Neurology — MCQs

On this page
What is the drug of choice for treating myoclonus in children?
Hypsarrhythmia in a child is typically associated with which type of epilepsy?
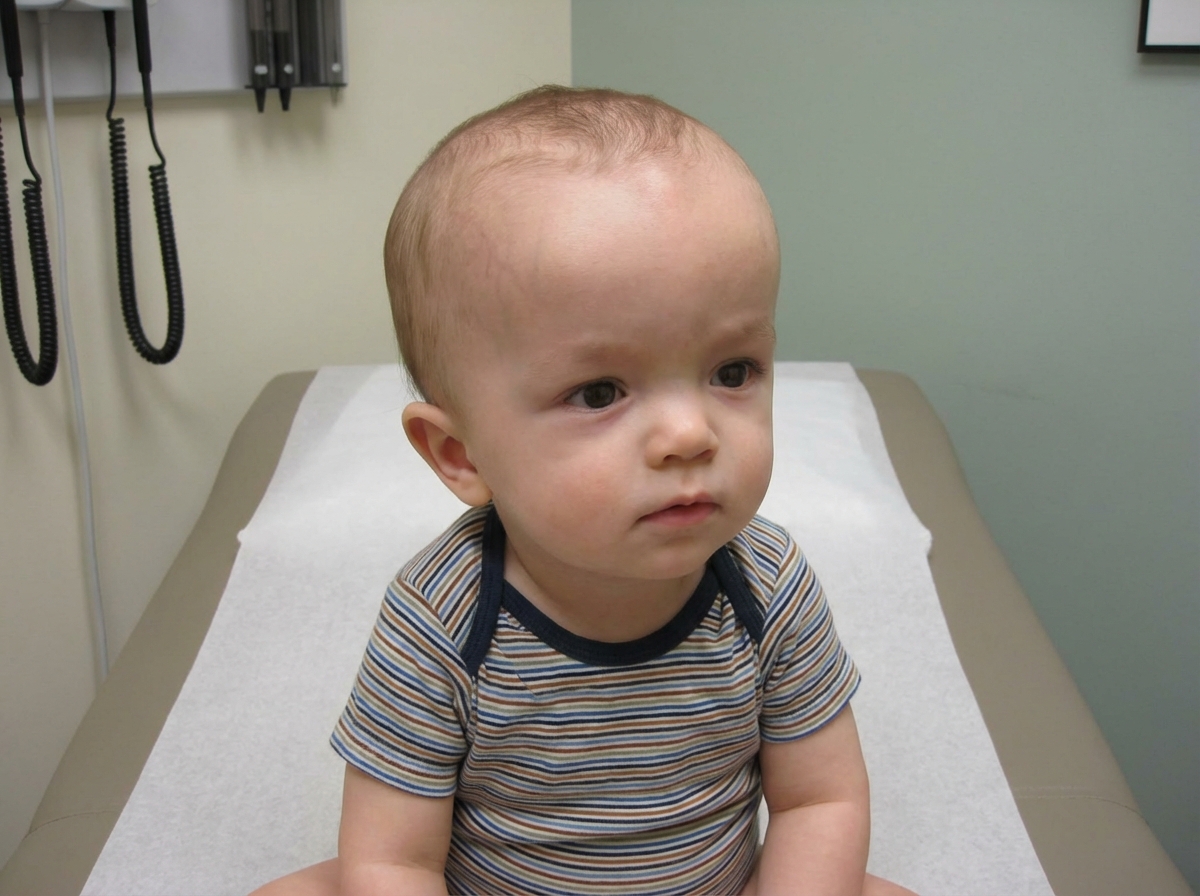
What is the most probable cause of a large head in this child?
A child presents with unilateral facial pigmentation and a history of multiple seizures. Radiography of the skull revealed a specific finding. What is the most likely underlying diagnosis?
Which of the following conditions is associated with vestibular schwannoma, spinal cord astrocytoma, and meningioma?
An 8-month-old child presented with reduced appetite, abdominal distension and pain, and psychomotor retardation. The child was normal at birth, and both parents are normal. On examination: Hepatosplenomegaly, moderate lymphadenopathy, abnormal posturing of the limbs, trunk, and face, impaired voluntary rapid eye movements, cherry-red spot on fundus examination, and bony defects. Lymph node histopathology and electron microscopy findings were noted. Which of the following enzymes is most likely deficient in the above disease?
All of the following predominantly involve the white matter EXCEPT?
Rett's syndrome is associated with a deficiency of which vitamin?
An 8-year-old child with a history of GTCS came with an episode of convulsions for more than 45 minutes. What will be the appropriate management for this patient?
The infant is being evaluated for recurrent episodes of seizures. EEG shows Hypsarrhythmia. Which drug is preferred for management?
Practice by Chapter
Seizure Disorders and Epilepsy
Practice Questions
Febrile Seizures
Practice Questions
Headache Disorders
Practice Questions
Cerebral Palsy
Practice Questions
Neural Tube Defects
Practice Questions
Neuromuscular Disorders
Practice Questions
Neurodegenerative Disorders
Practice Questions
CNS Infections
Practice Questions
Hydrocephalus
Practice Questions
Movement Disorders
Practice Questions
Traumatic Brain Injury
Practice Questions
Neuroimaging in Pediatrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
