Trauma — MCQs

On this page
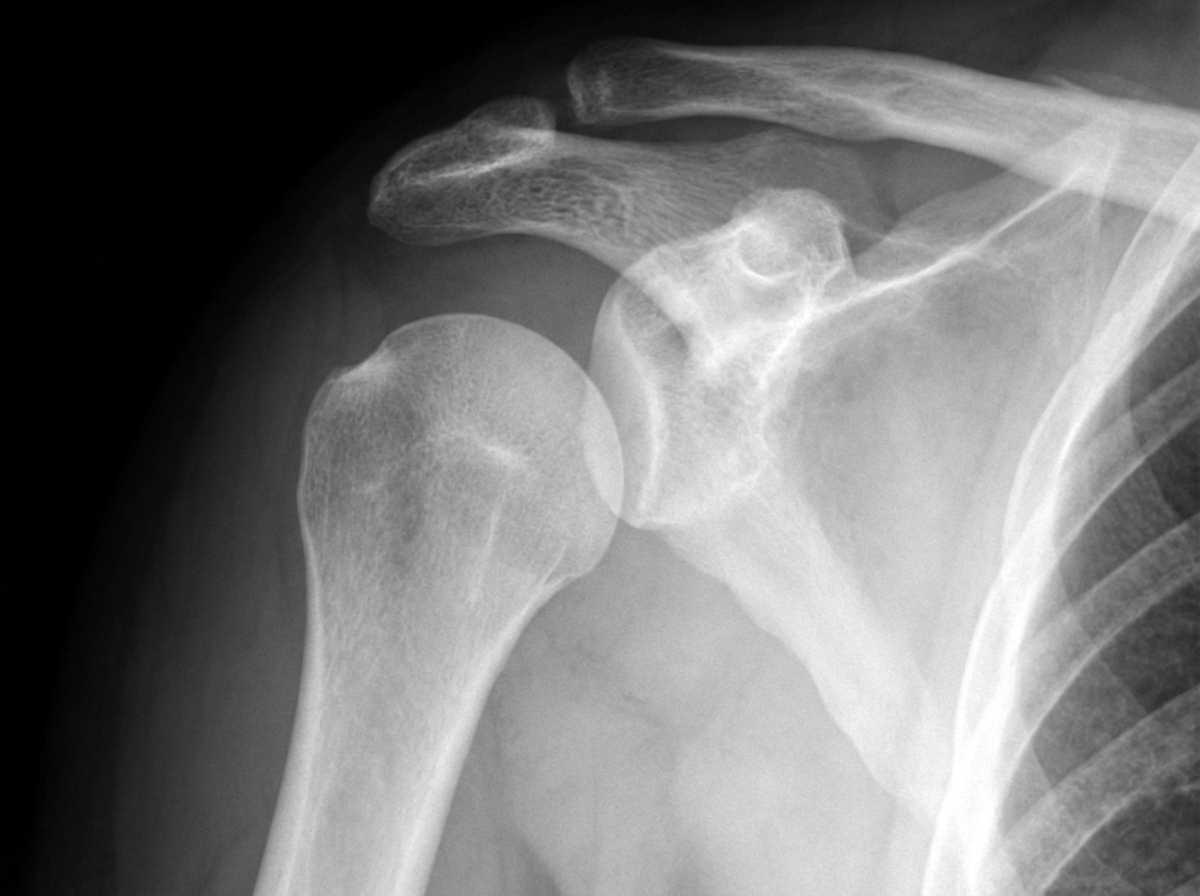
A 54-year-old male patient sustained a right upper limb injury in a road traffic accident and presented to the emergency room unable to move his right arm. Radiographic findings are shown. Which of the following nerves is most likely injured?
Which of the following is NOT a major criterion for Gurd?
What is the commonest site for osteochondritis dissecans in the elbow?
High-stepping gait is characteristic of which condition?
For which of the following conditions is a TT splint NOT indicated?
A person presents 3 days post Colles' fracture with inability to extend the thumb. What is the most likely cause?
Long compression is used for which fracture?
What is the most common fracture in the elderly?
Cubital tunnel syndrome involves which nerve?
In a posteriorly dislocated elbow, which nerve is most commonly involved?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
