Trauma — MCQs

On this page
Anterolateral avulsion fracture of the distal tibial physis is known as?
A 50-year-old male patient presented with a fracture as shown in the x-ray. On examination, there was paralysis of most of the intrinsic muscles of the hand and loss of sensation from the medial 1.5 palmar surface of fingers. Which of the following nerves arise from the same cord as the injured nerve, except?
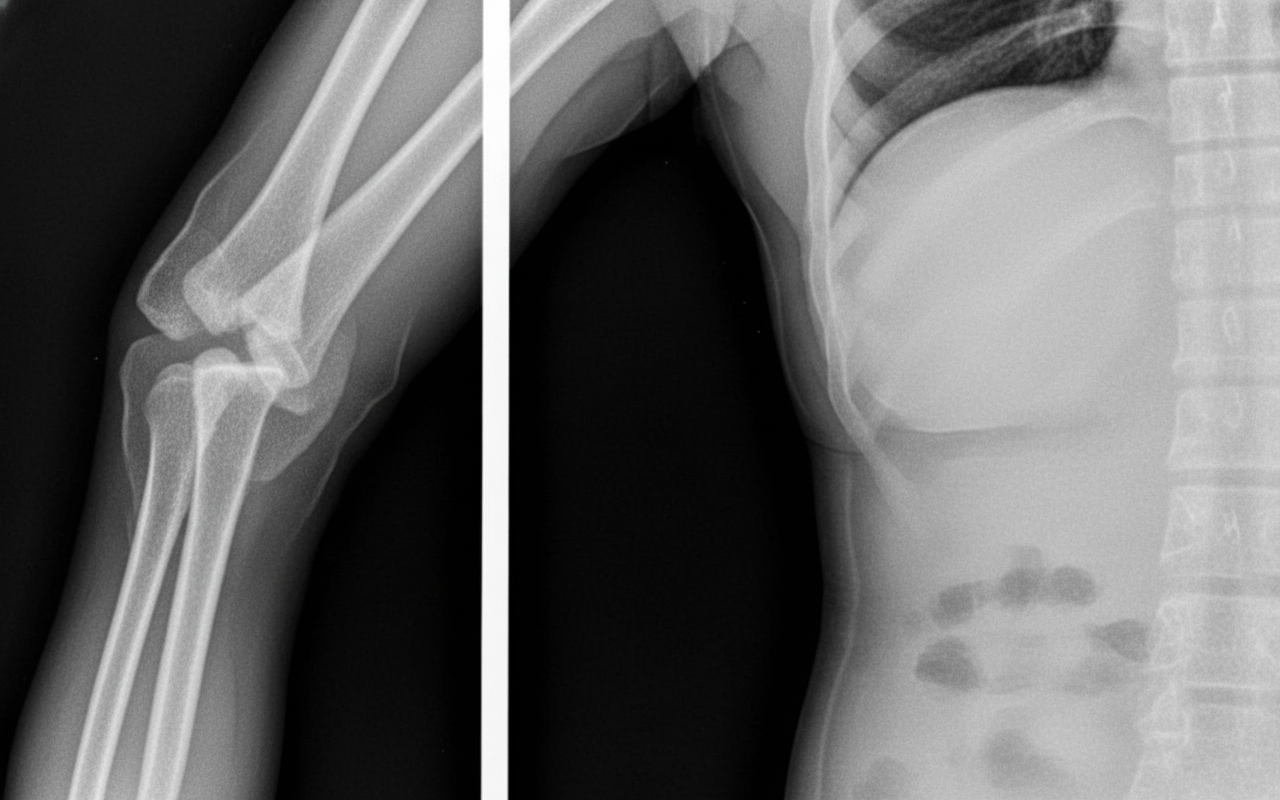
Which of the following arteries is affected in anterior shoulder dislocation?
In a supracondylar fracture of the humerus, to which direction is the distal segment most commonly displaced?
Which of the following is NOT a characteristic feature of acute compartment syndrome in the lower leg?
What is the best investigation for the detection of a stress fracture?
What is Mallet finger?
March fracture involves which of the following bones?
In posterior dislocation of the elbow, which bony prominence is most apparent?
Hangman's fracture occurs at which of the following vertebral levels?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
