Trauma — MCQs

On this page
"Dinner-fork" deformity is seen in which fracture?
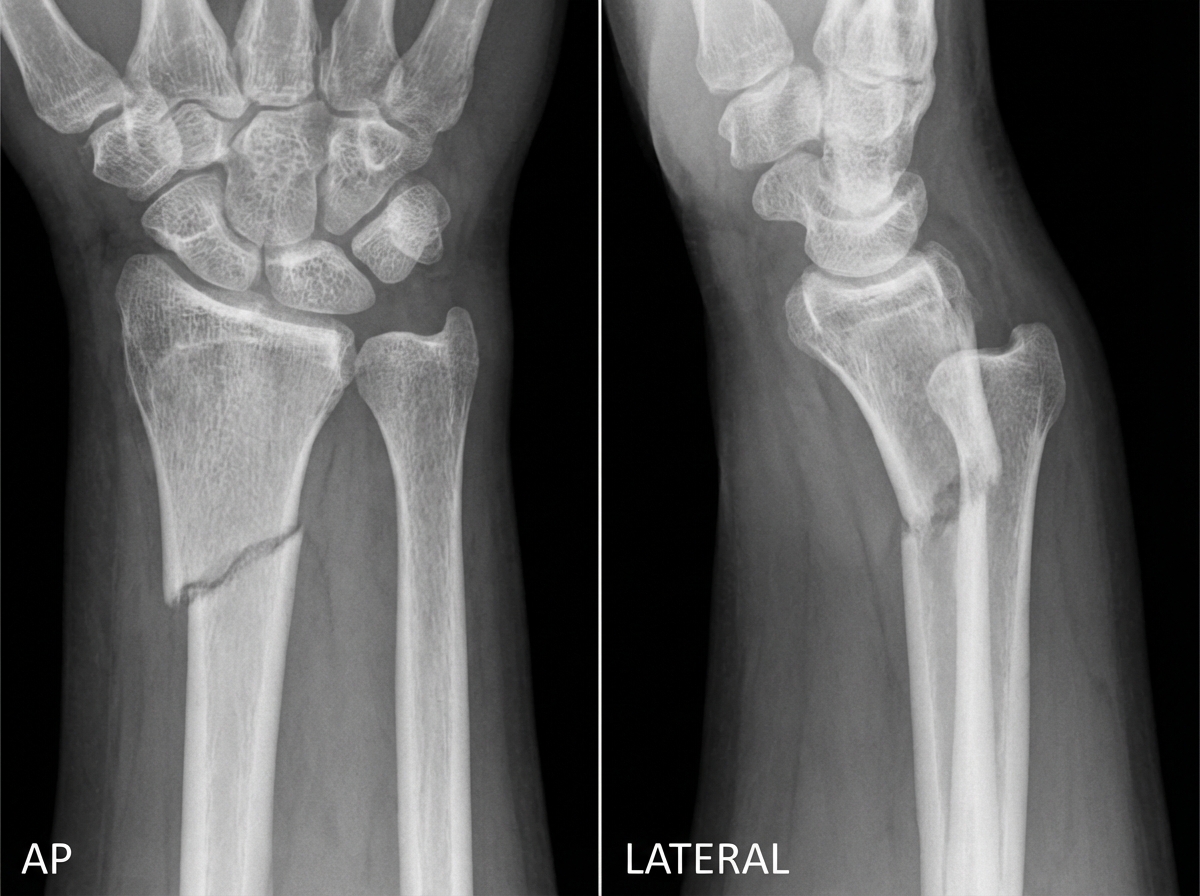
AP and lateral views of the wrist are provided. What is the diagnosis?
Volkmann's Ischaemic Contracture is due to which of the following?
All of the following are true about the clavicle, except:
Stress fracture is treated by:
The Lachman test is positive in which of the following conditions?
In some old fractures, cartilaginous tissue forms over the fractured bone end with a cavity in between containing clear fluid. What is this condition called?
Which of the following nerves is most commonly damaged during a wrist slash injury?
What is the most reliable test for an acutely injured knee in a 27-year-old athlete?
A 20-year-old male presents with anterior shoulder dislocation. This injury is usually caused as a combination of which of the following?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
