Neurology — MCQs

On this page
A child presents with hepatosplenomegaly & cherry red spots in the eye. He also has developmental regression with normal startle response. Likely enzyme deficiency?
A neonate is found to have multiple hypopigmented macules and ash-leaf spots on Wood's lamp examination. Which of the following is the most likely diagnosis?
A 3-year-old child is brought to the emergency room with a generalized seizure following a high-grade fever. What is the first-line drug of choice for seizure control in this acute febrile setting?
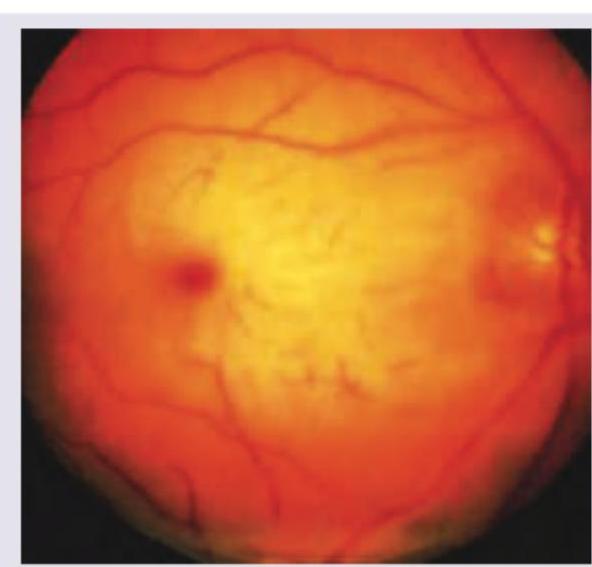
A child presents with regression of milestones and has become blind. On examination spasticity is noted in both legs. Fundus examination is given. What is the diagnosis? (Recent NEET Pattern 2016-17)
A 12-year-old boy presents with difficulty in noting from blackboard in school. Initially refraction error was considered but visual acuity was normal. He has started complaining of diplopia on watching TV or after studying for long. He takes very long time to finish his meals and his speech becomes very difficult to understand after speaking continuously for few minutes. All tests are indicated for diagnosis except?
A 12-year-old boy presents with difficulty in reading from the blackboard in school. Initially refraction error was considered but visual acuity was normal. He has started complaining of diplopia on watching TV or after studying for long. He takes very long time to finish his meals and his speech becomes very difficult to understand after speaking continuously for few minutes. Anti-Acetylcholine receptor blocking antibody is detected in high titers. All are done in management except? (Recent NEET Pattern 2016-17)
A female baby of 6 years presents with the features shown in image. All the following statements regarding this condition are true except:
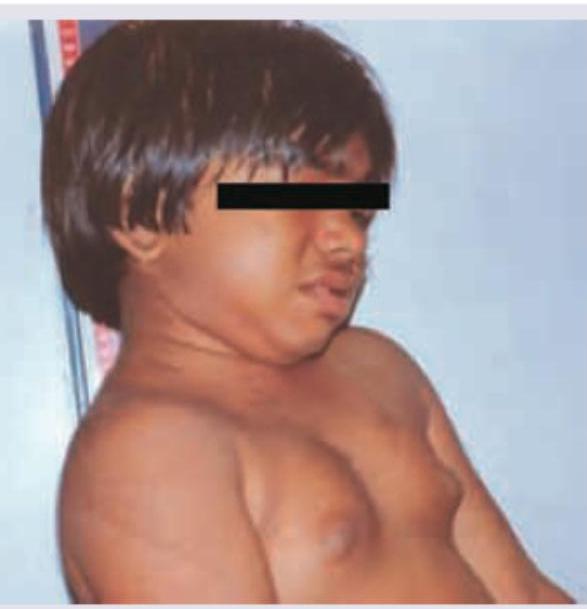
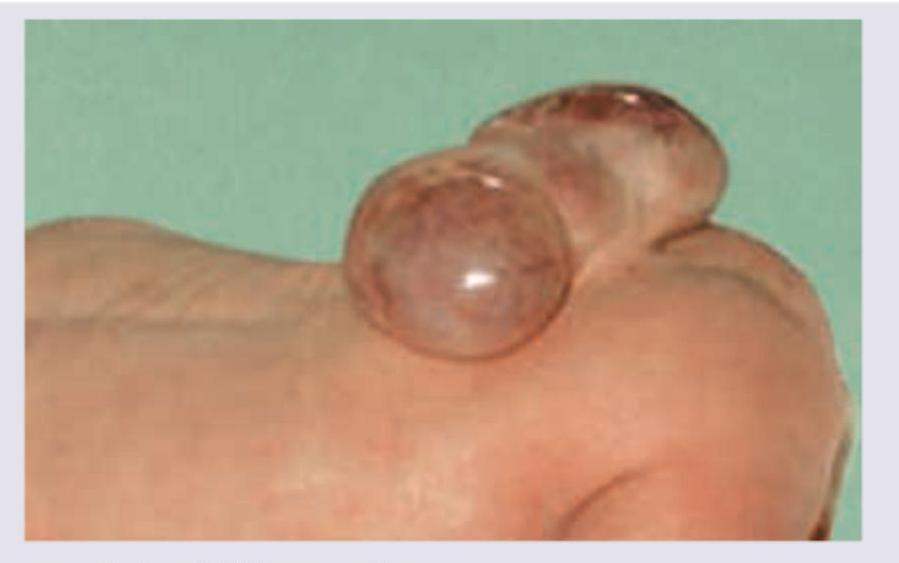
Which neural tube defect is shown here:
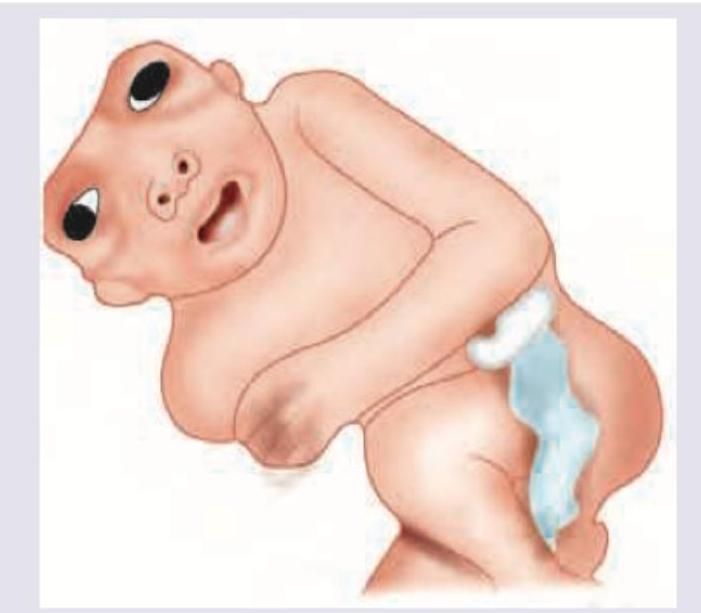
Name the neural tube defect shown here:
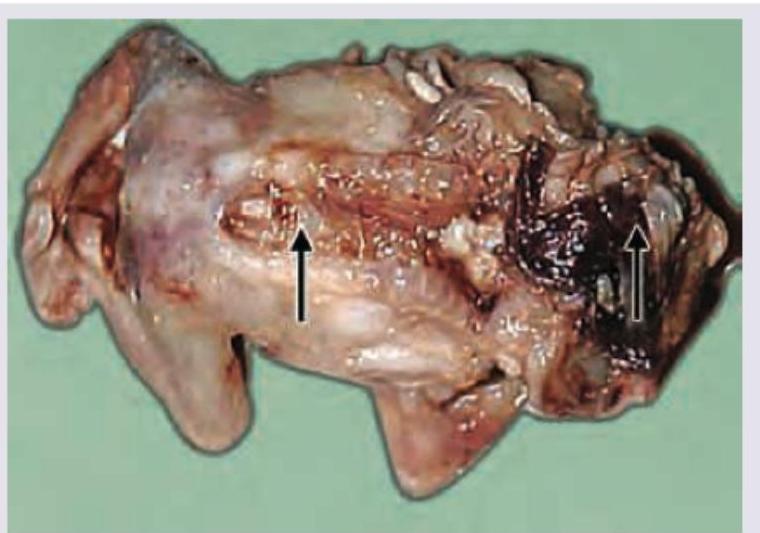
Identify the following congenital defect:
Practice by Chapter
Seizure Disorders and Epilepsy
Practice Questions
Febrile Seizures
Practice Questions
Headache Disorders
Practice Questions
Cerebral Palsy
Practice Questions
Neural Tube Defects
Practice Questions
Neuromuscular Disorders
Practice Questions
Neurodegenerative Disorders
Practice Questions
CNS Infections
Practice Questions
Hydrocephalus
Practice Questions
Movement Disorders
Practice Questions
Traumatic Brain Injury
Practice Questions
Neuroimaging in Pediatrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
