Trauma — MCQs

On this page
In a 70-year-old lady with an intracapsular fracture of the neck of femur, what is the ideal treatment?
Which of the following statements is not true regarding traction?
Meyer's procedure is a method for treatment of which of the following conditions?
A 5-year-old boy presents with a fracture in the shaft of the humerus. How will you exclude the involvement of the radial nerve?
Banka's lesion is seen at which anatomical location?
Inversion injury at the ankle can cause all of the following injuries except?
Which is the most commonly fractured carpal bone?
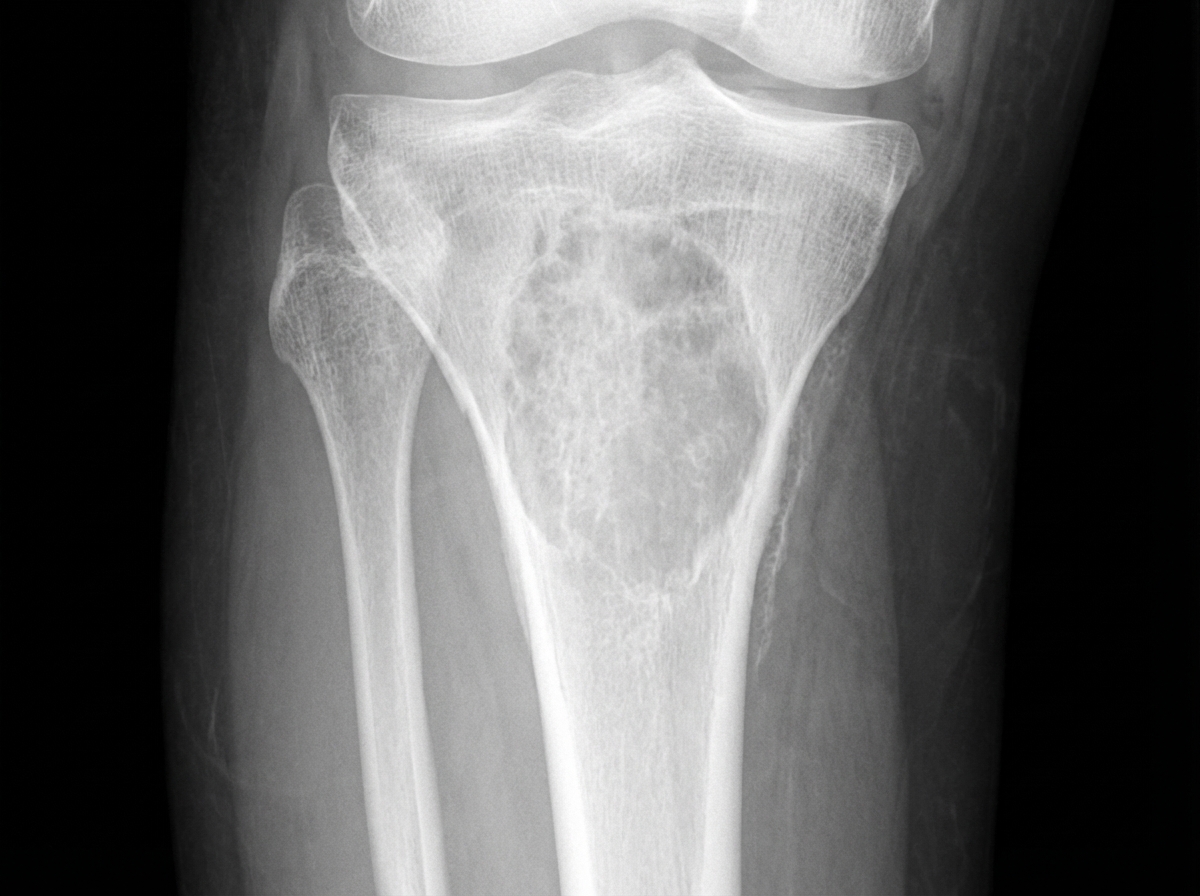
A 40-year-old female presented with severe pain in the left forearm and left ankle following trauma. She reported difficulty walking and swelling in her right upper leg. She also experienced ankle pain and painful ankle joint movements for approximately two years. Relevant abnormal biochemical parameters included: raised serum calcium (11.9 mg/dl), raised alkaline phosphatase (717 U/L), low inorganic phosphorus (1.3 mg/dl), and raised serum parathyroid hormone (1265 pg/l). Protein electrophoresis for M band was negative. An X-ray of the right leg is provided. What is the most likely diagnosis given the clinical presentation and biochemical findings?
A patient with anterior dislocation of the shoulder will most likely give a history of:
A 30-year-old male patient presents with breathlessness, irritability, and confusion. He has a history of a fracture of his right arm 3 days ago. On physical examination, a diffuse petechial rash is seen. Blood examination reveals thrombocytopenia. What is the most likely diagnosis for this patient?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
