Trauma — MCQs

On this page
A 22-year-old male is admitted with a fracture of the left femur. Two days later, he becomes mildly confused, has a respiratory rate of 40/min, and a scattered petechial rash on his upper torso. Chest X-ray shows patchy alveolar opacities bilaterally. His arterial blood gas analysis is abnormal. What is the most likely diagnosis?
Growth disturbance, nonunion, elbow instability, and late ulnar nerve palsy are commonly seen in which type of fracture?
What is the change in Gissane's angle in an intra-articular fracture of the calcaneum?
What is the last step in fracture healing?
Which nerve is most commonly involved in a fracture of the neck of the humerus?
A bucket handle tear occurs at the knee joint due to which of the following injuries?
Which of the following are considered non-rigid fixation devices?
What is the most important sign of Volkmann's ischemia?
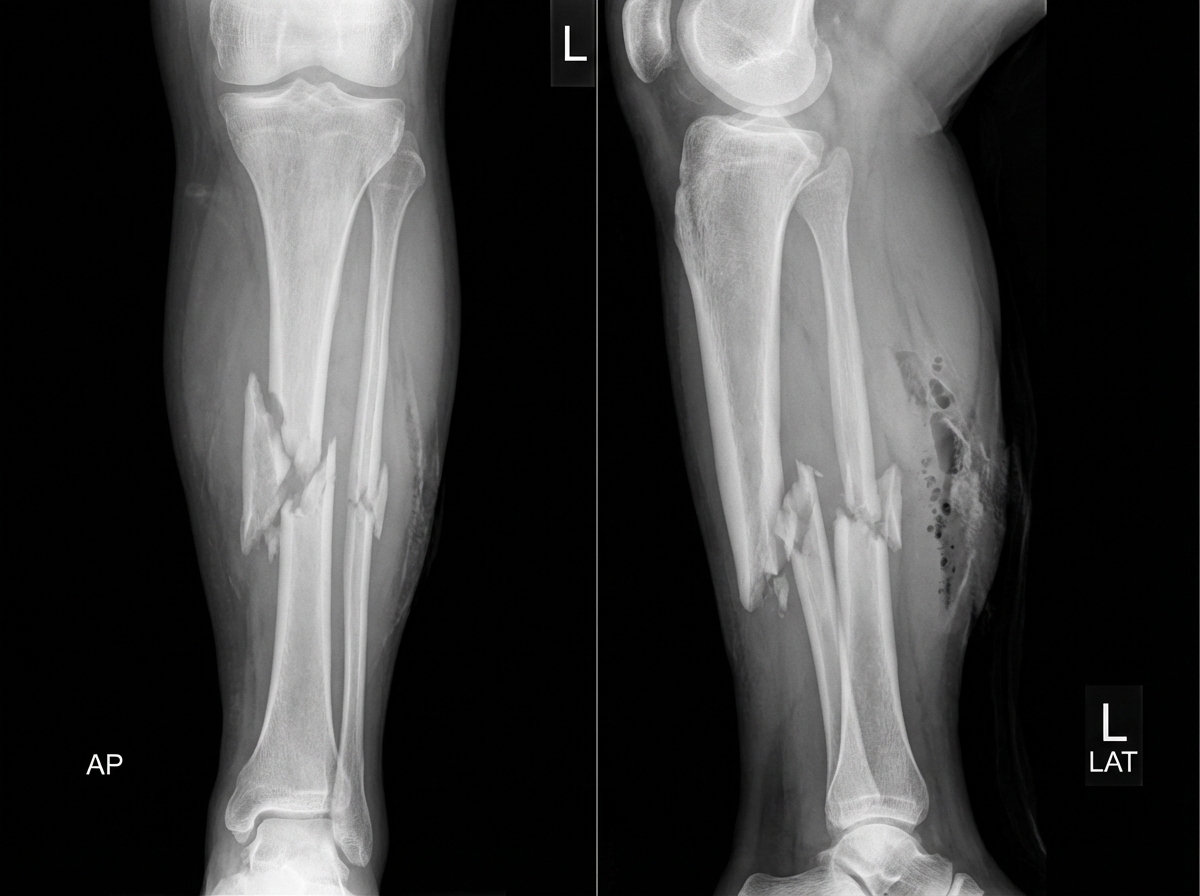
A 22-year-old man is brought to the emergency department following a rugby injury. Which of the following statements is false regarding the fracture shown?
What is the maximum weight typically allowed in skeletal traction?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
