Trauma — MCQs

On this page
What is the best diagnostic procedure for an anterior cruciate ligament injury?
Which of the following conditions shows the vascular sign of Narath?
What is Pauvel's angle?
Injury to which of the following structures would MOST likely account for the increased anterior translation of the tibia in reference to the femur?
Cubitus valgus deformity is a complication of which of the following?
What is the full form of SCIWORA?
The Maudsley test is performed to assess for which condition?
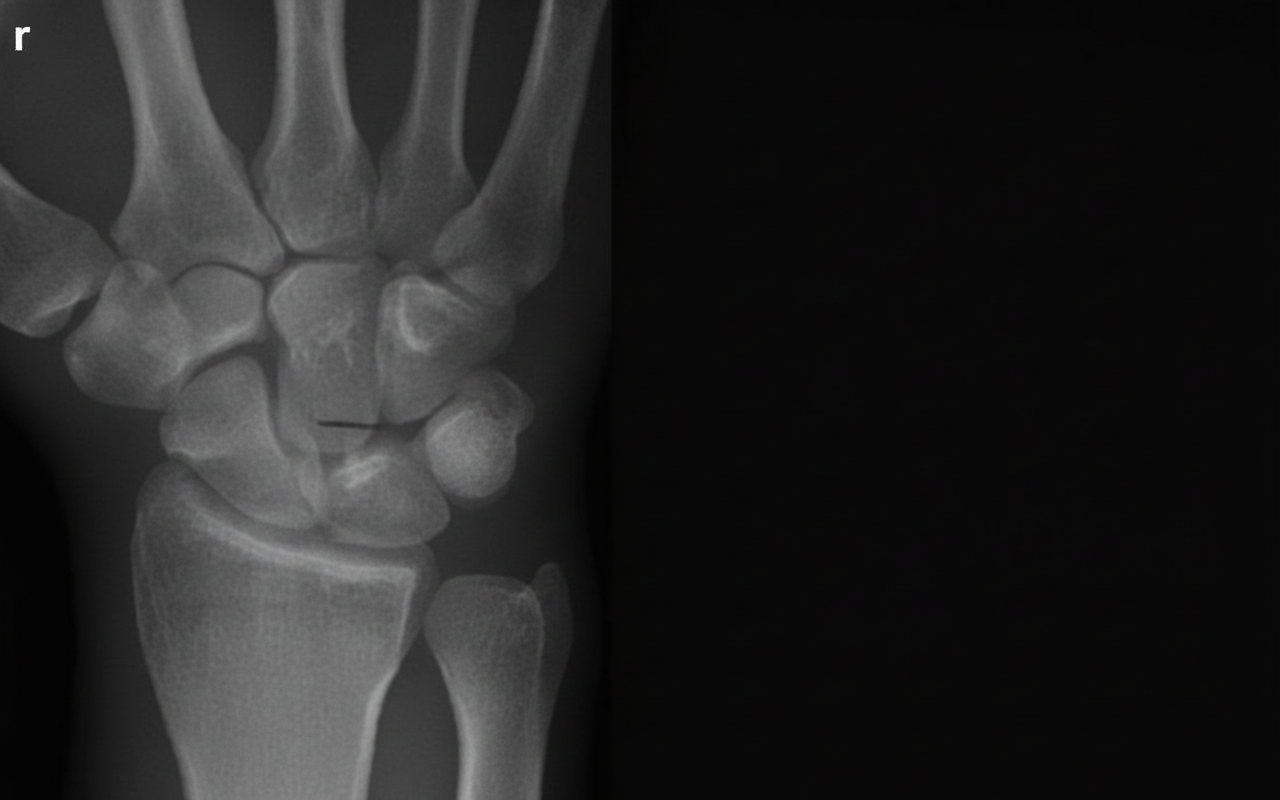
This diagnosis is?
What is the most common nerve injured in a posterior dislocation of the elbow?
Intramedullary fixation is ideal in a case of fracture of the shaft of the femur when there is which of the following conditions?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
