Trauma — MCQs

On this page
Which mechanism of injury is most commonly associated with ankle joint injuries?
Which of the following fractures is known for non-union?
What is the most common cause of neurological deficit in the upper limb?
In a supra condylar fracture of the humerus, which nerve is most commonly injured?
Seddon grading is used for what purpose?
Avascular necrosis is a known complication of which of the following fractures?
Hoffman Tinel sign is seen in?
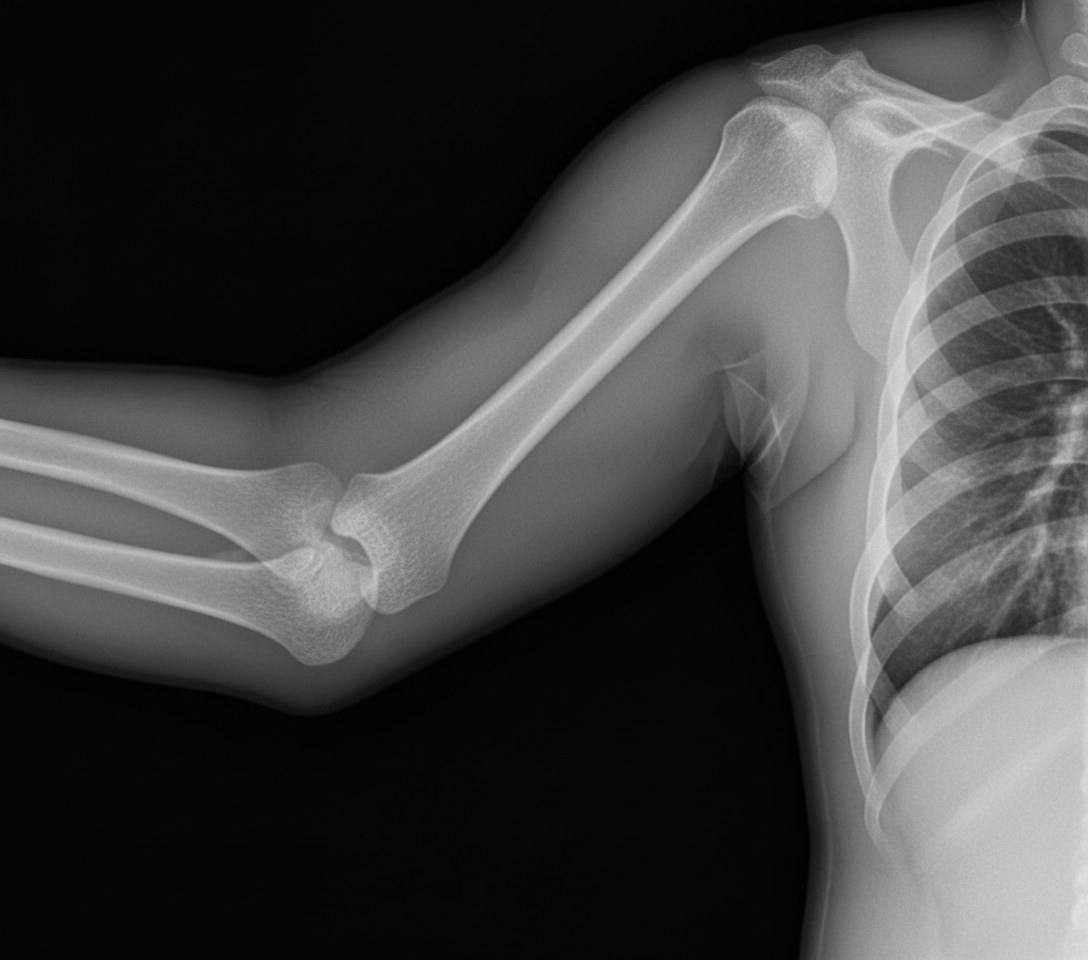
An 18-year-old male presents with a history of trauma. An X-ray is shown below. What is the diagnosis?
A 55-year-old woman presents with a traumatic injury to her right thigh. Which of the following findings is most sensitive for the diagnosis of compartment syndrome?
In lower-third fractures of the shaft of the femur, which displacement does the proximal fragment undergo?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
