Trauma — MCQs

On this page
Tardy ulnar nerve palsy is caused by which of the following?
Which of the following is NOT a type of displacement seen in a Colles fracture?
What is the primary action of an intramedullary 'K' nail?
An 8-year-old boy falls on a flexed left elbow and suffers a closed, fully displaced flexion type supracondylar fracture. He complains of finger numbness, but will not allow examination of his arm. Which of the following is most likely injured in this fracture?
What is a bumper fracture?
A 62-year-old woman presents with a 3-month history of progressive right shoulder pain, limiting her ability to lift her arm for daily activities. She denies neurological symptoms. Physical examination reveals weakness in abduction and external rotation with a normal passive range of motion. She cannot maintain 90 degrees of abduction. There is no motor deficit in the forearm or hand, and pulses and sensation are normal. Which of the following muscles constitute the injured structure?
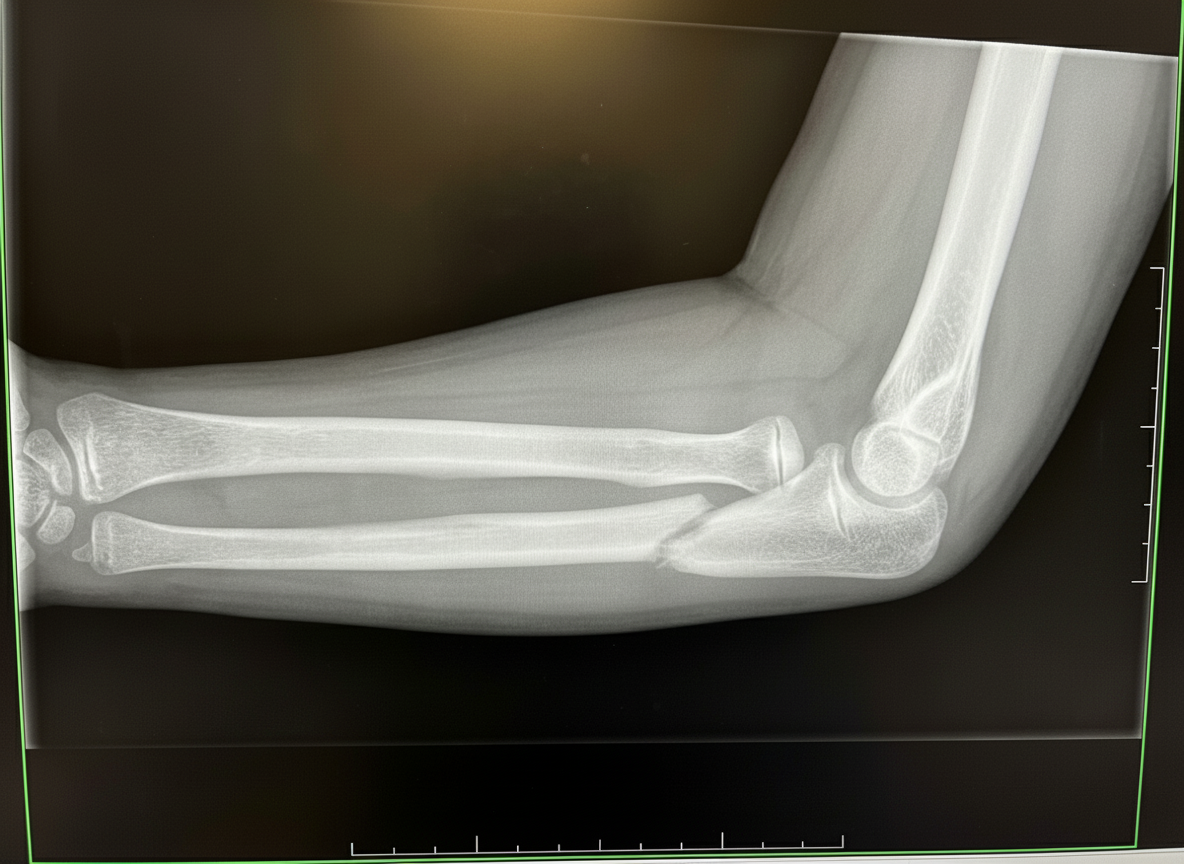
Which of the following best describes the patient's wrist fracture?
What is the typical position of the distal fragment in a fracture of the upper third of the femur shaft?
All of the following are true about dashboard injuries EXCEPT?
A 55-year-old woman presents with severe pain in the flexor muscles of the forearm, fixed flexion of the fingers, and swelling, cyanosis, and anesthesia of the fingers following a car crash. Which of the following is the most likely diagnosis?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
