Neoplasia — MCQs

On this page
Hereditary non-polyposis colorectal cancer (HNPCC), also known as Lynch syndrome, is caused by mutations in which type of genes?
HPV infection is most commonly associated with which type of cancer?
Which of the following is not related to disease progression?
Which of the following is true about p53?
A three-year-old boy has been observed by his parents to be increasingly clumsy for the past 6 months. On a physical examination, there is a cauliflower-like growth in the left eye, leukocoria, and an absent red reflex. The microscopic appearance of the specimen shows Flexner-Wintersteiner rosettes. Which gene is involved in the given condition?
Asbestos exposure may be associated with which of the following malignancies?
Most common cause of squamous cell carcinoma at the base of the tongue is:
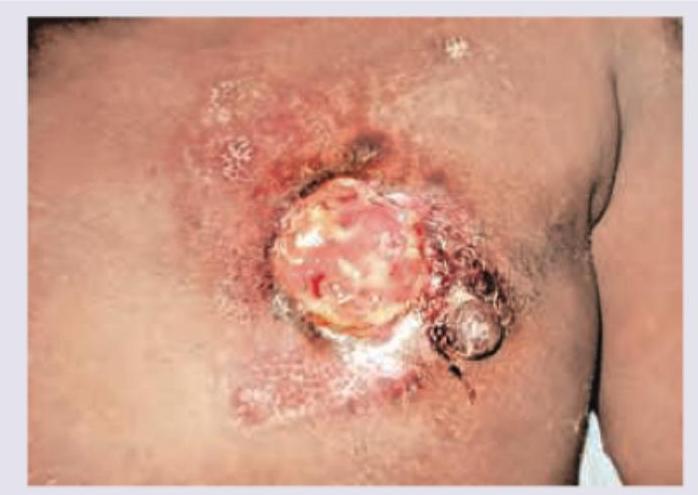
All of the following are true regarding this picture except: (Recent NEET Pattern 2016-17)
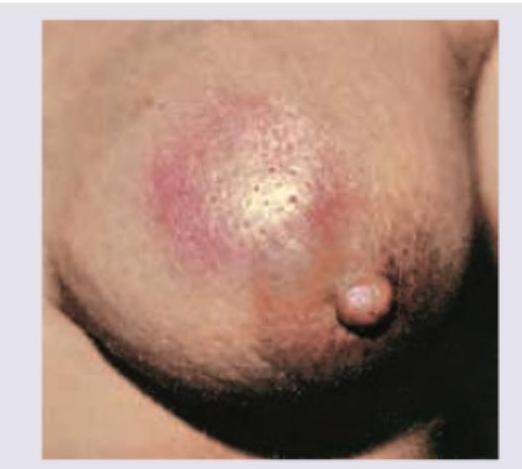
This appearance of mammary skin is due to:
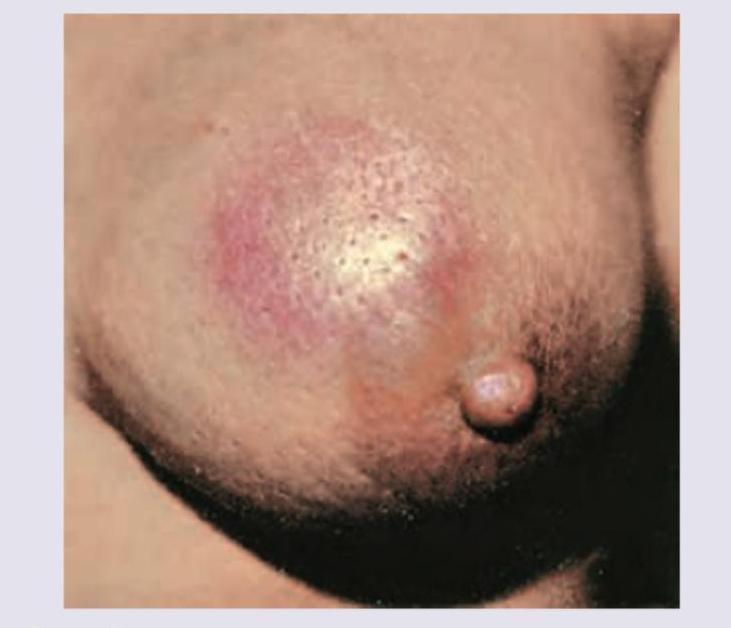
All are true about the condition shown in the image except:
Practice by Chapter
Nomenclature and Classification of Tumors
Practice Questions
Characteristics of Benign and Malignant Neoplasms
Practice Questions
Molecular Basis of Cancer
Practice Questions
Carcinogenesis and Carcinogens
Practice Questions
Tumor Progression and Metastasis
Practice Questions
Tumor Markers
Practice Questions
Paraneoplastic Syndromes
Practice Questions
Genetic Basis of Cancer
Practice Questions
Tumor Immunity
Practice Questions
Cancer Epidemiology and Prevention
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
