Neurology — MCQs

On this page
In which of the following conditions is the given appearance of calves typically observed?
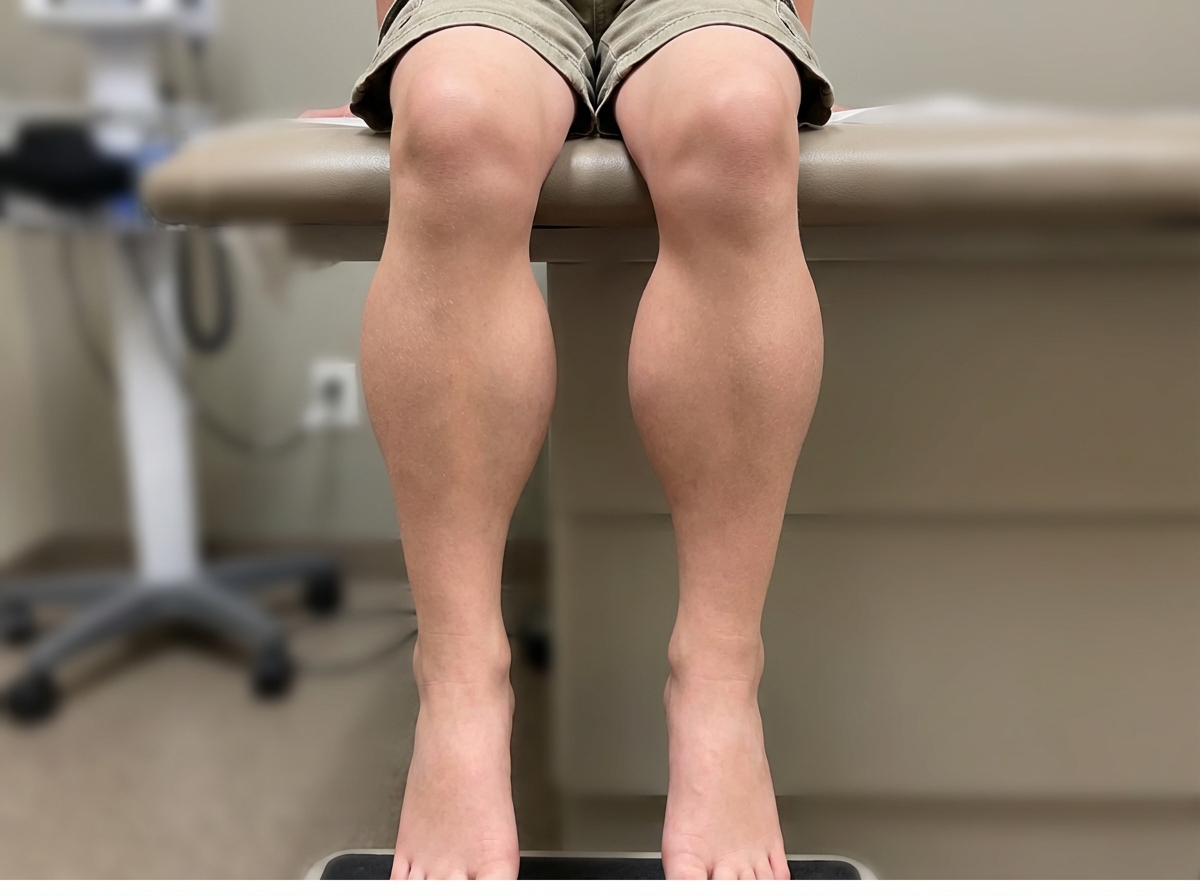
A 10-year-old boy, who was apparently normal at birth, had delayed walking and difficulty in walking. As years passed, weakness increased, and he is now wheelchair-bound. What is your diagnosis?
Which of the following is NOT true regarding breath-holding spells?
Rett's disease is caused by an abnormality in which gene?
Neurofibromatosis type 1 is most commonly associated with which of the following tumors?
A 12-year-old boy presents with weakness in his lower extremities that progressed to include his trunk over several days, following a mild upper respiratory infection. Physical examination reveals weakness without muscle atrophy or pain, and absent lower extremity deep tendon reflexes. Spinal fluid studies show elevated protein only. What is the most likely diagnosis in this patient?
What is the commonest type of seizure observed in newborns?
Spike and Dome pattern is seen in:
What is the drug of choice for neonatal seizures?
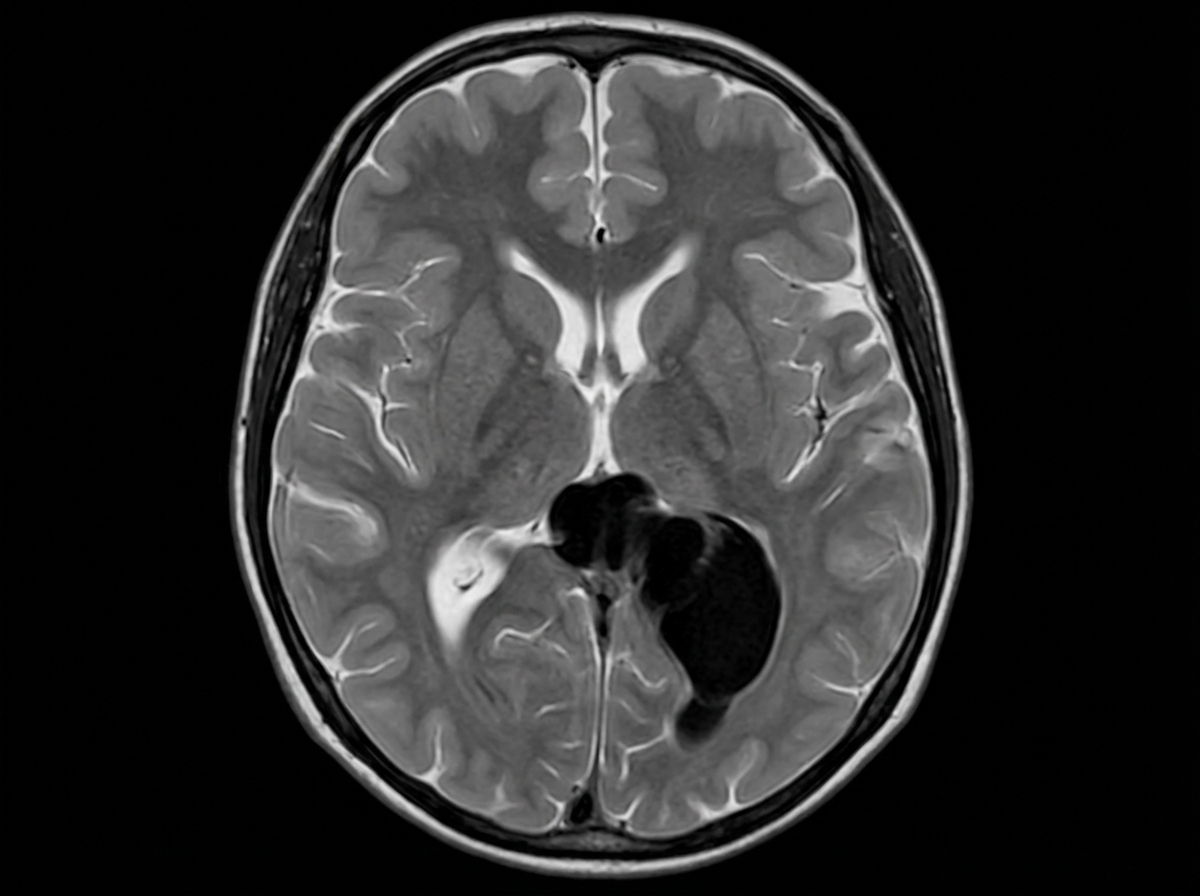
The given clinical condition may present with?
Practice by Chapter
Seizure Disorders and Epilepsy
Practice Questions
Febrile Seizures
Practice Questions
Headache Disorders
Practice Questions
Cerebral Palsy
Practice Questions
Neural Tube Defects
Practice Questions
Neuromuscular Disorders
Practice Questions
Neurodegenerative Disorders
Practice Questions
CNS Infections
Practice Questions
Hydrocephalus
Practice Questions
Movement Disorders
Practice Questions
Traumatic Brain Injury
Practice Questions
Neuroimaging in Pediatrics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
