Neurology — MCQs

On this page
An 8-year-old boy presents with intellectual deterioration and myoclonus. What is the most likely diagnosis?
A patient diagnosed with febrile convulsions is in the pediatric emergency. Which of the following can be used for the treatment of this patient?
A 5-year-old male presented with a chief complaint of difficulty in climbing stairs and getting up from a sitting position. There was a history of a maternal uncle having the same illness. On examination, there was pseudohypertrophy of the calf muscle. A muscle biopsy was performed. What is your diagnosis?
A newborn is admitted for high-output cardiac failure after presenting with seizures. CT shows dilated lateral ventricles suggestive of hydrocephalus. What is the most probable diagnosis?
Which of the following statements regarding a medulloblastoma in children is true?
Which of the following is not used in the prophylaxis of febrile seizures?
Periventricular leukomalacia most commonly causes which of the following conditions?
What is true about Erb's Palsy?
A patient presents with intractable convulsions, mental defect, and a facial nevus. What is the most likely diagnosis?
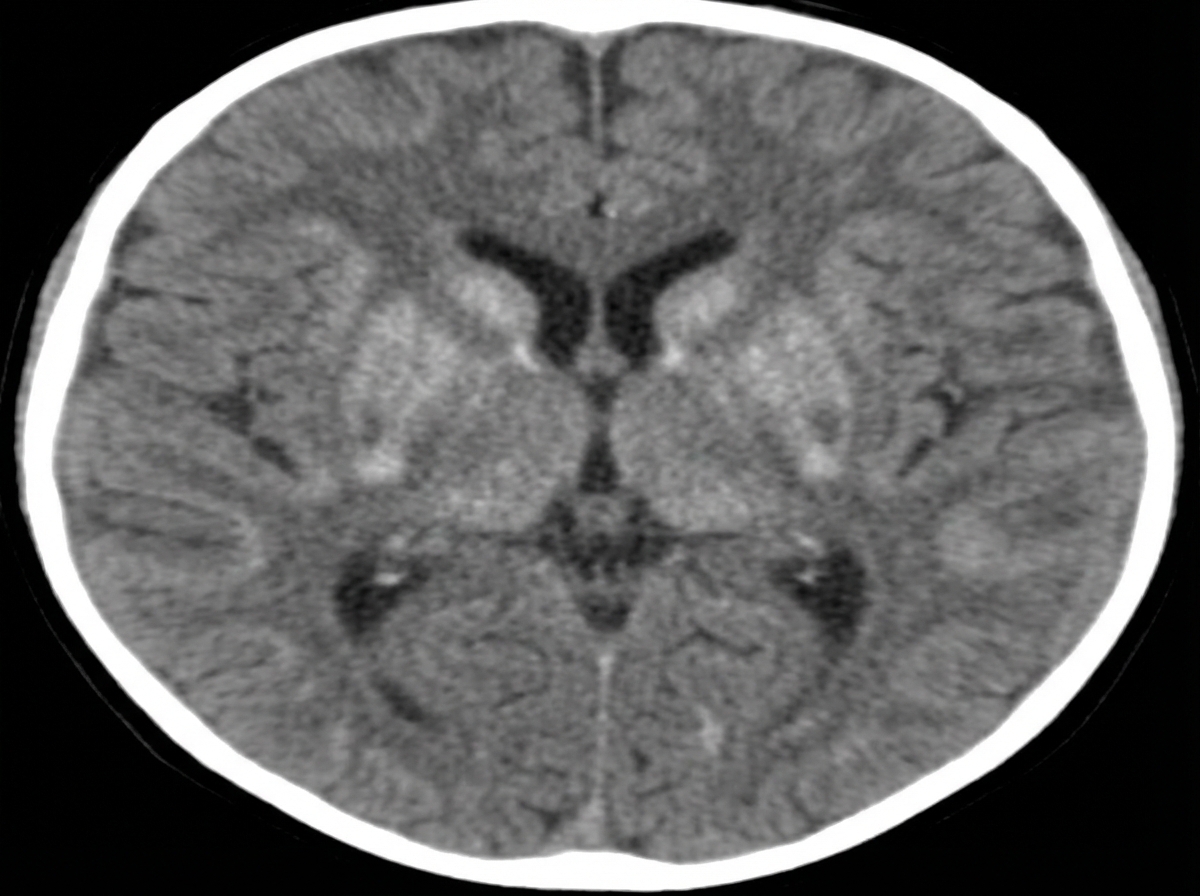
A 4-month-old child presents with excessive irritability and crying, unexplained hyperpyrexia, vomiting, and difficulty feeding for the last 15 days. On admission, the child has rigidity and visual inattentiveness. A CT scan of the brain shows specific findings. What is the probable diagnosis?
Practice by Chapter
Seizure Disorders and Epilepsy
Practice Questions
Febrile Seizures
Practice Questions
Headache Disorders
Practice Questions
Cerebral Palsy
Practice Questions
Neural Tube Defects
Practice Questions
Neuromuscular Disorders
Practice Questions
Neurodegenerative Disorders
Practice Questions
CNS Infections
Practice Questions
Hydrocephalus
Practice Questions
Movement Disorders
Practice Questions
Traumatic Brain Injury
Practice Questions
Neuroimaging in Pediatrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
