Trauma — MCQs

On this page
An 18 year old boy had a closed lower limb injury while riding his motorbike. He was brought to hospital where on examination he had severe pain which increased on passive movement of affected limb with distal sensory disturbances. What is the probable diagnosis?
In a fracture of shaft of longbone, the component which contributes least in fracture healing is:
Which one of the following statements about Compartment Syndrome is NOT correct?
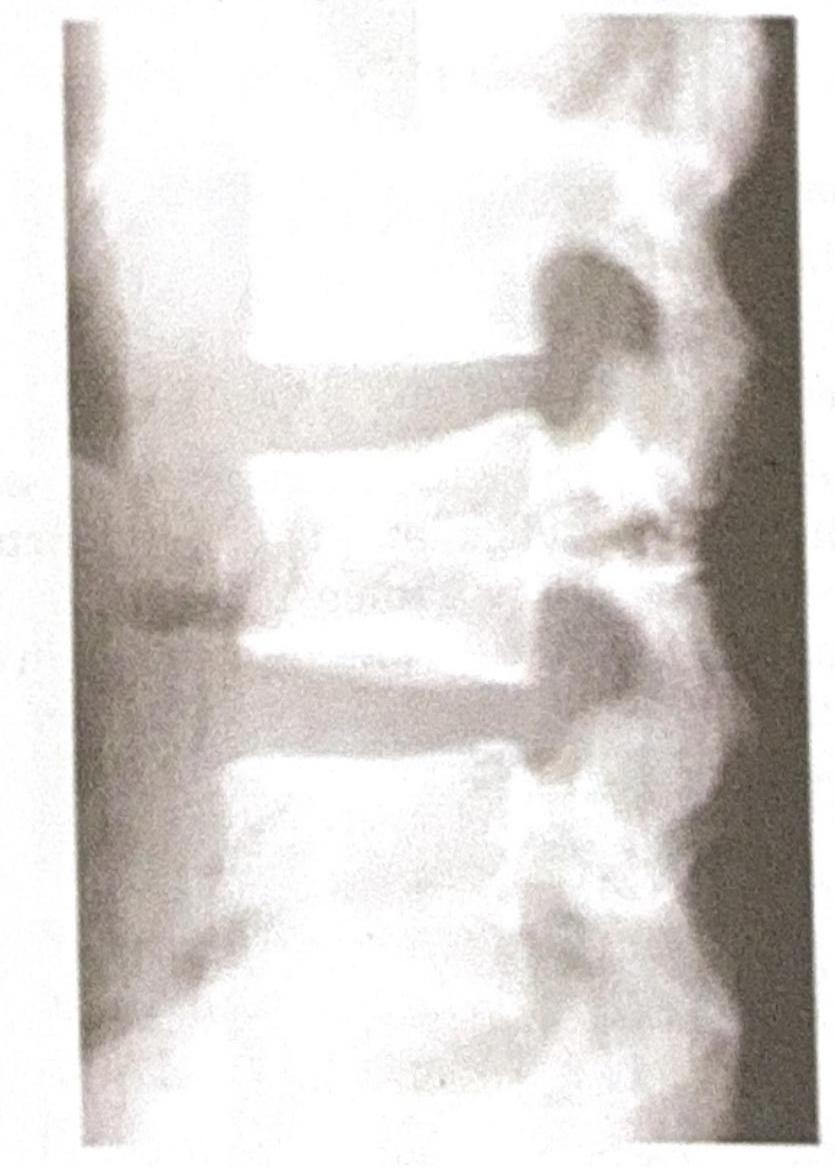
A 35-year-old male presents to the emergency department following a high-speed motor vehicle accident. He complains of severe lower back pain but denies any loss of consciousness or abdominal pain. A lateral X-ray of the lumbar spine is obtained, as shown in the image. The image reveals a horizontal fracture through the vertebral body, extending through the posterior elements. Based on the clinical presentation and imaging findings, what is the most likely diagnosis?
A patient fell off a bicycle and now complains of pain around the hip, with shortening of the affected limb. The hip is held in a position of flexion, adduction, and internal rotation. What is the most likely diagnosis?
Following a road traffic accident, a patient develops type IIIa compound tibial fracture. Arrange the following external fixators in decreasing order of their stability (highest to lowest) 1. Ilizarov fixator 2. Uniplanar with a single rod 3. Uniplanar with double rod 4. Biplanar frame/Ring with a cylindrical rod
Following a femoral shaft fracture, your consultant asks you to provide tibia traction. Which of the following will you request from the nurse? 1. Thomas splint 2. K-wire 3. Steinmann pin 4. Denham's pin 5. Bohler's stirrup 6. Bohler Braun splint
A 30-year-old male presents with pain and limited movement in his shoulder following a fall. X-ray reveals an anterior dislocation of the glenohumeral joint. Which of the following structures is most likely to be damaged in this injury?
Most common complication of extra capsular fracture of neck of femur is:
Which nerve is commonly damaged in fracture of neck of fibula?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
