Trauma — MCQs

On this page
A 23 year old male epileptic patient presented with pain in right shoulder region. Examination revealed that right upper limb was abducted and externally rotated and the movements could not be performed. Which of the following is the most likely diagnosis?
The diagnosis in a patient who is unable to perform internal and external rotation of the hip is?
A patient is referred to a higher center with the diagnosis of fracture. On examination, the forearm pulses were not palpable. An upper arm X-ray was done, which is given below. Which artery is most likely to be injured in this condition?
An 80-year-old female patient with a history of slip and fall in the bathroom was brought to the casualty. She is having pain in the left hip and is unable to walk. She has no history of osteoarthritis. On examination, the left lower limb is shortened and externally rotated. X-ray findings are shown below. How will you manage this patient?
A 60-year-old female patient complains of pain and swelling in the left wrist following a fall on an outstretched hand. On examination, dinner fork deformity can be noticed. What is the most likely displacement seen in this patient?
A 65-year-old osteoporotic female falls on her outstretched hand and presents with severe wrist pain and deformity. X-ray shows a distal radius fracture with dorsal angulation of 25°, radial shortening of 8mm, and intra-articular extension with 3mm step-off at the radiocarpal joint. Ulnar styloid is also fractured. Which of the following treatment options provides the best functional outcome and lowest complication rate in this patient?
A teenager presents to the emergency department with wrist pain after falling off his skateboard. He has snuff-box tenderness. Which bone is likely fractured?
What is the preferred treatment for an inter-trochanteric fracture in a 72-year-old female?
A 25-year-old man presents to the emergency department following a motorbike accident and is found to have a closed midshaft fracture of the left tibia. Six hours later, he develops severe leg pain that is disproportionate to the injury and worsens with passive dorsiflexion of the foot. The pain is not relieved by analgesics. On examination, dorsalis pedis and posterior tibial pulses are present, but there is no sensation over the first dorsal webspace. What is the most appropriate next step in management?
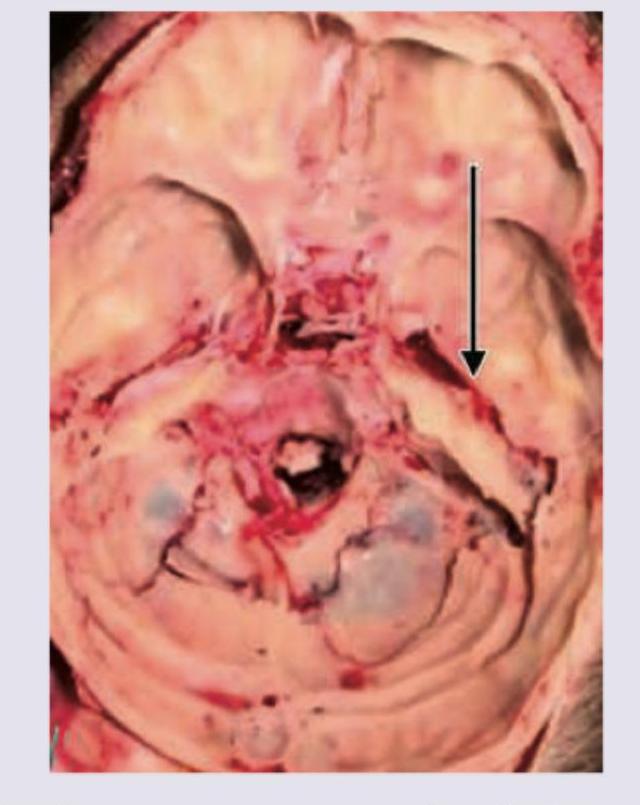
Identify the fracture given in the image given below:
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
