Trauma — MCQs

On this page
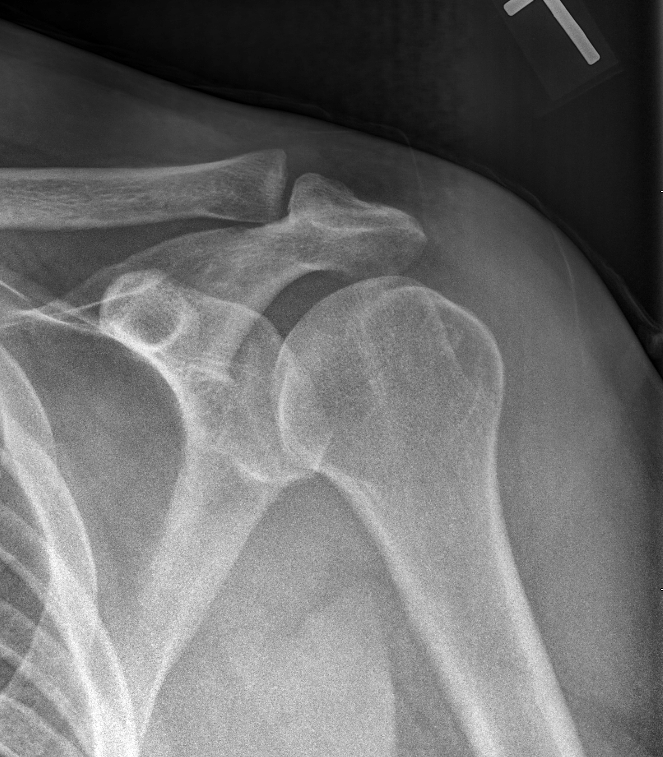
A 21-year-old man presents with shoulder pain after falling off his bike. What is your diagnosis?
The Nexus criteria is used for the assessment of which type of injury?
What structures are included in the terrible triad of O'Donoghue?
What is the absolute pressure threshold for indication of surgical compartment release in compartment syndrome?
After bone fracture, primary healing will show which of these features?
The Mangled Extremity Severity Score includes all of the following except?
What is the treatment of choice in acute myositis ossificans?
Compartment syndrome is treated by:
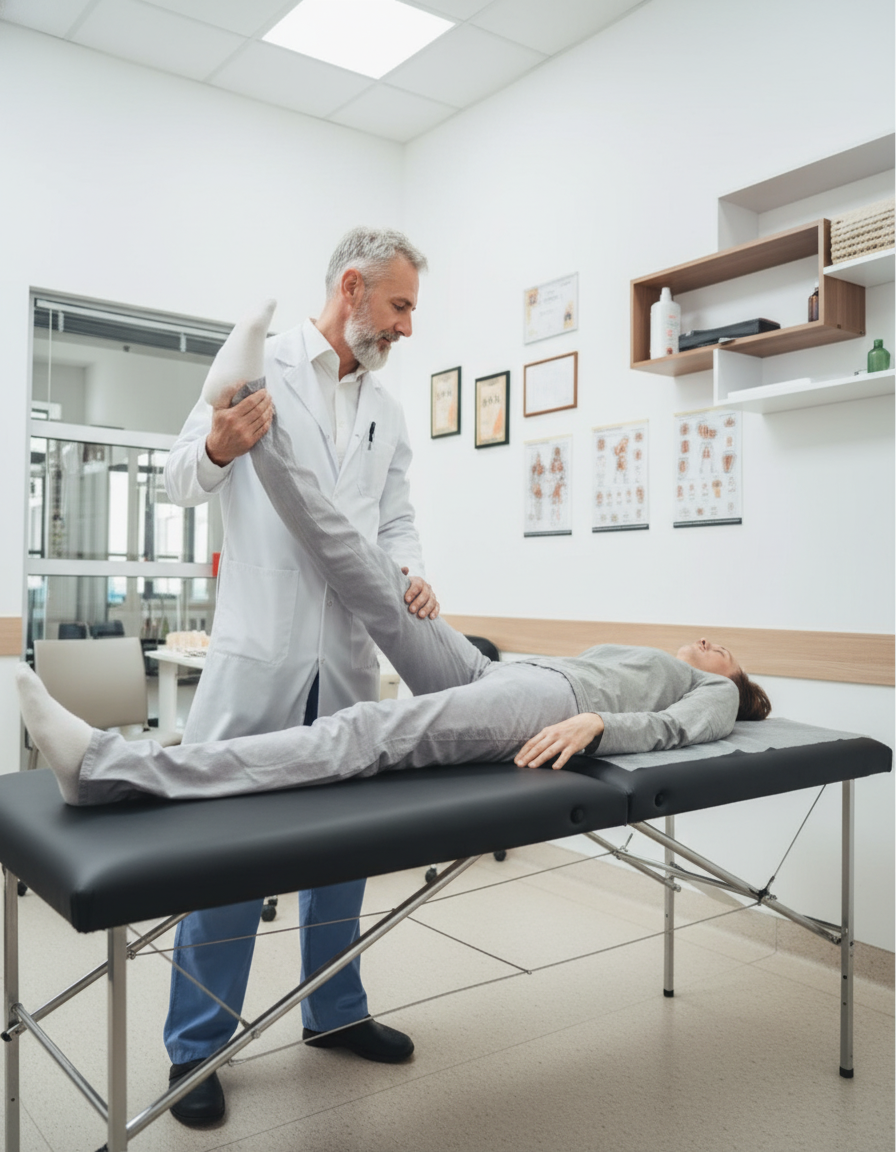
What condition is the given test used for?
A patient sustained an upper limb injury 3 years ago and now presents with a valgus deformity of the elbow and paresthesias over the medial border of the hand. What is the likely nature of the original injury?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
