Trauma — MCQs

On this page
Functional cast bracing not used in fracture of ?
Most common complication of mid shaft humerus fracture is ?
Which of the following factors does NOT indicate an unstable pelvis?
Garden's classification used for which fracture?
Thomas splint is used for immobilizing fractures of ?
Which part of scaphoid fracture is most susceptible to avascular necrosis?
An RTA patient presented to the emergency department with severe pain in the ankle. An X-ray was performed, given below. What is the best next step in management?
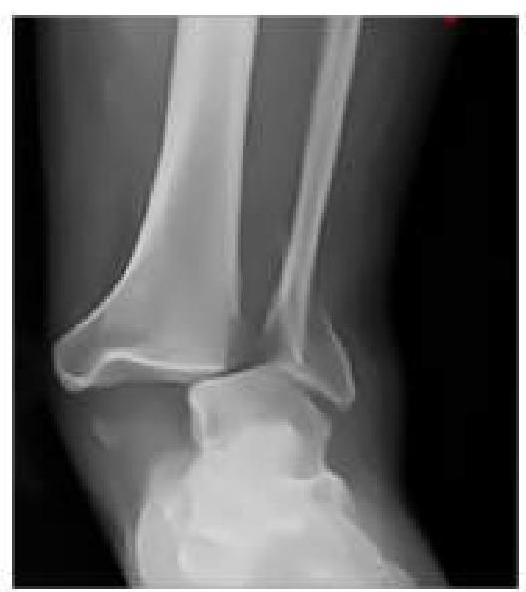
As an intern in the emergency department, you encounter four patients with different types of fractures. Which patient should you prioritize for orthopedic consultation based on the severity of their condition?
Identify the bone numbered in the X-ray that most commonly fractures when a person falls on outstretched hands.
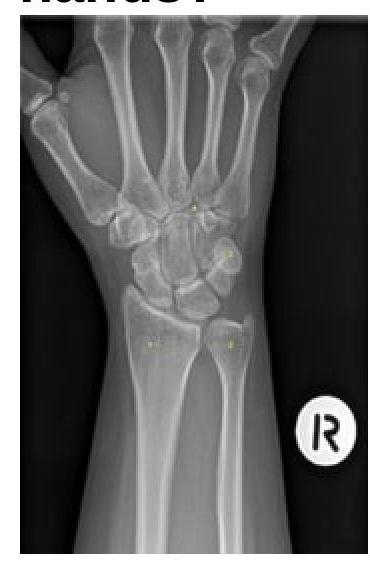
What is meant by perilunate dislocations?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
