Trauma — MCQs

On this page
A young woman presented with mild quadriparesis following an accident. Her lateral X-ray of the cervical spine revealed a C5-C6 fracture-dislocation. What is the most appropriate line of management?
A 72-year-old man presents to the emergency room after sustaining a right knee injury in a car accident. The pain, which began shortly after the accident, progressed to severe swelling and excruciating pain, significantly impairing ambulation. Physical examination reveals a warm, swollen knee with an effusion that is extremely painful to flex. Radiographs of the knee exclude fracture. Arthrocentesis yields opaque fluid containing rhomboid crystals with weak-positive birefringence. What is the most appropriate next step in management?
Which nerve is commonly injured due to a lunate dislocation?
What is meant by Clergyman's knee?
A 32-year-old man involved in a motor vehicle accident sustained an injury to his left arm and complains of an inability to open his left hand and loss of sensation to a portion of his left hand. What is the most likely injury?
Which of the following fractures is known for non-union?
The management of fat embolism includes all of the following except?
A Bennet's fracture is difficult to maintain in a reduced position because of the pull of which muscle?
What is the recommended re-implantation time for a lower limb injury?
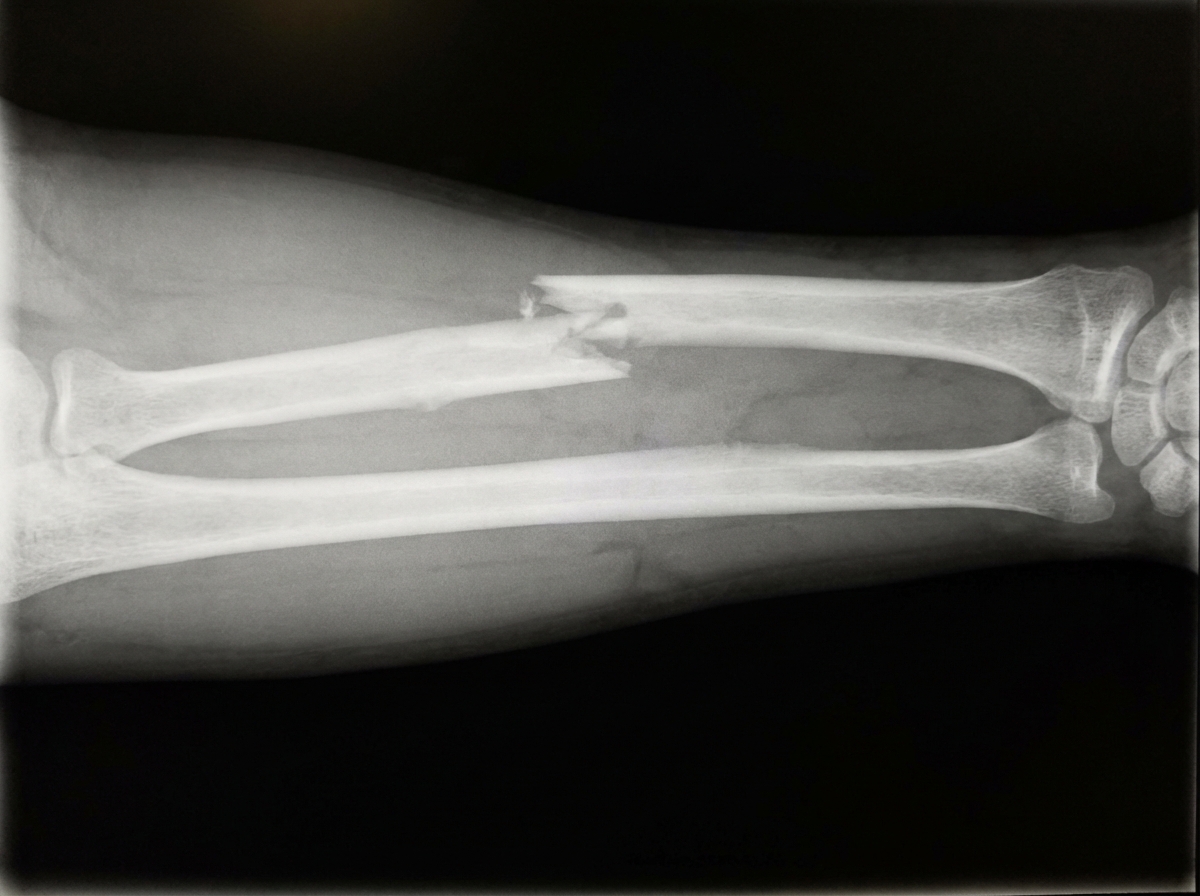
What is the management for the depicted condition?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
