Neurology — MCQs

On this page
What is the most common age group for febrile seizures?
Which corticosteroid is effective in children with cerebral edema?
Which of the following statements about Duchenne muscular dystrophy is false?
An 8-year-old boy presents with difficulty in walking. What is the most likely diagnosis?

What is the commonest cause of non-communicating hydrocephalus in children?
Adrenoleukodystrophy is characterized by which mode of inheritance?
A baby is born with a large red, raised discoloration of the face that persists into adulthood. This type of lesion is most likely a component of which of the following syndromes?
The 'sunset sign' is observed in which of the following conditions?
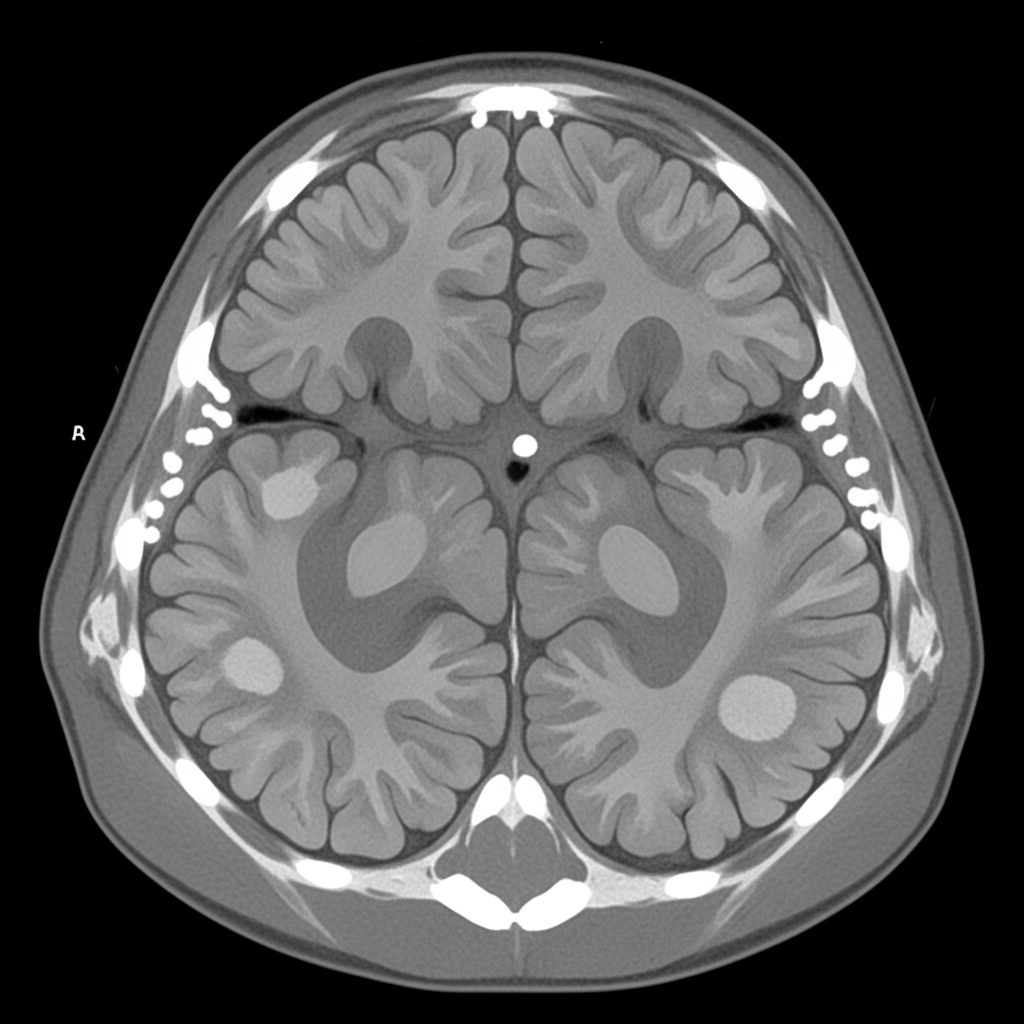
A child with mental retardation and a skin rash on the cheeks undergoes a CT scan. What is the most likely diagnosis?
Which of the following can cause acute flaccid paralysis?
Practice by Chapter
Seizure Disorders and Epilepsy
Practice Questions
Febrile Seizures
Practice Questions
Headache Disorders
Practice Questions
Cerebral Palsy
Practice Questions
Neural Tube Defects
Practice Questions
Neuromuscular Disorders
Practice Questions
Neurodegenerative Disorders
Practice Questions
CNS Infections
Practice Questions
Hydrocephalus
Practice Questions
Movement Disorders
Practice Questions
Traumatic Brain Injury
Practice Questions
Neuroimaging in Pediatrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
