Trauma — MCQs

On this page
A patient develops compartment syndrome (swelling, pain, and numbness) following manipulation and plaster for a fracture of both bones of the leg. What is the best treatment?
Which anatomical compartment is involved in De Quervain's tenosynovitis?
A fracture of the neck of the fibula is most likely to result in injury to which nerve?
Which of the following complications occurs commonly in the fracture shown in the X-ray, EXCEPT?
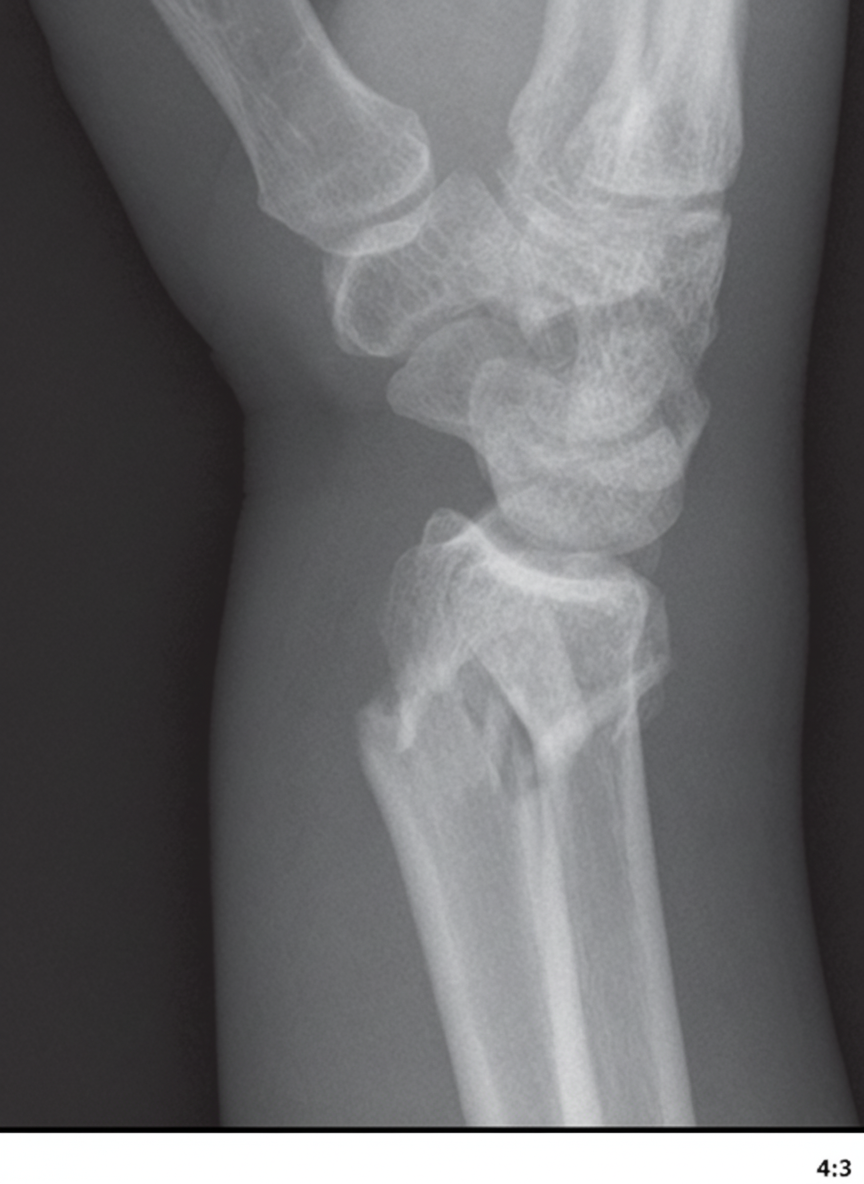
Which statement is NOT true about thoracic outlet syndrome?
What is a comminuted depressed fracture of the lateral tibial condyle classified as?
Which X-ray view is best for evaluating a patellar fracture?
Garden I fractures are also known as?
In myositis ossificans, where is mature bone typically seen?
A 67-year-old woman presents with a 3-month history of increasing right shoulder pain, resulting in an inability to lift her arm to brush her hair or retrieve items from shelves. She denies numbness, tingling, or pain radiation down her arm. Physical examination reveals weakness in abduction and external rotation of her right arm, with a normal passive range of motion. She is unable to hold her arms abducted to 90 degrees on the right side. There is no motor weakness, normal pulse, and normal sensation in her right upper extremity. Which of the following is the most likely diagnosis?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
