Trauma — MCQs

On this page
Which manoeuvre is used for diagnosing rupture of the medial collateral ligament?
What is the commonest complication of extra capsular fracture of the femur?
Regarding the displacement of the distal fragment in a Colles fracture, which statement is true?
Myositis ossificans is due to:
Sudeck's atrophy is more common in which of the following conditions?
Cock-up splint is used in which of the following conditions?
A man presents to the emergency department after an alcohol binge the previous night and sleeping in an armchair. In the morning, he is unable to move his hand and a diagnosis of ulnar palsy is made. What is the next line of management?
Which of the following is NOT a complication of Colles fracture?
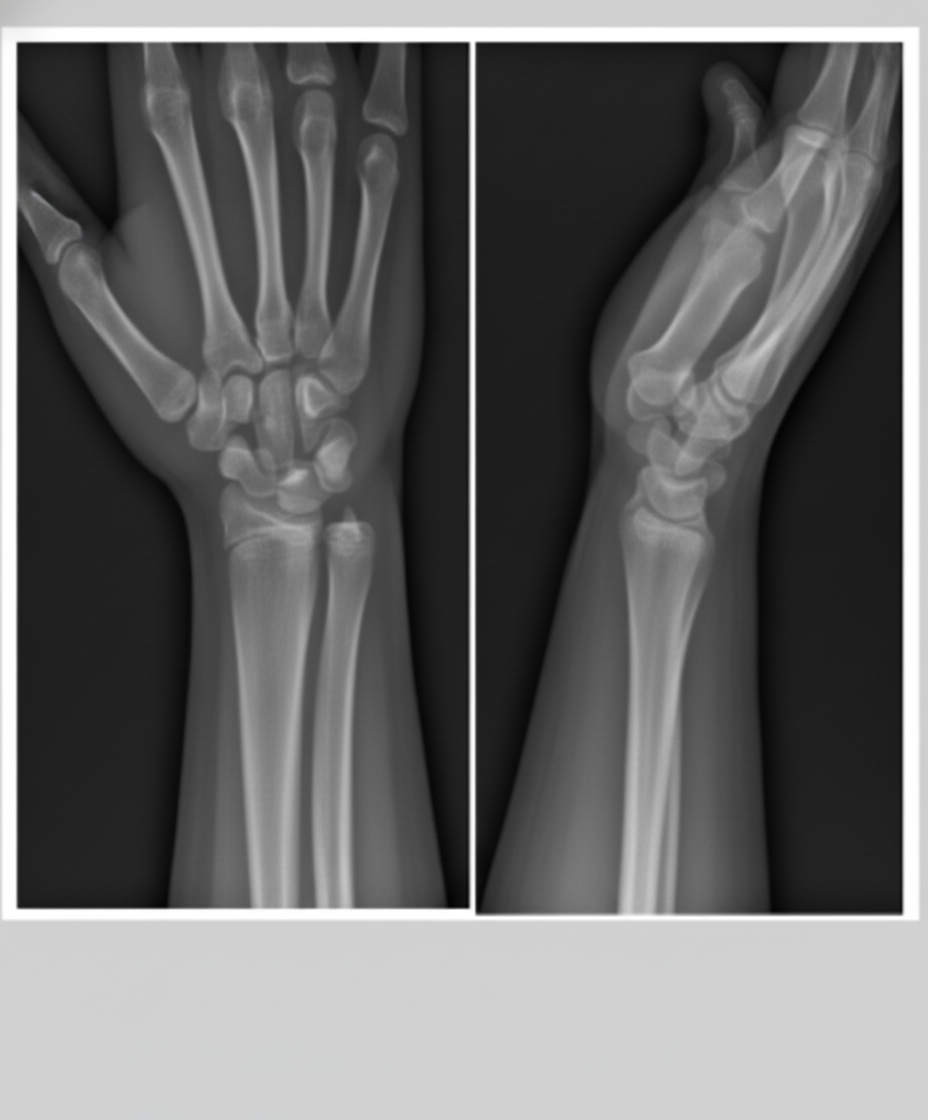
A boy fell from a height onto his outstretched hand. The X-ray of his forearm is shown below. What is the most likely diagnosis?
A 20-year-old male patient presented with acute pain in the left hip region and inability to bear weight on the left hip. On examination, deformity of the left lower limb was noticed. The lower limb was in slight flexion, adduction, and internal rotation. The patient gave a history of a road accident with sudden braking. Neurovascular examination was normal. Which of the following x-rays will most likely correspond to the above condition?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
