Neurology — MCQs

On this page
A 9-year-old boy presented with difficulty in climbing stairs and combing. On examination, his calves are swollen and the child uses his feet to stand up on his legs. What is the next diagnostic step?
A 5-year-old child developed seizures a few months ago. The seizures start with a strange smell (burning rubber), continue with generalized contractions, and end with rhythmic spasms. Consciousness is lost during attacks, and the child is confused afterwards. The child was prescribed phenytoin as the initial treatment. Currently, the parents bring the child for scheduled DTP immunization (diphtheria, tetanus, pertussis). Which of the following is the most appropriate next step in management?
Continuous prophylactic anticonvulsant therapy is not needed in a child with febrile convulsions with which of the following conditions?
Atypical febrile seizures are associated with which of the following?
A child presented to the casualty with seizures. On examination, oval hypo-pigmented macules were noted on the trunk, along with stib-noo:il. What is the probable diagnosis in this child?
A 7-year-old girl presents with recurrent staring spells lasting a few seconds, after which she returns to her previous activities. Her EEG shows 3 Hz spike-and-wave discharges. Which of the following drugs is NOT indicated for treating this child?
All of the following are TRUE regarding Panayiotopoulos syndrome, EXCEPT:
Which of the following is NOT true about migraine in children?
What is true about febrile convulsions?
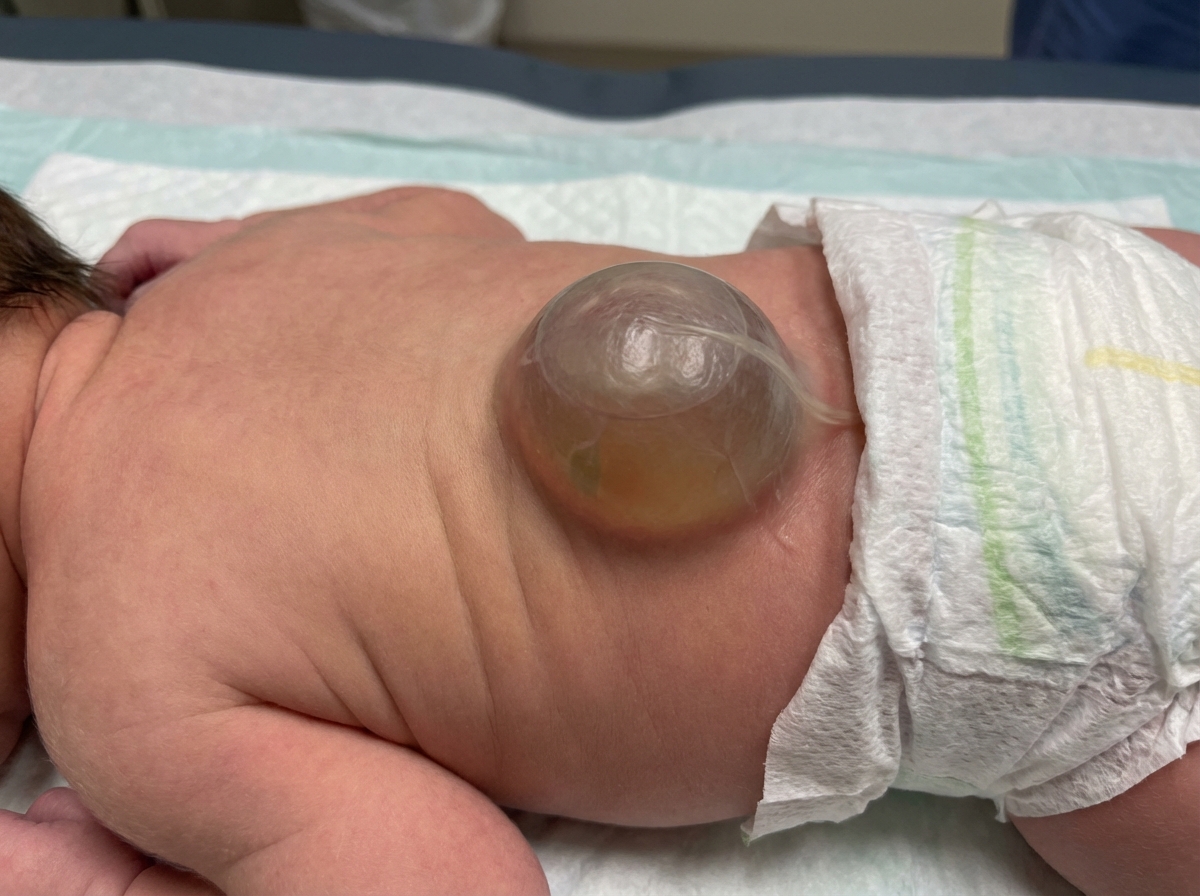
A newborn baby presents with a lumbar mass. What is the most likely diagnosis?
Practice by Chapter
Seizure Disorders and Epilepsy
Practice Questions
Febrile Seizures
Practice Questions
Headache Disorders
Practice Questions
Cerebral Palsy
Practice Questions
Neural Tube Defects
Practice Questions
Neuromuscular Disorders
Practice Questions
Neurodegenerative Disorders
Practice Questions
CNS Infections
Practice Questions
Hydrocephalus
Practice Questions
Movement Disorders
Practice Questions
Traumatic Brain Injury
Practice Questions
Neuroimaging in Pediatrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
