Trauma — MCQs

On this page
A 30-year-old biker sustained a compound fracture of the leg following a road traffic accident. The fracture has been classified as Gustilo-Anderson type IIIB. Which of the following best represents this injury classification?
Fracture of the neck of the humerus is common in:
Trauma to a nerve resulting in paresthesia is termed as:
In fracture shaft of femur, which nail is commonly used for ORIF?
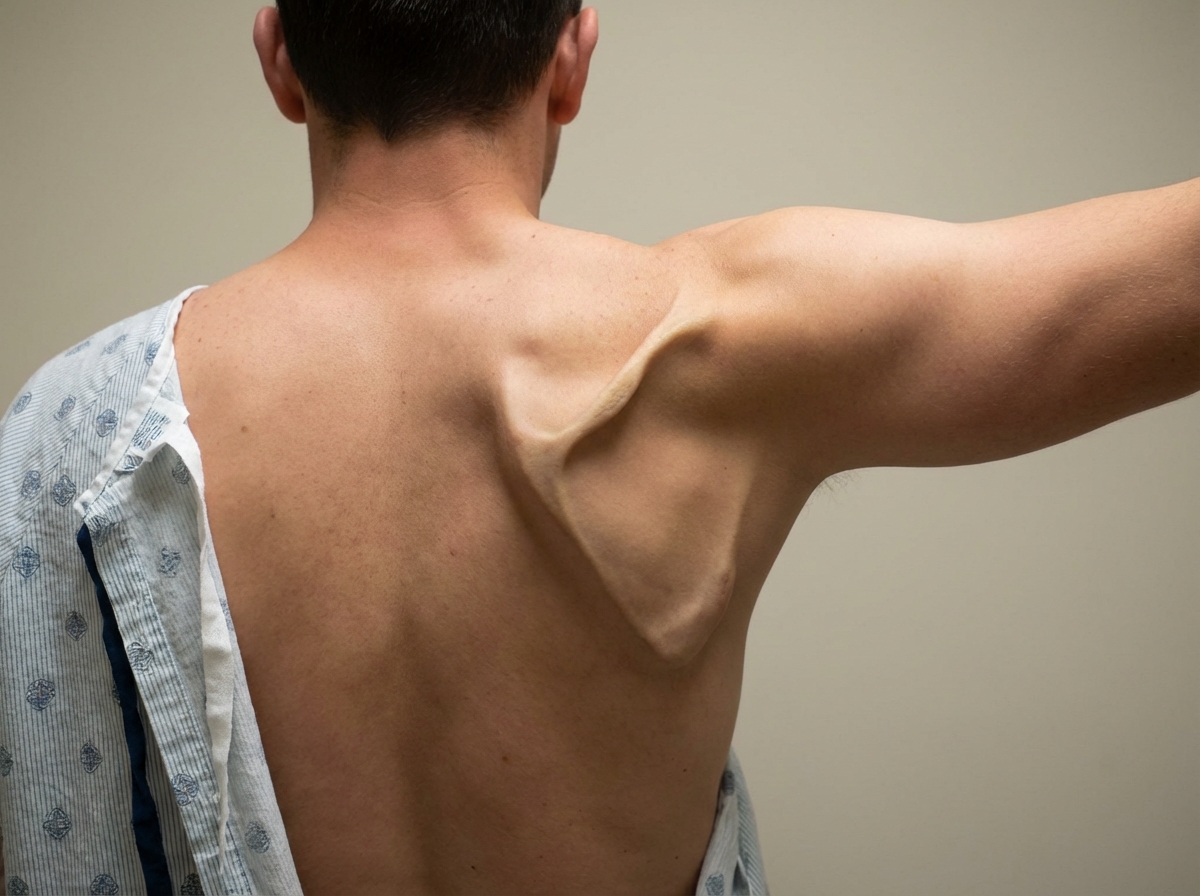
Which nerve is involved in this deformity?
Open book and bucket handle injuries are seen in which anatomical region?
In ankle sprain, which is the most commonly torn ligament?
The Judet and Lectournal classification is used for which type of fracture?
What is the most common fracture in childhood?
Which of the following is a false statement regarding Patellofemoral stress syndrome?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
