Trauma — MCQs

On this page
Which of the following is the safest test to be performed in a patient with an acutely injured knee joint?
Which of the following statements regarding shoulder dislocation is true?
What is the treatment of choice for a one-week-old fracture of the neck of the femur in a 65-year-old patient?
Acute compartment syndrome is characterized by all of the following EXCEPT?
Which of the following statements regarding eponymous fractures is NOT TRUE?
A person with multiple injuries develops fever, restlessness, tachycardia, tachypnea, and periumbilical rash. What is the likely diagnosis?
Which of the following factors does NOT facilitate non-union of a fracture?
A 26-year-old male sustained a mid-arm injury, resulting in wrist drop, finger drop, and loss of sensation on the dorsum of the hand. The patient can perform elbow extension. What is the most likely diagnosis?
What is the most common site for spinal trauma?
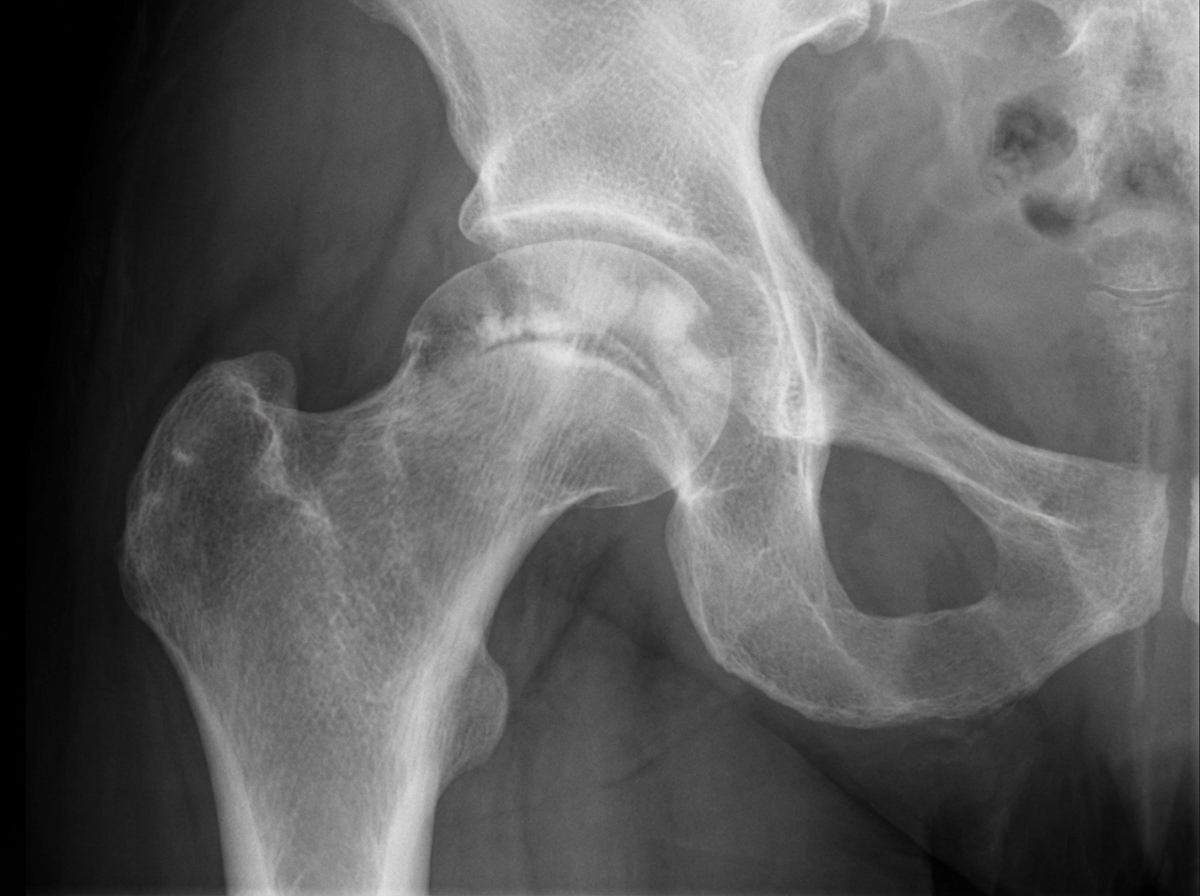
A 36-year-old woman with sickle cell disease presents with increasing pain in her right hip. She has no fever, chills, back or other bone pain, and there is no history of any trauma. On examination, her temperature is 37.3°C, range of motion in the right hip is reduced, she walks with a limp, and the right leg is shorter than the left. Movements of the hip and walking on it are painful. X-rays of the hip are shown. Which of the following is the most likely diagnosis?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
