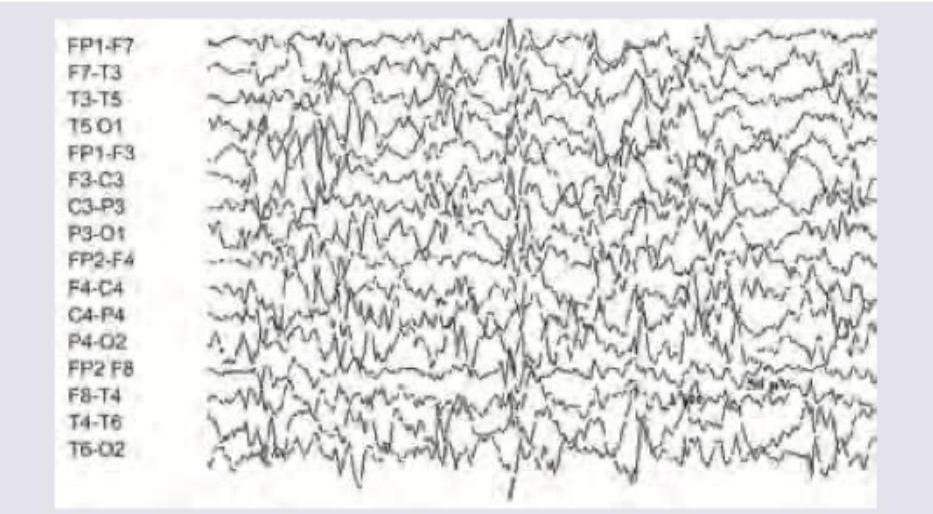
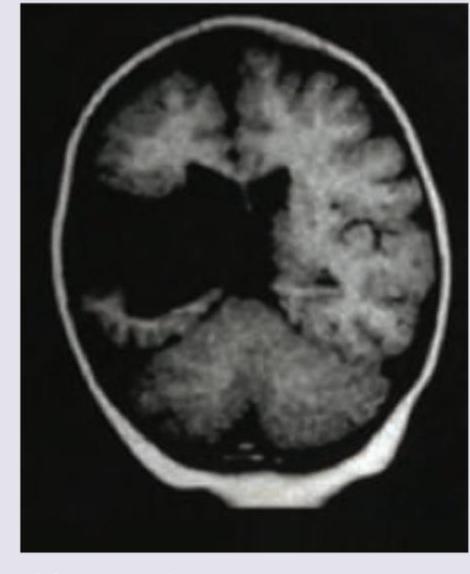
A 2-year-old epileptic child with developmental delay presents to emergency with fever for the last two days. NCCT shows:
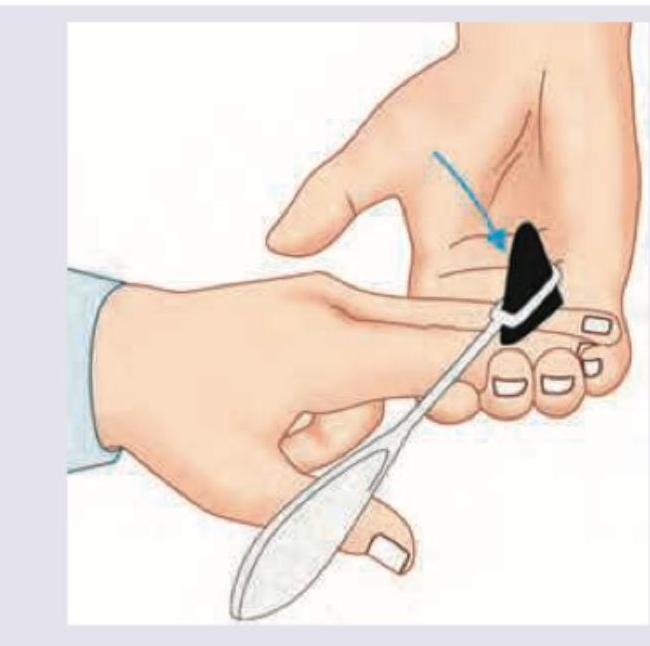
Which reflex is being tested here?
Which of the following are tools commonly used in the evaluation of children with cerebral palsy for motor function and spasticity assessment? I. Gross Motor Function Classification System II. Medical Research Council System III. Modified Connors Scale (Connors-II) IV. Modified Ashworth Scale Select the correct answer using the code given below:
Which one of the following childhood epileptic disorders often needs long term treatment with antiepileptic drugs?
Practice by Chapter
Seizure Disorders and Epilepsy
Practice Questions
Febrile Seizures
Practice Questions
Headache Disorders
Practice Questions
Cerebral Palsy
Practice Questions
Neural Tube Defects
Practice Questions
Neuromuscular Disorders
Practice Questions
Neurodegenerative Disorders
Practice Questions
CNS Infections
Practice Questions
Hydrocephalus
Practice Questions
Movement Disorders
Practice Questions
Traumatic Brain Injury
Practice Questions
Neuroimaging in Pediatrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
