Trauma — MCQs

On this page
Which of the following is true of fat embolism?
What is the permissible ischemia time for proximal limb amputations?
The femur is fractured at which location?
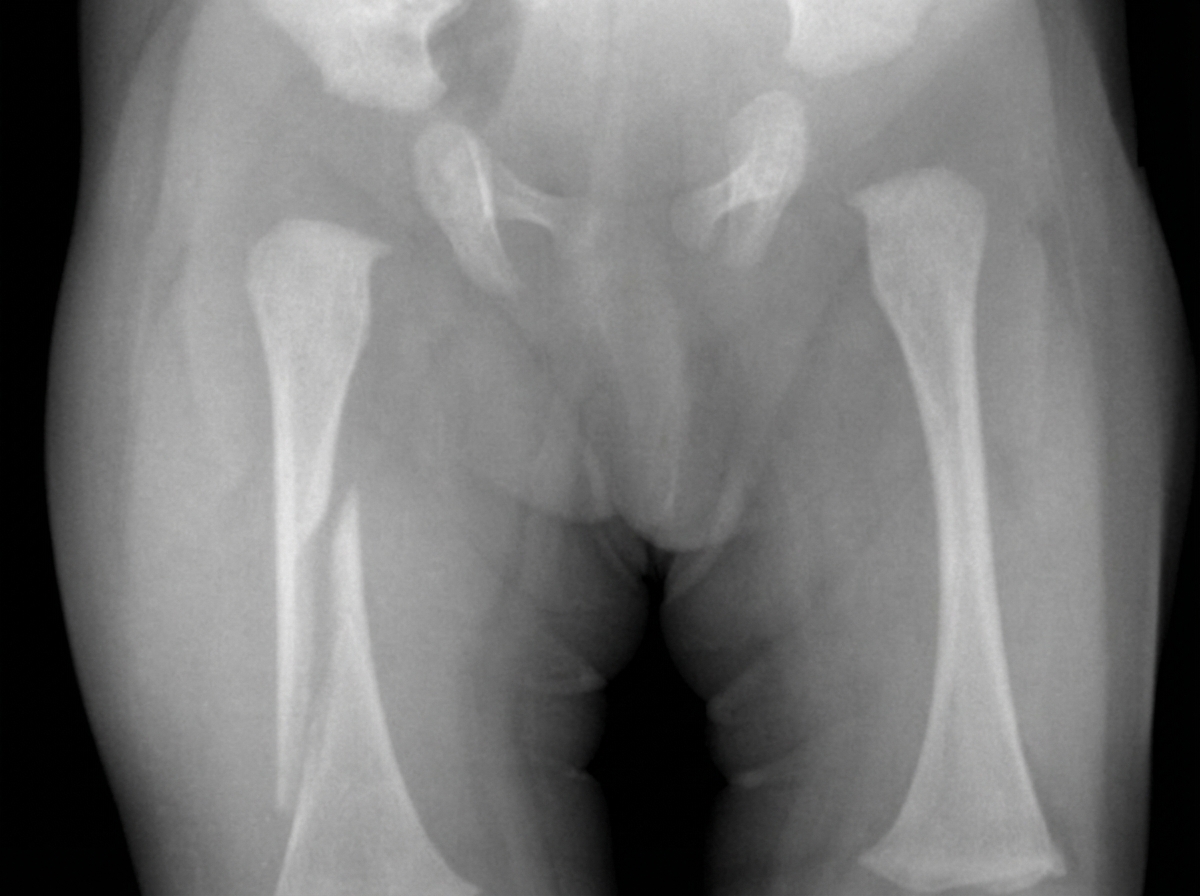
Three bony point relationship is maintained in which of the following conditions?
All of the following show compression osteosynthesis except:
Which condition presents with the vascular sign of Narath?
For which fracture is a tube (cylinder) cast typically applied?
Which of the following statements is true regarding fat embolism?
A 50-year-old male presented to the orthopedic OPD for regular follow-up, being treated for a forearm injury marked in a specimen. During examination, the doctor elicited a specific sign by tapping distal to the injury site, causing the patient to feel a tingling sensation. What is the rate of growth of the injured structure's stump?
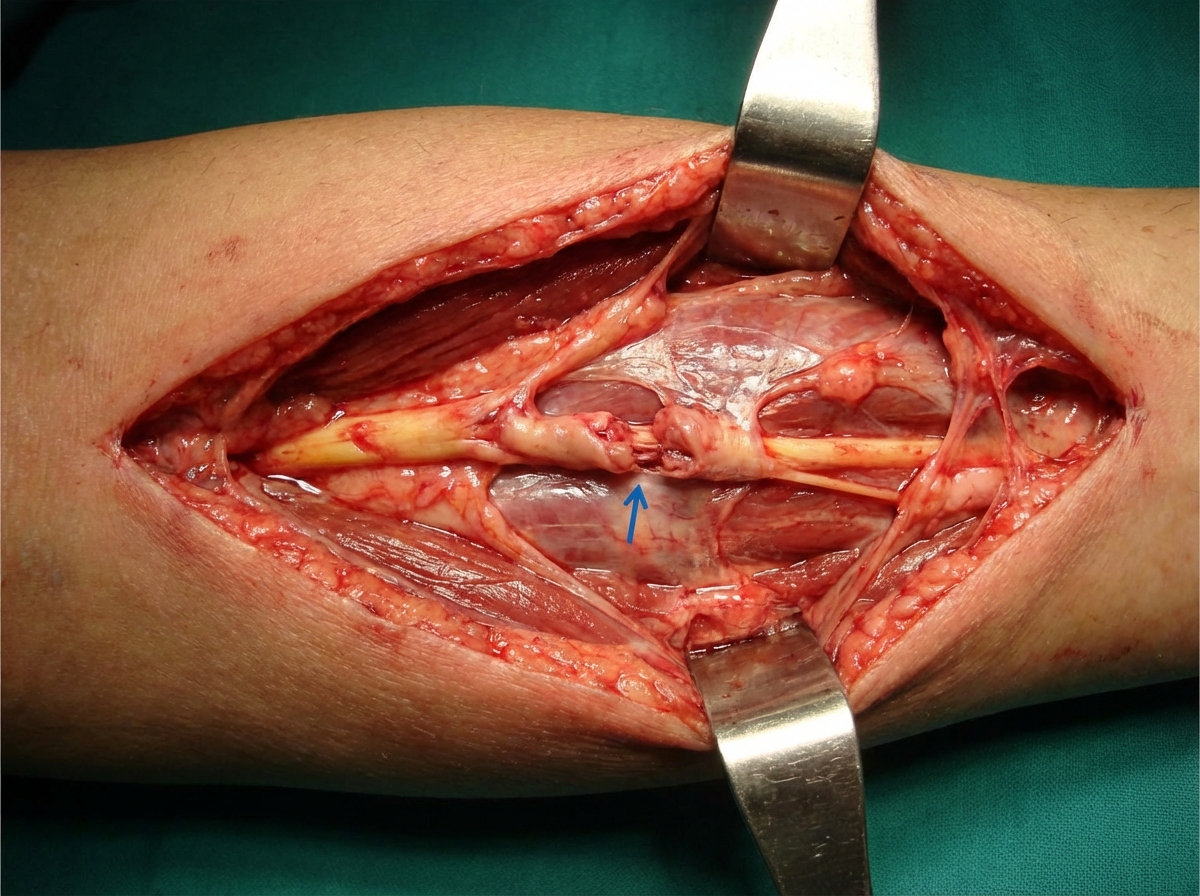
All of the following is true about thoracic outlet syndrome except?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
