Neurology — MCQs

On this page
Which of the following is NOT a characteristic of typical febrile seizures?
A 6-month-old child presents with multiple episodes of focal seizures, developmental delay, learning difficulties, and ADHD. Examination reveals macrocephaly, hemianopsia, a facial lesion, glaucoma with buphthalmos, and conjunctival and episcleral hemangiomas. Which of the following genes is most likely mutated?
Neurofibromatosis type 2 is associated with which of the following?
Which one of the following is the most common cause of congenital hydrocephalus?
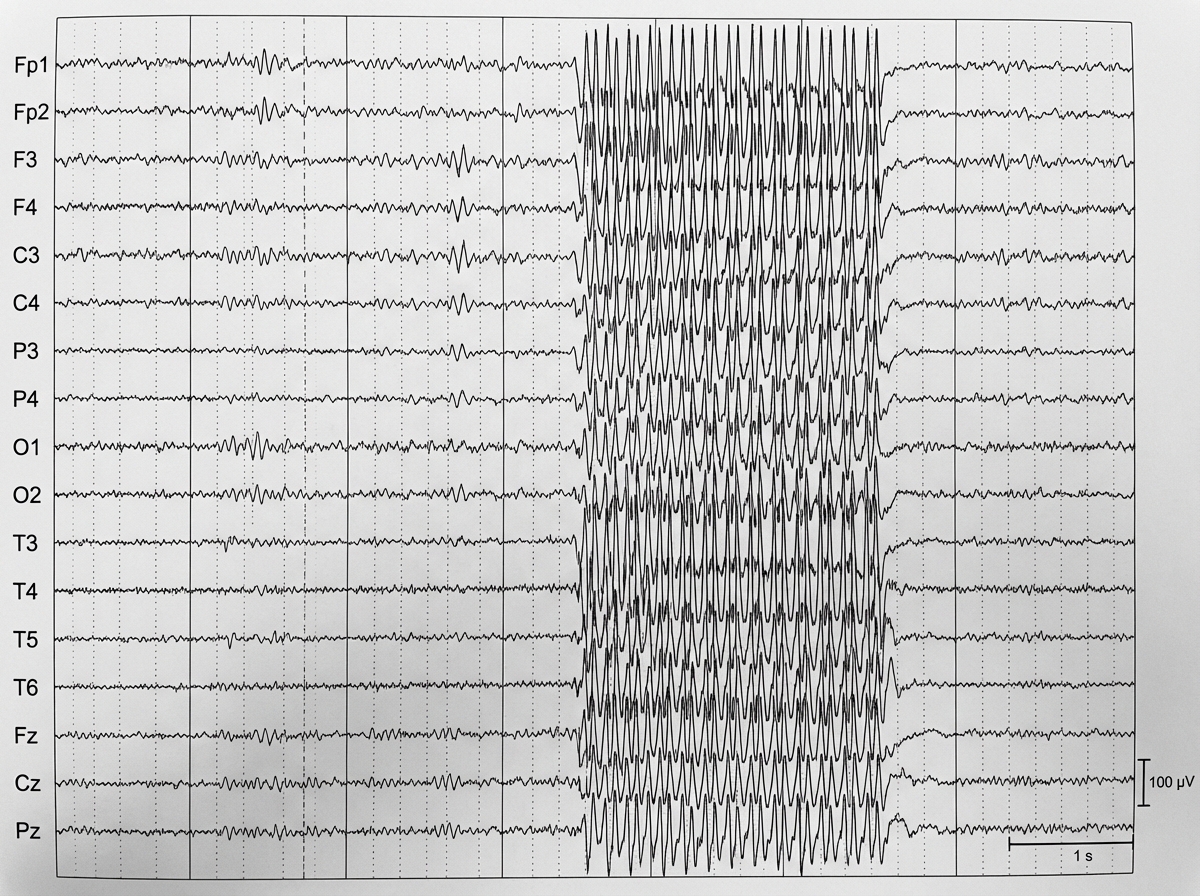
A 7-year-old boy, who gets easily distracted in class with poor academic performance, experiences a seizure episode after hyperventilation. What is the diagnosis suggested by the EEG findings shown in the image?
Foster's test is used in the diagnosis of which condition?
Which of the following leads to communicating hydrocephalus?
Hypotonia with brisk tendon reflexes is typically seen in which condition?
Which of the following statements about hydrocephalus is true?
A 10-year-old girl develops ataxia and hydrocephalus. A CT scan shows a midline cerebellar mass. Which of the following is the most likely diagnosis?
Practice by Chapter
Seizure Disorders and Epilepsy
Practice Questions
Febrile Seizures
Practice Questions
Headache Disorders
Practice Questions
Cerebral Palsy
Practice Questions
Neural Tube Defects
Practice Questions
Neuromuscular Disorders
Practice Questions
Neurodegenerative Disorders
Practice Questions
CNS Infections
Practice Questions
Hydrocephalus
Practice Questions
Movement Disorders
Practice Questions
Traumatic Brain Injury
Practice Questions
Neuroimaging in Pediatrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
