Neoplasia — MCQs

On this page
Most commonly, this tumor is due to carcinoma of which of the following organs?
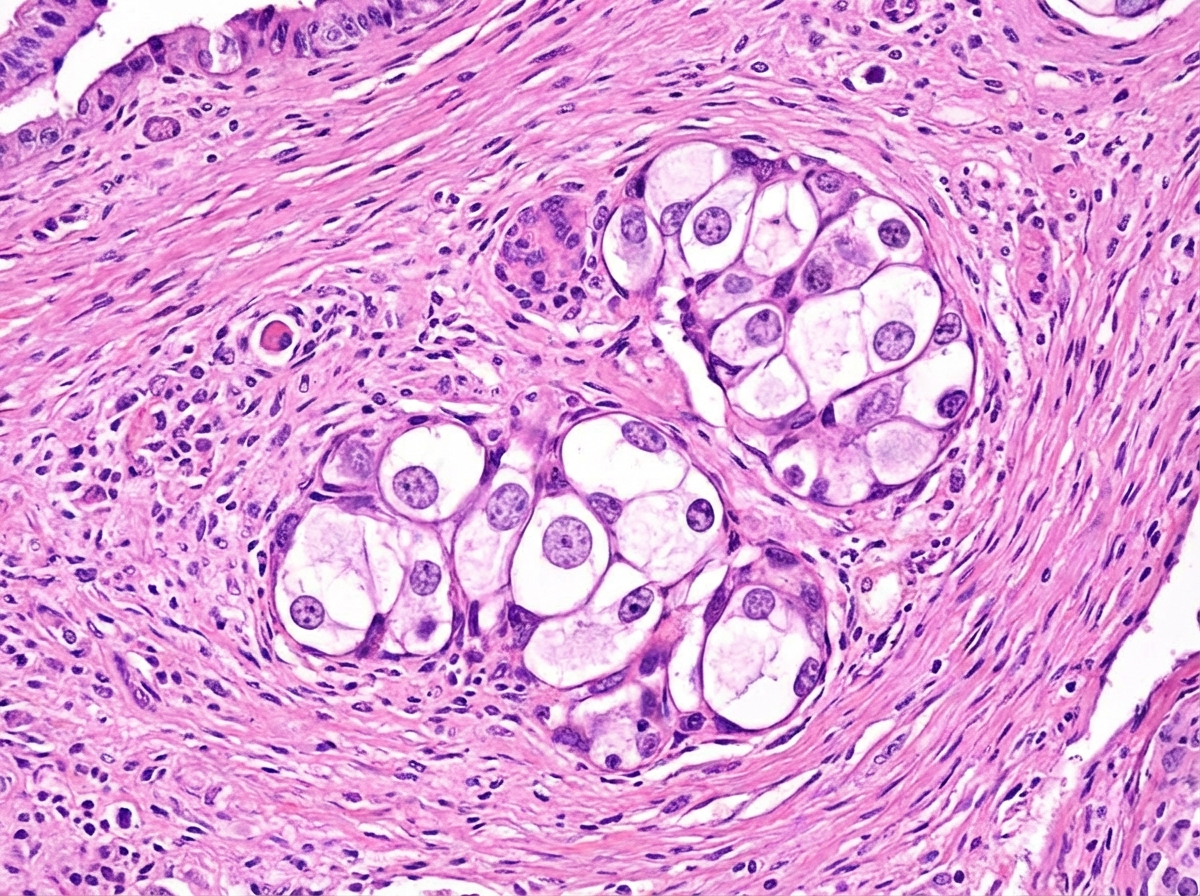
Which of the following describes cells that are abnormal in appearance and may become premalignant?
What is the most common malignant neoplasm of infancy?
Which of the following tumours produces a marked elevation of Alpha fetoprotein?
Psammoma bodies are seen in all except?
Sarcoma botryoides is a type of?
Verrucous carcinoma is an:
What is the paraneoplastic syndrome associated with Hodgkin's disease?
Colon carcinoma is associated with all the following except:
Multiple cutaneous sebaceous adenomas are seen in which of the following conditions?
Practice by Chapter
Nomenclature and Classification of Tumors
Practice Questions
Characteristics of Benign and Malignant Neoplasms
Practice Questions
Molecular Basis of Cancer
Practice Questions
Carcinogenesis and Carcinogens
Practice Questions
Tumor Progression and Metastasis
Practice Questions
Tumor Markers
Practice Questions
Paraneoplastic Syndromes
Practice Questions
Genetic Basis of Cancer
Practice Questions
Tumor Immunity
Practice Questions
Cancer Epidemiology and Prevention
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
