Neoplasia — MCQs

On this page
Which of the following genetic changes is commonly observed in cancers?
What is the most common lymphoma associated with Sicca syndrome?
Which of the following is described as a unicentric, non-functional, anatomically benign, and clinically persistent tumor?
Which electrolyte imbalance is characteristic of tumor lysis syndrome?
All of the following predispose to squamous cell carcinoma, EXCEPT?
A 60-year-old woman presents with a large breast mass that she first detected 3 months ago. Mammography reveals a well-circumscribed mass measuring 8 cm in diameter. A breast biopsy shows loose fibroconnective tissue with a sarcomatous stroma, abundant mitoses, and nodules and ridges lined by cuboidal epithelial cells. What is the most likely diagnosis?
Overexpression of BCL-2 proteins occurs in which of the following conditions?
What is the most important prognostic indicator for Wilms tumor?
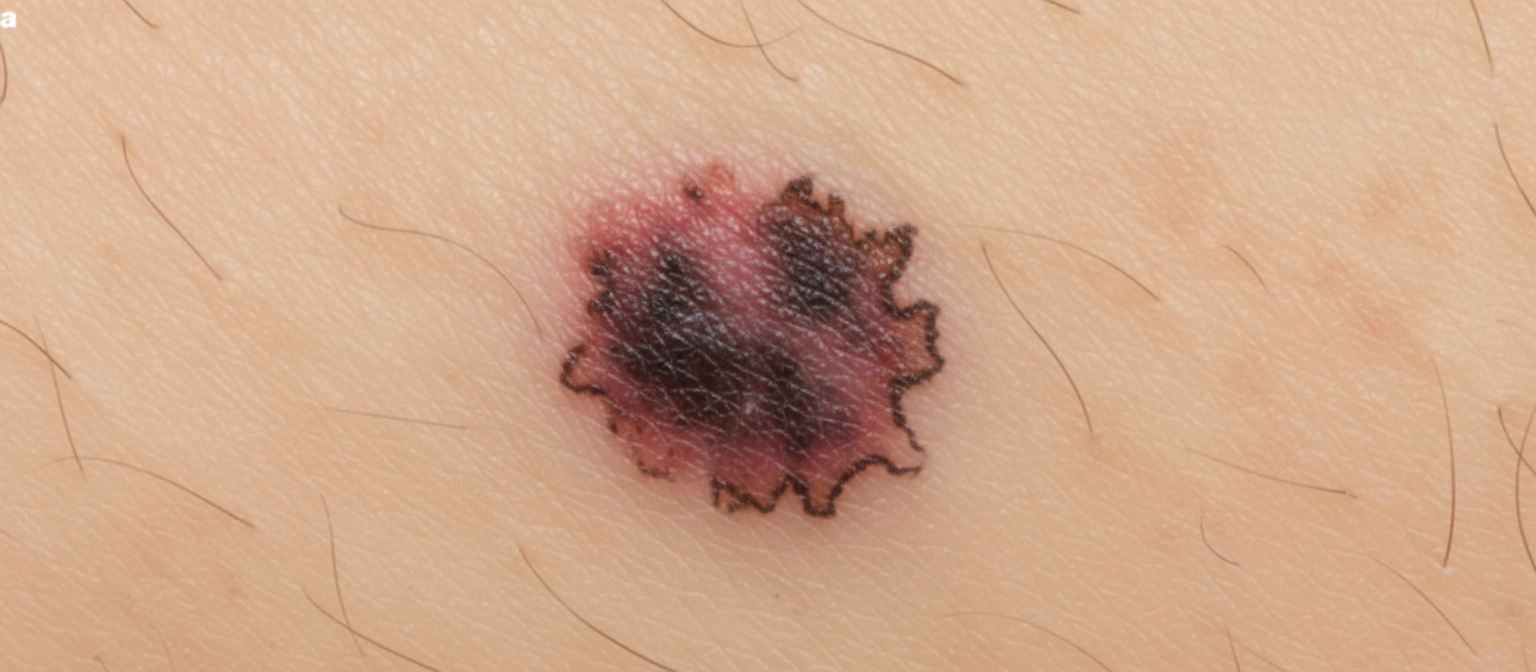
A 48-year-old woman presents with new-onset seizures and behavioral changes that began approximately 6 months ago. Advanced imaging reveals multiple round metastatic lesions in her brain. Her past medical history is remarkable for a black lesion on her toe that was excised 20 years prior. A thorough workup and multiple additional imaging studies reveal no primary malignancy. A lesion on the arm is noted and shown. Which of the following most likely characterizes this type of malignancy?
Which of the following is not a tumor marker?
Practice by Chapter
Nomenclature and Classification of Tumors
Practice Questions
Characteristics of Benign and Malignant Neoplasms
Practice Questions
Molecular Basis of Cancer
Practice Questions
Carcinogenesis and Carcinogens
Practice Questions
Tumor Progression and Metastasis
Practice Questions
Tumor Markers
Practice Questions
Paraneoplastic Syndromes
Practice Questions
Genetic Basis of Cancer
Practice Questions
Tumor Immunity
Practice Questions
Cancer Epidemiology and Prevention
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
