Trauma — MCQs

On this page
What is a Colles' fracture a fracture of?
Arrange the following nerves according to the incidence of their involvement in a supracondylar fracture of the humerus:
What is the most important factor in fracture healing?
A patient operated for a forearm fracture under general anesthesia with a tourniquet was unable to move his fingers and had sensory loss over the entire hand postoperatively. What is the most common type of nerve injury in this scenario?
What is the X-ray diagnosis?
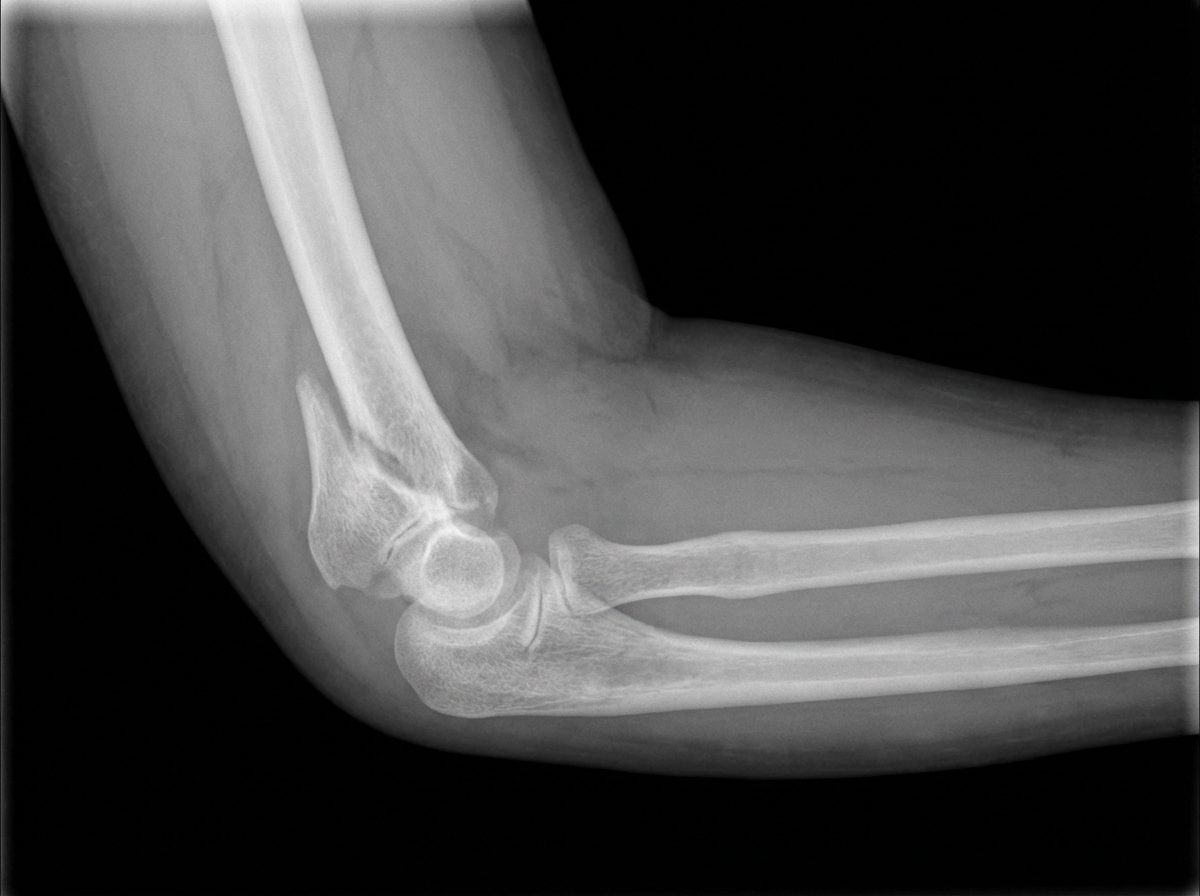
A 25-year-old man presents with a blue right arm with absent radial pulse and painful passive finger extension following a supracondylar fracture of the humerus. What condition is he most likely suffering from?
A Tillaux fracture involves which part of the bone?
What is a crescent fracture?
Tinel's sign indicates which of the following?
What is Neurapraxia?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
