Neoplasia — MCQs

On this page
Which syndrome represents a subset of Carney complex?
How will you differentiate a mediastinal mass being a thymoma or acute lymphoblastic leukemia?
Invasive carcinoma differs from carcinoma in situ by:
Which of the following is the most characteristic ultrastructural feature of paraganglioma on electron microscopy?
Which of the following is a tumor marker?
The lesion shown below is caused by:
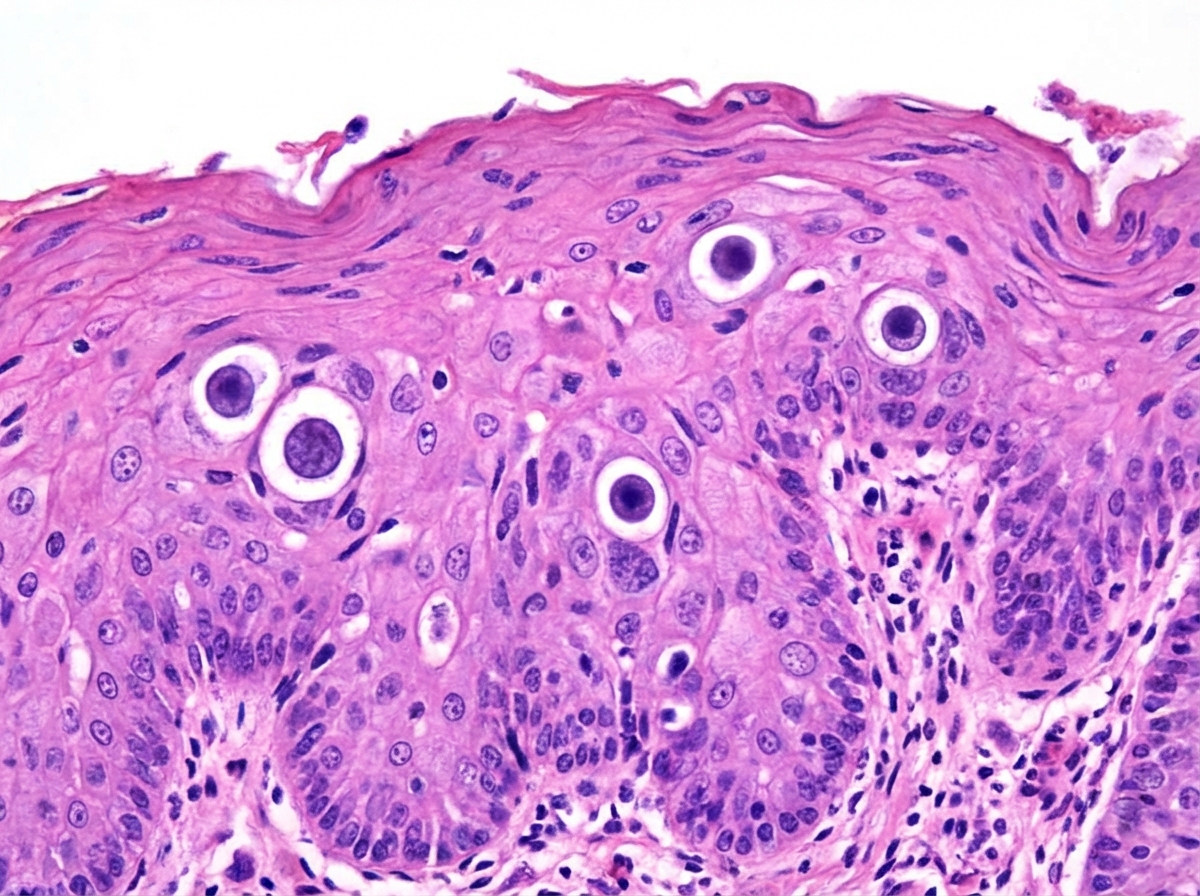
The RET proto-oncogene is associated with which carcinoma?
Which of the following is not a benign neoplasm?
What are the characteristic features of a pleomorphic adenoma?
N-MYC amplification is associated with which tumor?
Practice by Chapter
Nomenclature and Classification of Tumors
Practice Questions
Characteristics of Benign and Malignant Neoplasms
Practice Questions
Molecular Basis of Cancer
Practice Questions
Carcinogenesis and Carcinogens
Practice Questions
Tumor Progression and Metastasis
Practice Questions
Tumor Markers
Practice Questions
Paraneoplastic Syndromes
Practice Questions
Genetic Basis of Cancer
Practice Questions
Tumor Immunity
Practice Questions
Cancer Epidemiology and Prevention
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
