Trauma — MCQs

On this page
Which of the following laboratory findings is NOT typically seen in fat embolism?
Pipkin classification is used for which type of fracture?
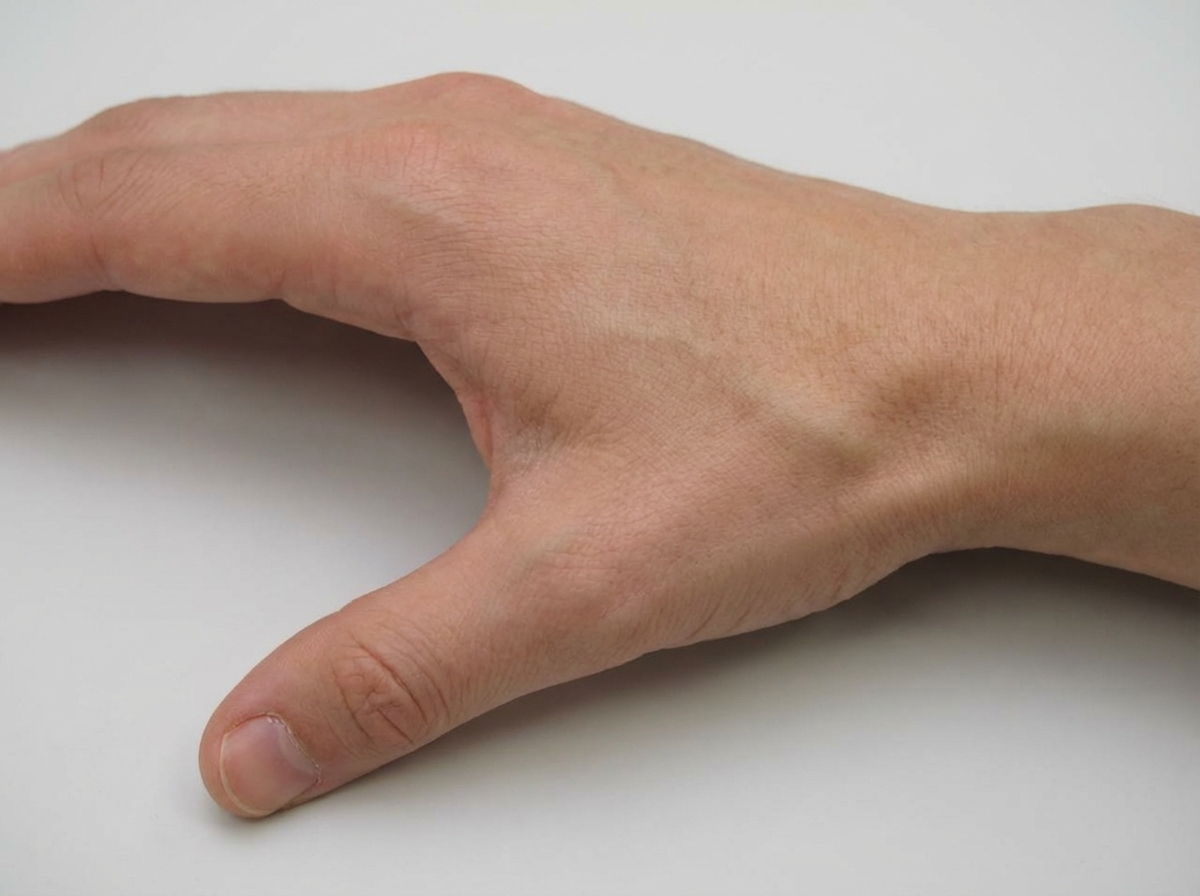
An injury to the shown area can lead to fracture of which bone?
Non-union is a complication of which of the following fractures?
Ruptured tendon is most commonly seen in which of the following conditions?
All of the following statements about dislocation of the shoulder are true, except?
Shoeing of the lower limb with abduction and internal rotation is observed in which of the following types of hip dislocation?
A 45-year-old female has a history of a slip in the bathroom, complaining of right hip pain and tenderness in Scarpa's triangle. The X-ray is normal. What is the next investigation?
Which is the most commonly injured tarsal bone?
The posterolateral lesion in the head of humerus in cases of recurrent anterior shoulder dislocation is:
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
