Trauma — MCQs

On this page
What is the typical union time for a fracture of the femoral shaft in an adult?
Inability to touch the opposite shoulder in a dislocated shoulder is known as which test?
Adson's test is positive in which condition?
What is the recommended dose of methylprednisolone for acute spinal cord injury?
A bumper fracture is defined as which of the following?
All of the following are classifications of C-spine injury except which one?
What is the typical position of the leg in a fracture of the neck of the femur?
Management of calcaneal fractures depends upon which of the following?
Which nerve is most at risk in the injury shown in the accompanying radiograph?
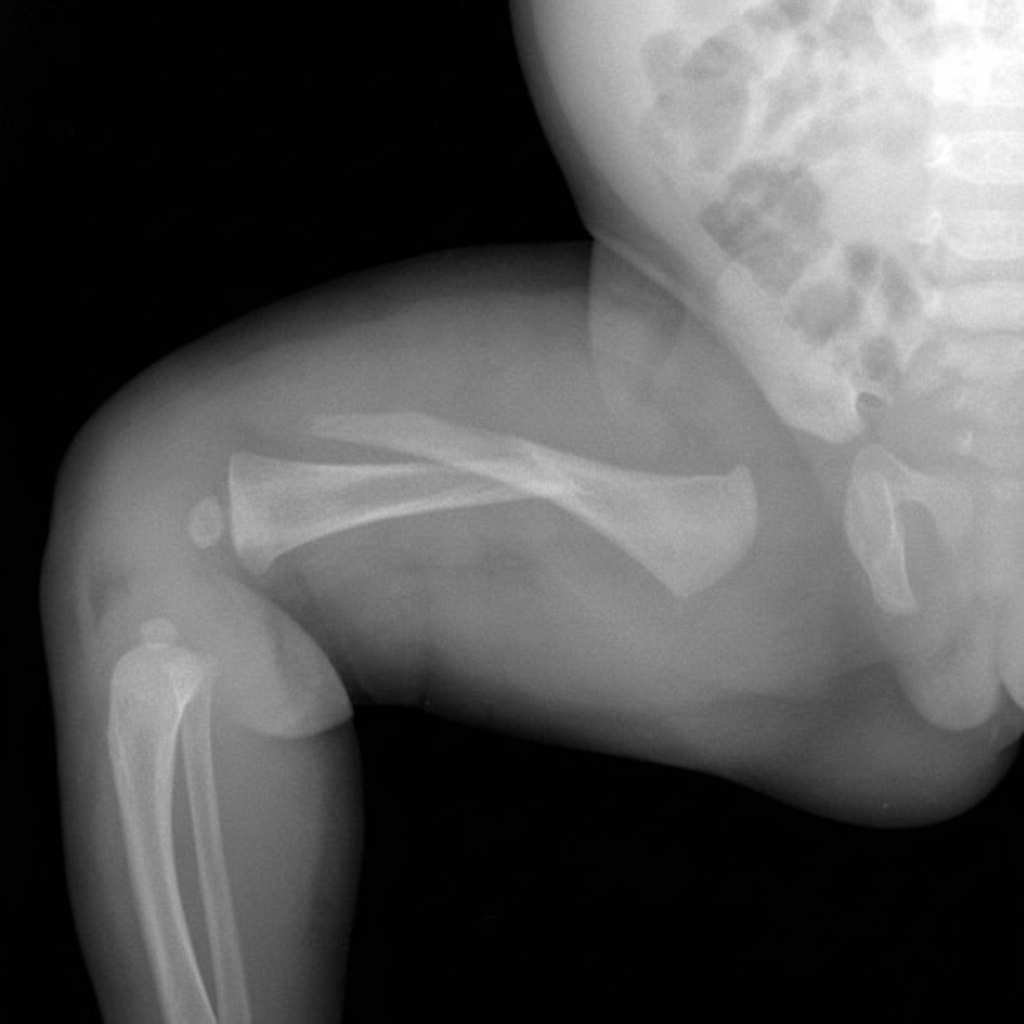
A 30-year-old male who is positive for HIV and on antiretroviral therapy presents with pain in the right hip region. He has had a flexion, abduction, and external rotation deformity of the right hip for 2 months. What is the most likely diagnosis?
Practice by Chapter
Principles of Fracture Management
Practice Questions
Upper Limb Fractures
Practice Questions
Lower Limb Fractures
Practice Questions
Spinal Trauma
Practice Questions
Pelvic and Acetabular Fractures
Practice Questions
Open Fractures
Practice Questions
Fractures in Children
Practice Questions
Fracture Complications
Practice Questions
Nonunion and Malunion
Practice Questions
Polytrauma Management
Practice Questions
Joint Dislocations
Practice Questions
Soft Tissue Injuries
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
